Health Centers > Cancer Health Center > Vaginal Cancer
Vaginal Cancer
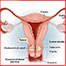
The vagina is a muscular tube that extends from the opening of the womb (cervix) to the folds of skin (vulva) between a woman's legs.
It allows blood from periods (menstruation) to pass out of the body, and is the passageway through which babies are born.
It is also called the "birth canal." The vagina connects the cervix (the opening of the womb, or uterus) and the vulva (the external genitalia).
Essentials of diagnosis
- Asymptomatic: abnormal vaginal cytology.
- Early: painless bleeding from ulcerated tumor.
- Late: bleeding, pain, weight loss, swelling.
General Considerations
Primary cancers of the vagina are rare, representing approximately 3% of gynecologic cancers. Approximately 85% are squamous cell cancers, and the remainder, in decreasing order of frequency, are adenocarcinomas, sarcomas, and melanomas. A tumor should not be considered a primary vaginal cancer unless the cervix is uninvolved or only minimally involved by a tumor obviously arising in the vagina. By convention, any malignancy involving both cervix and vagina that is histologically compatible with an origin in either organ is classified as cervical cancer.
Vaginal cancer is a rare cancer that occurs in your vagina - the muscular tube that connects your uterus with your outer genitals. Vaginal cancer most commonly occurs in the cells that line the surface of your vagina, which is sometimes called the birth canal.
While several types of cancer can spread to your vagina from other places in your body, cancer that begins in your vagina (primary vaginal cancer) is rare.
Women with early-stage vaginal cancer have the best chance for a cure. Vaginal cancer that spreads beyond the vagina is much more difficult to treat.
Malignant diseases of the vagina are either primary vaginal cancers or metastatic cancers from adjacent or distant organs. Primary vaginal cancers are defined as arising solely from the vagina, with no involvement of the external cervical os proximally or the vulva distally. The importance of this definition lies in the different clinical approaches to the treatment of upper and lower vaginal cancer.
According to the International Federation of Gynecology and Obstetrics (FIGO), a vaginal lesion involving the external os of the cervix should be considered cervical cancer and treated as such; a tumor involving both the vulva and the vagina should be considered vulvar cancer.
About 80% of vaginal cancers are metastatic, primarily from the cervix or endometrium. Metastatic cancer from the vulva, ovaries, choriocarcinoma, rectosigmoid, and bladder are less common. These cancers usually invade the vagina directly. Cancers from distant sites that metastasize to the vagina through the blood or lymphatic system also occur, including colon cancer, renal cell carcinoma, melanoma, and breast cancer.
Although primary vaginal carcinoma is a rare gynecologic malignancy, its impact on women's health should not be underestimated, especially when considering the demographic increase in elderly women. As more women survive past age 60 years, physicians need to consider the likelihood that more women will present with vaginal cancer.
Because the 5-year survival rate of treated early stage vaginal cancer is significantly higher than that of vaginal cancer in the advanced stages, early detection is key to improving treatment outcomes. To improve outcomes of primary vaginal carcinoma, select referral oncology centers should see additional cases per month in order to plan appropriate randomized, prospective studies. This would increase the experience of any of these centers in treating primary vaginal carcinoma.
Risk Factors
The etiology of vaginal cancer has not been identified. Note that vaginal cancer is not histologically homogeneous; several types of lesions exist, each with its own characteristics, age predilection, aggressiveness, and prognosis. This suggests that a single etiologic factor is unlikely. Although some histologic types of vaginal cancer have been associated with exposure to certain agents, so far no clear cause-and-effect relationship has been found between any of those agents and vaginal carcinoma.
HPV and other infectious agents
The identification of HPV deoxyribonucleic acid (DNA) in squamous cell cancer cells by in situ hybridization (21%) and southern blot hybridization (56%) strongly suggests a possible role for HPV in the pathogenesis of squamous cell vaginal carcinoma.
HPV subtypes 16 and 18 have the highest oncogenic potential and are most commonly linked to dysplastic changes in the female genital tract. Because HPV is sexually transmitted, this association raises the question as to whether women who engage in high-risk sexual behaviors, such as sex with multiple partners, are at risk for developing vaginal cancer.
Another association that strengthens the link between HPV infection and vaginal cancer is the presence of a premalignant lesion in the vagina, known as vaginal intraepithelial neoplasia (VAIN). Aho and coworkers reported that 5-9% of patients treated for VAIN progressed to invasive carcinoma. This suggested that VAIN may be a precursor to vaginal cancer even though the incidence of VAIN in the United States is 0.2-0.3 per 100,000 women , which is less than the incidence of diagnosed vaginal cancer. This is because of the fact that women with VAIN are usually asymptomatic and that screening for VAIN is not recommended for the general population. Still, the true malignant potential of VAIN needs to be clarified.
Other infectious agents that appear to be associated with vaginal cancer are herpes simplex virus (HSV) and Trichomonas vaginalis. In 2000, Lee and colleagues reported a case of rapidly progressive vaginal squamous cell carcinoma in a young woman with a 2-year history of human immunodeficiency virus (HIV) infection. They suggested that young women infected with both HIV and HPV are at increased risk for a more aggressive and less responsive vaginal cancer.
History of carcinoma
A history of cervical intraepithelial neoplasia (CIN), invasive cervical carcinoma, or invasive vulvar carcinoma has also been associated with vaginal carcinoma. Several studies indicate that up to 30% of patients with primary vaginal carcinoma have a history of in situ or invasive carcinoma that was treated at least 5 years before diagnosis.
Diethylstilbestrol
Diethylstilbestrol (DES), a drug previously used in the first trimester to prevent pregnancy loss, has a strong association with clear cell adenocarcinoma of the vagina. Herbst and colleagues first observed this association in 1971, which led to the discontinuation of DES that same year.
By 1987, the Registry for Hormonal Transplacental Carcinogenesis, established by Herbst and Scully, identified 524 women with clear cell adenocarcinoma, but only 60% had a history of DES exposure. Disease in the other 40% of patients with no history of DES exposure could be explained by recall bias or exposure to other unidentified factors. Women with in utero exposure to DES are at higher risk of developing adenocarcinoma than the general population. The estimated risk in these women is 1 in 1000.
Prior hysterectomy
Although 59% of women with vaginal cancer had a prior hysterectomy, in a 1986 report, Herman and colleagues demonstrated that when age and prior cervical cancer are controlled for, risk of vaginal cancer is not increased following hysterectomy for benign disease. Note that hysterectomy by itself is not a risk factor; rather, women who underwent hysterectomy were poorly monitored.
Age
In a 2004 publication, Hellman et al reviewed 341 cases of primary carcinoma of the vagina from 1956-1996 and suggested that the etiology of vaginal cancer may be age related. In younger women, the disease occurred in the upper part of the vagina and seemed to be related to cervical dysplasia and HPV infection, while in older patients, the tumors were exophytic. There was significant correlation with late menarche, suggesting hormonal factors and trauma to the vagina as probable etiologies.
Additional factors
Long-term pessary use and chronic irritation of vaginal mucosa in women with procidentia have been associated with vaginal cancer. Other predisposing factors include cigarette smoking, immunosuppressive therapy, chemotherapy, and radiation therapy. Approximately 10% of women diagnosed with primary vaginal carcinoma have a previous history of irradiation to the pelvis.
Pukkala and colleagues reported an association between low socioeconomic class in Finland and an increased incidence of cervical, endometrial, and vaginal cancer.
Secondary carcinoma of the vagina is seen more frequently than primary vaginal cancers. Secondary, or metastatic, tumors may arise from cervical, endometrial, or ovarian cancer, breast cancer, gestational trophoblastic disease, colorectal cancer, or urogenital or vulvar cancer. Extension of cervical cancer to the vagina is probably the most common malignancy involving the vagina. HPV, early hysterectomy, and prior radiation are possible risk factors for vaginal cancer, but no specific etiologic agent has been identified.
Signs and symptoms
The most common symptom of vaginal cancer is abnormal vaginal bleeding. This includes:
- bleeding between your normal periods, or after sex
- bleeding after the menopause (post-menopausal bleeding)
Other symptoms can include:
- smelly or bloody vaginal discharge
- pain during sex
- pain when urinating
- needing to urinate more frequently than usual
- blood in your urine
- pelvic pain
- an itch or lump in your vagina
See your GP if you experience any abnormal vaginal bleeding, changes in your usual pattern of periods (such as irregular periods or heavier periods than usual), or problems urinating.
While it's highly unlikely that these symptoms are caused by vaginal cancer, they should still be investigated by your GP. Read more about diagnosing vaginal cancer.
Pathology
Squamous cell carcinoma may be ulcerative or exophytic. It usually involves the posterior wall of the upper third of the vagina, but may be multicentric. Direct invasion of the bladder or rectum may occur. The incidence of lymph node metastases is directly related to the size of the tumor. The route of nodal metastases depends on the location of the tumor in the vagina. Tumors in the lower third metastasize like cancer of the vulva, primarily to the inguinal lymph nodes (Fig 49-8). Cancers of the upper vagina, which is the most common site, metastasize in a manner similar to cancer of the cervix. The lymphatic drainage of the vagina consists of a fine capillary meshwork in the mucosa and submucosa with multiple anastomoses. As a consequence, lesions in the middle third of the vagina may metastasize to the inguinal lymph nodes or directly to the deep pelvic lymph nodes.
- ENDOMETRIAL CANCER
- Etiology and Pathology
- Symptoms, Signs, and Diagnosis
- Staging, Prognosis, and Treatment
- OVARIAN CANCER
- Etiology and Pathology
- Symptoms, Signs, and Diagnosis
- Treatment
- CERVICAL CANCER
- Pathology
- Symptoms and Signs
- Diagnosis
- Prognosis and Treatment
- VULVAR CANCER
- Pathology
- Symptoms, Signs, and Diagnosis
- Prognosis
- Treatment
- VAGINAL CANCER
- Symptoms and Signs
- Prognosis and Treatment
- FALLOPIAN TUBE CANCER
- Symptoms, Signs, and Diagnosis
- GESTATIONAL TROPHOBLASTIC DISEASE
- Symptoms, Signs, and Diagnosis
- Treatment
Melanomas and sarcomas of the vagina metastasize like squamous cell cancer, although liver and pulmonary metastases are more common. Nevi rarely occur in the vagina; therefore, any pigmented lesion of the vagina should be excised or biopsied. The anterior surface and lower half of the vagina are the most common sites. Grossly, the tumors are usually exophytic and described as polypoid or pedunculated with secondary necrosis.
Sarcomas of the vagina occur in children younger than 5 years of age and in women in the fifth to sixth decades. Embryonal rhabdomyosarcomas or sarcoma botryoides, replace the vaginal mucosa of young girls and consist of polypoid, edematous, "grapelike" masses that may protrude from the vaginal introitus. Leiomyosarcomas, reticulum cell sarcomas, and unclassified sarcomas occur in older women. The upper anterior vaginal wall is the most common site of origin. The appearance of these tumors depends on the size and the extent of disease at the time of diagnosis.
Clear cell adenocarcinomas arise in conjunction with vaginal adenosis, which, in recent years, has been detected most frequently in young women with a history of exposure to diethylstilbestrol (DES) in utero (Fig 49-9). The Registry of Clear Cell Adenocarcinoma of the Genital Tract in Young Females was established in 1971 to study the clinicopathologic and epidemiologic aspects of these tumors in girls born in 1940 or later, the years during which DES was used during pregnancy. The risk of developing clear cell adenocarcinoma by age 24 years has been calculated to be 0.14-1.4 per 1000 exposed female fetuses. Adenosis vaginae and adenocarcinoma do occur in sexually mature and postmenopausal women.
Metastatic adenocarcinoma to the vagina may arise from the urethra, Bartholin's gland, the rectum or bladder, the endometrial cavity, the endocervix, or an ovary, or it may be metastatic from a distant site. Hypernephroma of the kidney characteristically metastasizes to the anterior wall of the vagina in the lower third. These tumors are not primary vaginal cancers.
Clinical Findings
Vaginal cancer is often asymptomatic, discovered by routine vaginal cytologic examination, and confirmed by biopsy after delineation of the location and extent of the tumor by colposcopy.
Postmenopausal vaginal bleeding and/or bloody discharge are the most common presenting symptoms. Approximately 50% of patients with invasive vaginal cancer report for examination within 6 months after symptoms are noted. Less commonly, advanced tumors may impinge upon the rectum or bladder or extend to the pelvic wall, causing pain or leg edema.
A diagnosis of primary cancer of the vagina cannot be established unless metastasis from another source is eliminated. A complete history and physical examination should be performed, including a thorough pelvic examination, cervical cytologic examination, endometrial biopsy when indicated, complete inspection of the vagina, including colposcopy, and biopsy of the vaginal tumor. Careful bimanual examination with palpation of the entire length of the vagina can detect small submucosal nodules not visualized during the examination.
The staging system for cancer of the vagina is clinical and not surgical (Table 49-2).
Screening
Routine screening
Routine screening for vaginal carcinoma is not justified for all patients, because it is not cost effective. Women at risk, however, particularly those with a history of cervical neoplasia and risky sexual behavior, should receive a Papanicolaou test on a regular basis.
Screening after hysterectomy
Screening women with previous hysterectomy is controversial. In 1990, Manetta and colleagues suggested that women with previous hysterectomy should be counseled to continue their gynecologic cancer surveillance program. They reported that 63% of patients who were diagnosed after the onset of their symptoms and who tended to have an unfavorable prognosis had undergone a prior hysterectomy.
In a 1996 report, however, Pearce et al reviewed 9,610 vaginal smears from 5,682 women who underwent hysterectomy for benign gynecologic diseases and found that the probability of an abnormal Papanicolaou smear in these women was 1.1%, with a 0% positive predictive value for detecting vaginal cancer. Similarly, in 2000, Videlefsky et al and Fetters et al concluded that routine vaginal cuff testing for most patients who underwent hysterectomy for benign conditions is not indicated.
The American College of Obstetricians and Gynecologists recommends discontinuing screening in women who have undergone hysterectomy for benign diseases who have no prior history of high-grade cervical dysplasia. Women with a history of CIN 2 or CIN 3 are at increased risk of developing recurrent dysplasia or carcinoma of the vaginal cuff; therefore, in these women and in those in whom a negative history of high-grade dysplasia could not be verified, screening after hysterectomy should continue.
Screening in women exposed to DES
Young girls who were exposed to DES in utero should be routinely examined starting at puberty or at the age of 14 years. Examination includes cytologic screening of the cervix and vagina, followed by careful inspection and palpation of the genital tract. Staining with half-strength Lugol iodine helps to mark areas of adenosis. As long as cytologic findings are negative, colposcopy is unnecessary.
How vaginal cancer is diagnosed
Usually you will begin by seeing your GP, who will refer you to a specialist doctor for tests, and for expert advice and treatment. The following tests are commonly used to diagnose vaginal cancers.
Internal vaginal examination
At the hospital, the specialist doctor will do a full pelvic examination. They will examine the inside of your vagina to check for any lumps or swellings. The doctor will also feel your groin and pelvic area to check for any swollen lymph nodes and may also check your back passage (rectum).
Cervical screening
You may have a liquid-based cytology test or smear test to see if there are any abnormalities in the cells of the cervix.
The person taking the liquid-based cytology or smear test should explain the procedure and you should feel able to ask questions at any time. Once you are lying comfortably on the couch, the doctor or nurse will gently insert an instrument called a speculum into the vagina, to keep it open while the smear is taken.
A special brush or small disposable spatula is then used to take a sample of cells from the cervix. The cells are then either put into a small container of preservative or placed on a glass slide, and sent to the laboratory for examination under a microscope.
Colposcopy
This is an examination of the vagina using a colposcope, which is a small, low-powered microscope.
The colposcope acts like a magnifying glass so the doctor or specialist nurse can see the whole vagina in more detail.
The doctor will use a speculum in the same way as in the screening test, to hold the vagina open. A liquid is then applied to the vagina that makes any abnormal areas show up more clearly. A colposcopy is usually carried out in the hospital outpatient department and takes about 10-15 minutes. It isn't usually painful but may be slightly uncomfortable.
Biopsy
A small sample of tissue will be taken from any abnormal areas. This sample will be examined under a microscope.
Differential Diagnosis
Benign tumors of the vagina are uncommon, are usually cystic, arise from the mesonephric (wolffian) or paramesonephric ducts, and are usually an incidental finding on examination of the anterolateral wall of the vagina (Gartner's duct cyst).
An ulcerative lesion may occur at the site of direct trauma, following an inflammatory reaction caused by prolonged retention of a pessary or other foreign body, or, occasionally, following a chemical burn. Granulomatous venereal diseases seldom affect the vagina but may be diagnosed with appropriate laboratory studies and a biopsy.
Endometriosis that penetrates the cul-de-sac of Douglas into the upper vagina cannot be differentiated from cancer except by biopsy.
Cancer of the urethra, bladder, rectum, or Bartholin's gland may penetrate or extend into the vagina. Cloacogenic carcinoma is a rare tumor of the anorectal region originating from a persistent remnant of the cloacal membrane of the embryo. The tumor accounts for 2-3% of anorectal carcinomas and occurs more than twice as often in women. Although these metastatic tumors often penetrate into the vagina as fungating or ulcerating lesions, they may present as a submucosal mass.
Biopsy should be performed to establish a histologic diagnosis.
Treatment
Following biopsy confirmation of disease, all patients should undergo a thorough physical examination and evaluation of the extent of local and metastatic disease. Pretreatment evaluation may include the following studies: chest radiography, intravenous pyelogram, cystoscopy, proctosigmoidoscopy, and CT scan of the abdomen and pelvis. The treatment of patients with invasive vaginal cancer primarily consists of combined external-beam and internal radiation therapy. In patients in whom coitus is an important factor, surgery should be considered. Also in patients with stages I and IIA lesions, radical hysterectomy with an upper vaginectomy may be performed. Therapy is complicated by the anatomic proximity of the vagina to the rectum, bladder, and urethra. Most primary invasive epidermoid cancers of the vagina are treated by irradiation. Irradiation consists of whole-pelvis external therapy supplemented by internal radiation treatment. Interstitial therapy is commonly used unless there exists a small vault lesion, which may be adequately managed by a tandem and ovoid implant.
A select group of patients with stage III or IV disease may benefit from preoperative whole-pelvic radiation followed by radical surgery. However, most affected patients are treated by irradiation, which consists of whole-pelvis external irradiation followed by intracavitary or interstitial implants, or additional external therapy through a treatment field that has been reduced in size and localized to the affected parametrium. In some cases, carcinoma at the introitus may be treated like cancer of the vulva, using radical vulvectomy and bilateral superficial and deep inguinal lymphadenectomy. A very small and early lesion may be treated by total vaginectomy. However, the close proximity of the bladder and the rectum often precludes conservative surgery. Irradiation is essentially the same as that used for cancers of the upper vagina. When the lower third of the vagina is involved, the inguinal nodes must be treated with either irradiation or inguinal lymphadenectomy.
The principles of treatment of primary adenocarcinoma of the vagina are the same as those for squamous cell cancer. However, preferred therapy for clear cell carcinoma of the vagina and cervix in young women has not been established. Approximately 60% of tumors occur in the upper half of the vagina, and the remainder occur in the cervix. The incidence of nodal metastases is approximately 18% in stage I and 30% or more in stage II disease. If the disease is found sufficiently early and is confined to the upper vagina and cervix, radical abdominal hysterectomy, upper vaginectomy, and pelvic lymphadenectomy with ovarian preservation can be performed. More advanced lesions are treated with irradiation.
Sarcoma botryoides, a variety of rhabdomyosarcoma, is usually seen in patients who are younger than 5 years of age. Radiation therapy or local excision has yielded poor results; thus, historically, pelvic exenteration was the standard of therapy. Primary chemotherapy with vincristine, actinomycin D, and cyclophosphamide plus radiation leads to excellent results in treating patients with this disease. Melanoma of the vagina may be treated with radiation, conservative excision, and/or radical surgery.
Gynecologic Cancers |
Epidermoid cancers that recur after primary radiation therapy are usually treated by pelvic exenteration. Chemotherapy for recurrent disease has been relatively ineffective, but multidrug regimens incorporating cisplatin may prove to be more useful.
Prognosis
The size and stage of the disease at the time of diagnosis are the most important prognostic indicators in squamous cell cancers. The 5-year survival rate is approximately 77% in patients with stage I disease, 45% in patients with stage II disease, 31% in patients with stage III disease, and 18% in patients with stage IV disease.
Melanomas (even small ones) are very malignant, and few respond to therapy. The tumor recurs locally and metastasizes to the liver and lungs. Chemotherapy and immunotherapy have been used as adjunctive treatment.
Too few sarcomas of the vagina have been reported to generate survival data. These tumors have a propensity for local recurrence and distant metastases, and the prognosis is usually poor.
REFERENCES
General
Berek JS: Novak's Gynecology. Philadelphia: Williams & Wilkins, 2002.
Preinvasive Disease of the Vulva & Vagina
Davis G, Wentworth J, Richard J: Self-administered topical imiquimod treatment of vulvar intraepithelial neoplasia. J Reprod Med 2000;45:619.
Hart WR: Vulvar intraepithelial neoplasia: Historical aspects and current status. Int J Gynecol Pathol 2001;20:116.
Hillemanns P et al: Integration of HPV-16 and HPV-18 DNA in vulvar intraepithelial neoplasia. Gynecol Oncol [2005; Epub ahead of print]. 2006;100:276.
Jones RW, Rowan DM: Spontaneous regression of vulvar intraepithelial neoplasia 2-3. Obstet Gynecol 2000;96:470.
Joura EA et al: Increasing incidence of vulvar intraepithelial neoplasia and squamous cell carcinoma of the vulva in young women. J Reprod Med 2000;45:613.
McNally OM et al: VIN 3: A clinicopathologic review. Int J Gynecol Cancer 2002;12:490.
Muderspach L et al: A phase I trial of a HPV peptide vaccine for women with high grade cervical and vulvar intraepithelial neoplasia who are HPV 16 positive. Clin Cancer Res 2000;6:3406.
Murta EF et al: Vaginal intraepithelial neoplasia: Clinical-therapeutic analysis of 33 cases. Arch Gynecol Obstet 2005;272:261.
Rome RM et al: Management of vaginal intraepithelial neoplasia: A series of 132 cases with long-term follow-up. Int J Gynecol Cancer 2000;10:382.
Cancer of the Vagina
Miner TJ et al: Primary vaginal melanoma: A critical analysis of therapy. Ann Surg Oncol 2004;11:34.
Samant R et al: Radiotherapy for the treatment of primary vaginal cancer. Radiother Oncol 2005;77:133.
Tjalama WA et al: The role of surgery in invasive squamous carcinoma of the vagina. Gynecol Oncol 2001;81:360.