Health Centers > Heart Diseases Health Center > Heart Attack Overview
Heart Attack Overview
What Is a Heart Attack?
A heart attack happens when the flow of oxygen-rich blood to a section of heart muscle suddenly becomes blocked and the heart can't get oxygen. If blood flow isn't restored quickly, the section of heart muscle begins to die.
What Is a Heart Attack
What is
Other Names
Causes
Risk Factors
Signs and Symptoms
Diagnosis
Treatments
Prevention
Life After
Heart Failure Overview
Heart Attack FAQ
Heart attacks are a leading killer of both men and women in the United States. The good news is that excellent treatments are available for heart attacks. These treatments can save lives and prevent disabilities.
Heart attack treatment works best when it's given right after symptoms occur. If you think you or someone else is having a heart attack (even if you're not fully sure), call9-1-1 right away.
Overview
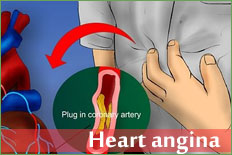
Heart attacks most often occur as a result of coronary heart disease (CHD), also called coronary artery disease. CHD is a condition in which a waxy substance called plaque (plak) builds up inside the coronary arteries. These arteries supply oxygen-rich blood to your heart.
When plaque builds up in the arteries, the condition is called atherosclerosis (ath-er-o-skler-O-sis). The buildup of plaque occurs over many years.
Eventually, an area of plaque can rupture (break open) inside of an artery. This causes a blood clot to form on the plaque's surface. If the clot becomes large enough, it can mostly or completely block blood flow through a coronary artery.
If the blockage isn't treated quickly, the portion of heart muscle fed by the artery begins to die. Healthy heart tissue is replaced with scar tissue. This heart damage may not be obvious, or it may cause severe or long-lasting problems.
A less common cause of heart attack is a severe spasm (tightening) of a coronary artery. The spasm cuts off blood flow through the artery. Spasms can occur in coronary arteries that aren't affected by atherosclerosis.
Heart attacks can be associated with or lead to severe health problems, such as heart failure and life-threatening arrhythmias (ah-RITH-me-ahs).
Heart failure is a condition in which the heart can't pump enough blood to meet the body's needs. Arrhythmias are irregular heartbeats. Ventricular fibrillation is a life-threatening arrhythmia that can cause death if not treated right away.
Other Names
- Coronary thrombosis
- Coronary occlusion
- Acute coronary syndrome
- Myocardial infarction or MI
- Acute myocardial infarction or AMI
Causes
Coronary heart disease is caused by any problem with the coronary arteries that keeps the heart from getting enough oxygen- and nutrient-rich blood. The most common cause by far is atherosclerosis. Lack of sufficient blood is called ischemia, so coronary heart disease is sometimes called ischemic heart disease.
The cause of coronary heart disease is related to multiple risk factors. The following are the most common:
- Heredity: Coronary heart disease runs in the family.
- High cholesterol: Levels of cholesterol in the blood are above healthy levels. This usually involves high levels of low-density lipoprotein (LDL), the bad cholesterol, and low levels of high-density lipoprotein (HDL), the good cholesterol.
- Tobacco abuse: This includes not only smoking any form of tobacco (cigarettes, cigars, pipes), but also chewing tobacco.
- Obesity
- High blood pressure (hypertension)
- Diabetes
- Lack of regular exercise
- High-fat diet
- Emotional stress
- Type A personality (impatient, aggressive, competitive)
Your sex. Overall, more men have heart attacks than women do, and they experience them earlier in life, too. While a woman's risk of dying from heart disease increases after menopause, it's still lower than a man's. Your race. Somewhat related to family history, your race can also predetermine part of your risk of heart disease. African Americans, American Indians, Mexican Americans, and native Hawaiians are more likely to have heart disease than Caucasians, but this is partly due to other risk factors that these populations tend to experience, such as diabetes and high blood pressure.
Your body type. Whether or not you become overweight or obese is mostly within your control, but you cannot control your weight distribution, which refers to where your body stores fat. For years, experts warned that people who tend to carry excess weight in their belly area (known as "apple" shapes) are at a greater risk of several health problems, including heart disease, while "pear" shaped bodies that store more fat in the lower body don't have the same risk. However, one 2010 study published in The Lancet dispelled that idea, saying that being overweight (regardless of where your body stores the fat) is a heart disease risk factor. Your genetics determine your body type; if you are apple-shaped now, you will always be apple-shaped, even if you lose weight. Still, maintaining a healthy body weight - which would decrease your waist circumference - is a controllable risk factor (more on that below) that can reduce your heart disease risk.
Your drinking habits. Drinking too much - and possibly too little - seems to increase one's risk of heart disease. People who drink moderately (defined as an average of one drink day for women and two drinks daily for men) have a lower risk of heart disease than nondrinkers. However, the AHA does not recommend that teetotalers start drinking (or that drinkers increase the amount they drink) in order to achieve these purported benefits. Drinking too much has far more risks than not drinking. Too much alcohol can raise blood pressure and triglycerides, as well as contribute to obesity, irregular heartbeat, cardiomyopathy, alcoholism, heart failure, cancer, stroke and other diseases. To protect your heart, cut back on drinking; if you don't drink often - or at all - don't start.
Diagnosis
It is important that you call 911 if you find yourself (or someone that you are with) experiencing symptoms or the warning signs of a heart attack. The longer treatment is delayed, the more likely it is that irreversible damage will occur to your heart muscle. At the hospital, the doctor will ask you questions and perform tests to determine whether or not the symptoms you are feeling are truly being caused by a heart attack. The doctor will ask questions about your medical history and risk factors for heart disease such as whether you smoke, your family history, and cholesterol history. One or more of the following tests to determine whether or not you have actually had a heart attack, may be performed:
ECG. An ECG (also referred to as an EKG or electrocardiogram) measures the electrical activity of the heart. Changes in the heart's activity levels can signal a heart attack. The EKG also monitors your heart rate for dysrhythmias (irregular heart rates) that can occur during a heart attack. Dysrhythmias may result in the inability of the heart to pump enough blood throughout your body.
Blood Tests. Heart muscle cells contain unique enzymes that help them to function. When heart muscle cells are lysed (broken) during a heart attack, the contents of the cells, including these enzymes, get spilled into the bloodstream. Doctors can measure the levels of these heart muscle enzymes in your blood to determine if you have had a heart attack.
Echocardiography(ECHO). Echocardiography is an ultrasound of the heart. An ECHO is particularly useful at identifying which heart structures have been damaged during a heart attack and the amount of function lost (i.e. how well is the heart able to pump blood after a heart attack).
Stress Test: If your doctor is uncertain whether your chest pain is caused by your heart, he or she may perform a stress test. There are several types of stress tests, but their purpose is similar: to observe your heart (through EKG, ECHO, or nuclear imaging techniques) while it is under stress (i.e., during exercise or after taking medication that causes your heart to work harder). During a stress test the doctor is looking for changes that show your heart is not getting enough blood flow to some of its muscles.
Prevention
While people cannot control their family history and genetics, they can minimize risk factors for heart disease by:
- quitting smoking;
- controlling high blood pressure, cholesterol, diabetes;
- exercise regularly, and
- take a baby aspirin a day.
These are all lifelong challenges to prevent heart disease, stroke, and peripheral vascular disease.
Even with the best of preventive care, heart attacks happen. Develop an emergency plan so that if chest pain occurs make certain you, your family, and friends know how to activate the Emergency Medical Services in your area or call 911.
Lowering your risk factors for coronary heart disease (CHD) can help you prevent a heart attack.
Even if you already have CHD, you can still take steps to lower your risk for a heart attack. These steps involve following a heart healthy lifestyle and getting ongoing care.
Heart Healthy Lifestyle
Following a healthy diet is an important part of a heart healthy lifestyle. A healthy diet includes a variety of fruits, vegetables, and whole grains. It also includes lean meats, poultry, fish, beans, and fat-free or low-fat milk or milk products. A healthy diet is low in saturated fat, trans fat, cholesterol, sodium (salt), and added sugars.
If you're overweight or obese, work with your doctor to create a reasonable weight-loss plan that involves diet and physical activity. Controlling your weight helps you control risk factors for CHD and heart attack.
Be as physically active as you can. Physical activity can improve your fitness level and your health. Talk with your doctor about what types of activity are safe for you.
If you smoke, quit. Smoking can raise your risk of CHD and heart attack. Talk with your doctor about programs and products that can help you quit. Also, try to avoid secondhand smoke. For more information about quitting smoking, go to the Health Topics Smoking and Your Heart article.
Heart Failure Overview
The term "Heart Failure" is used to describe a condition where someone's heart is unable to pump enough blood to support all of his or her body's organs, muscles and other tissues. The heart continues to work during heart failure, but not efficiently enough to adequately support the body's needs. Over 5 million people in the United States have heart failure. It is a major cause of hospitalization for people older than 65 years.
Heart failure can affect one or both sides of the heart. Recall that the heart is divided into four chambers, with each side of the heart containing an atrium and a ventricle. Blood collects in the atria, and is then pumped out by the ventricles. Ventricles can become defective in two different ways; they can either lose their ability to contract, or lose their ability to relax. When the ventricle loses its ability to contract it can no longer generate enough force to push the blood through the body effectively. When the ventricle loses its ability to relax, it can not open enough to fill completely, and the volume of blood available for pumping is drastically reduced. Either condition results in a decreasing rate of blood flow throughout the body's circulatory system which often leads to fluids backing up in various tissues (e.g, "edema").
Causes of Heart Failure
A variety of factors influence whether someone will develop heart failure. Some individuals who develop heart failure may have simply been born with a structural defect in a portion of their heart. Others develop the disease as a result of medical conditions (such as diabetes or high blood pressure) that have not been controlled. The major causes of heart failure include:
- Coronary Artery Disease (atherosclerosis): This disease is caused by fatty plaque buildups that disrupt blood flow in the coronary arteries that supply blood to the heart itself. When the blood flow becomes blocked a heart attack occurs.
- Diabetes: Diabetes is a condition that occurs when your body cannot control your blood sugar levels and maintain them at a normal level. High blood sugar levels can cause damage to many organs such as the heart and kidneys. Individuals with diabetes are more likely to develop heart failure, and this risk is greater if blood sugar levels are not treated and controlled.
- Hypertension (high blood pressure): When pressure in the vessels of the circulatory system increases the heart must work harder to maintain adequate blood flow. Uncontrolled high blood pressure causes the heart muscle to become thicker and stiff, decreasing the heart's ability to relax and adequately collect blood for pumping.
- Heart Valve Dysfunction: When the valves separating the heart's chambers cannot open and close properly for any reason it causes the heart to need to pump harder so as to keep up with the body's demand for oxygen. The elevated strain this process places on the heart can lead to heart failure.
- Cardiomyopathy: Damage and weakening of the heart muscle can lead to reduced efficiency and heart failure. Cardiomyopathy has many causes including viral infections, alcoholism, autoimmune diseases (e.g., rheumatoid arthritis, lupus), high blood pressure, and heart attacks.
- Heart birth defects: Congenital (i.e., something that someone is born with) abnormalities in heart structures such as faulty valves or a deformity in the heart muscle can create heart failure.
- Lung Disease: When the lungs are damaged and they do not provide adequate oxygen for exhausted blood to pick up, the heart pumps faster so as to compensate, placing strain on the heart which can lead to heart failure.
- Thyroid disease: Thyroid hormone regulates the body's metabolic rate (the rate at which your body burns calories for energy). As thyroid hormone levels increase, a person's metabolic rate also increases. People with hyperthyroidism (too much thyroid hormone) have an increased metabolism, which will necessitate the heart pumping faster to supply enough oxygen to the body. Both too much and too little thyroid medicine can result in heart failure that usually is reversible with treatment.
Arrhythmia (dysrhythmia): Arrhythmia is a condition in which the heart beats irregularly rather than rhythmically. This can mean that it either beats too fast, too slow, at a fluctuating pace, or it may skip regular beats. Arrhythmias interfere with normal blood flow. For example, if the ventricle is beating too quickly it will not have enough time to fill up with blood to pump to the rest of the body.
Signs and Symptoms
Acting fast at the first sign of heart attack symptoms can save your life and limit damage to your heart. Treatment works best when it's given right after symptoms occur.
Many people aren't sure what's wrong when they are having symptoms of a heart attack. Some of the most common warning symptoms of a heart attack for both men and women are:
- Chest pain or discomfort. Most heart attacks involve discomfort in the center or left side of the chest. The discomfort usually lasts more than a few minutes or goes away and comes back. It can feel like pressure, squeezing, fullness, or pain. It also can feel like heartburn or indigestion.
- Upper body discomfort. You may feel pain or discomfort in one or both arms, the back, shoulders, neck, jaw, or upper part of the stomach (above the belly button).
- Shortness of breath. This may be your only symptom, or it may occur before or along with chest pain or discomfort. It can occur when you are resting or doing a little bit of physical activity.
- Fullness, indigestion or choking feeling (may feel like heartburn)
- Sweating, nausea, vomiting or
Other possible symptoms of a heart attack include:
- Breaking out in a cold sweat
- Feeling unusually tired for no reason, sometimes for days (especially if you are a woman)
- Nausea (feeling sick to the stomach) and vomiting
- Light-headedness or sudden dizziness
- Any sudden, new symptom or a change in the pattern of symptoms you already have (for example, if your symptoms become stronger or last longer than usual)
Not all heart attacks begin with the sudden, crushing chest pain that often is shown on TV or in the movies, or other common symptoms such as chest discomfort. The symptoms of a heart attack can vary from person to person. Some people can have few symptoms and are surprised to learn they've had a heart attack. If you've already had a heart attack, your symptoms may not be the same for another one.
Quick Action Can Save Your Life: Call 9-1-1
If you think you or someone else may be having heart attack symptoms or a heart attack, don't ignore it or feel embarrassed to call for help. Call 9-1-1 for emergency medical care. Acting fast can save your life.
Do not drive to the hospital or let someone else drive you. Call an ambulance so that medical personnel can begin life-saving treatment on the way to the emergency room. Take a nitroglycerin pill if your doctor has prescribed this type of treatment.
Outlook
Each year, close to 1 million people in the United States have heart attacks, and many of them die. CHD, which often results in heart attacks, is the leading killer of both men and women in the United States.
Many more people could survive or recover better from heart attacks if they got help faster. Of the people who die from heart attacks, about half die within an hour of the first symptoms and before they reach the hospital.
Bibliography
American Heart Association website. Available at: http://www.americanheart.org . Accessed August 14, 2008.
National Heart, Lung, and Blood Institute website. Available at: http://www.nhlbi.nih.gov/ .
Mayo Clinic website. Available at: http://www.mayoclinic.com/health/heart-attack-symptoms/HB00054 . Accessed January 23, 2007.
Huffington Post. "Is the Apple or Pear-Shaped Body Type More Dangerous?," accessed March 2011. www.huffingtonpost.com.
National Heart, Lung and Blood Institute. "Coronary Heart Disease Risk Factors," accessed March 2011. www.nhlbi.nih.gov.
WebMD. "Risk Factors for Heart Disease," accessed March 2011. www.webmd.com.