Uterine or Ovarian Enlargement in patients with breast cancer
Enlargement of the uterus or ovaries is a frequent reason for referral of breast cancer patients to the Gynecologic Oncology Center. In many cases, the enlargement is detected on an abdominal-pelvic computed tomography scan obtained for staging or follow-up purposes.
Uterine Enlargement
The most common cause of uterine enlargement is leiomyoma, which is found in approximately 20-25% of women of reproductive age and approximately 50% of postmenopausal women. Leiomyomata are usually asymptomatic. Unless the disease is symptomatic or the size of the uterus has increased rapidly, patients with leiomyoma should simply be reassured and should not be subjected to surgical intervention. A sudden increase in the size of the uterus or pain associated with leiomyoma should raise concern about the possibility of leiomyosarcoma. However, such tumors are rare, occurring in less than 0.2% of all patients with leiomyoma.
If leiomyoma causes enlargement of the uterus or excessive bleeding, a total hysterectomy may be required for therapeutic or, occasionally, for diagnostic purposes.
Ovarian Enlargement
The most common cause of ovarian enlargement is an ovarian cyst.
Ovarian cysts can be classified as either nonneoplastic or neoplastic.
Nonneoplastic ovarian cysts include physiologic cysts, such as corpus luteum and endometriotic cysts. The most common neoplastic ovarian cysts are cystic teratoma (dermoid cyst), which is usually found in younger patients, and serous or mucinous cystadenoma, which occurs in patients of all ages.
In women of reproductive age, the ovaries may enlarge slightly in parallel with physiologic effects of pituitary ovarian stimulation. Physiologic ovarian cysts are simple cysts, usually unilocular on sonography. Physiologic cysts may regress by the next menstrual cycle but sometimes persist for two or more cycles. Of note, data from the Breast Cancer Prevention Trial (Chalas et al., 2005) showed that there was an increased incidence of benign ovarian cysts in women taking tamoxifen (relative risk, 1.5).
If an ovarian cyst is more than 5 cm in diameter or if there is any palpable enlargement after menopause, the possibility of a neoplastic event should be considered.
The initial evaluation should include a thorough history that specifically addresses menstrual history, sexual history, family history, tamoxifen usage, neurologic history, and associated symptoms. This is followed by a comprehensive physical examination, with the pelvic examination being the primary focus.
The goal is to look for evidence of a pelvic mass and to determine the consistency (solid or cystic), mobility (mobile or fixed), and size of any such mass. Dysmenorrhea, dyspareunia, or pain that radiates to the upper thigh, with or without a history of endometriosis, may suggest a diagnosis of endometriosis. Pain associated with an enlarged ovary is usually related to a benign process except in the case of a rapidly growing or necrotic neoplasm of the ovary, such as a sarcoma or granulosa cell tumor.
Vaginal sonography can provide useful information about the size and complexity of an ovarian mass (Figure 15-4). Multiloculation, excrescences, and increased Doppler flow (low impedance) should increase the suspicion of a neoplasm.
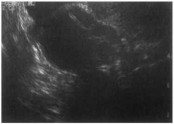 Figure 15-4. Ovarian mass identified on vaginal sonography.
Figure 15-4. Ovarian mass identified on vaginal sonography.
Even in the case of ovarian cysts less than 5 cm in diameter, sonography may be helpful in determining whether the cyst is simple, unilocular, or multilocular.
An elevated serum CA-125 value may suggest underlying pathology, although the CA-125 value is normal in up to 50% of patients with early-stage ovarian cancers. Moreover, even though CA-125 is used as a marker for epithelial ovarian cancer, levels of this marker may also be significantly elevated in patients who have uterine fibroids, adenomyosis, endometriosis, or any type of inflammation of the pleura or peritoneum; in patients with cirrhosis of the liver; and in 5-7% of women with no abnormalities. If the CA-125 value is elevated and the likelihood of a malignancy as indicated by other factors is low, the patient can be observed and the CA-125 value measured again two weeks later.
Ovarian cysts less than 5 cm in diameter that do not appear to be multiloculated on sonography can be managed conservatively. Conservative management should include serial clinical examinations and repeat vaginal sonography, which is generally performed approximately 8 weeks after initial sonography.
Complex ovarian cysts, ovarian cysts larger than 5 cm in diameter and ovarian cysts that increase in size usually require surgical exploration, primarily to rule out a neoplastic cause. In patients who have had breast reconstruction with a transverse rectus abdominis myocutaneous flap, appropriate surgical intervention may be carried out using a laparoscopic approach or midline abdominal laparotomy approach. It should be emphasized that these are general guidelines and do not replace good clinical judgment in the individual patient.
It is important to recognize that the ovaries and other genital-tract organs can be the site of metastases from breast cancer. If one or both ovaries are replaced by solid masses, especially when radiologic findings indicate metastases in the abdomen or elsewhere, percutaneous needle biopsy of the ovaries under computed tomographic guidance provides rapid and useful information without the need for surgical intervention. If ovarian metastases from breast cancer cause symptoms (pain, bladder pressure, or constipation) or contribute to obstruction of the small or large bowel, abdominal surgery may be necessary to correct the problem.
If the patient is asymptomatic and ovarian metastases from breast cancer are confirmed, tumor-reductive surgery is not generally favored over additional systemic therapy unless it can be demonstrated with high certainty that the cancer is localized to pelvic organs and that hysterectomy or oophorectomy alone will remove most of the metastatic disease. If the patient is experiencing pain secondary to the ovarian metastasis or if radiation therapy or chemotherapy is not an option for the patient, palliative surgery can be considered.
Elizabeth R. Keeler, Pedro T. Ramirez, and Ralph S. Freedman
Committee on Gynecological Practice, the American College of Obstetricians and Gynecologists. Obstet Gynecol 2007