Viral Infections and breast cancer
Human papillomavirus (HPV) infection, herpes simplex, and herpes zoster (“shingles”) are occasionally found in breast cancer patients.
HPV Infection
HPV infection can cause condylomata of the external genitals and perianal region.
Condylomata acuminata of the vulva, vagina, and perianal area are usually associated with forms of HPV that have low oncogenic potential.
In the case of such lesions, specific HPV typing is not usually performed.
A simple biopsy of one of the lesions will confirm the diagnosis of condylomata and differentiate the lesions from vulval or vaginal in situ or invasive carcinoma. Biopsy is necessary because early invasive squamous carcinoma of the vulva sometimes appears similar to a condyloma.
Condylomata acuminata can be treated in a variety of ways, including simple excision, cryotherapy, laser ablation, and use of topical preparations. Recently, 5% imiquimod in a cream base has been used. The cream is applied three times weekly before bedtime and is washed off the next day with mild soap and water.
The surrounding normal skin should be protected by applying petroleum-based jelly and covering with cotton gauze when imiquimod cream is applied because imiquimod can be very irritating. Imiquimod cream can be used for up to 16 weeks. Another topical treatment, podophyllotoxin 5% solution or gel, is applied to condylomata in cycles consisting of twice-daily treatment for 3 days followed by 4 days of no therapy. Up to four cycles of treatment may be given. Lesions larger than 2-3 cm are best treated by cryotherapy, electrocautery, or laser surgery. Recurrences are common with all treatments and usually occur within 3 months.
 Table 15-2. Diagnosis and Treatment of Nontrichomonal Purulent Vaginal Discharge
Table 15-2. Diagnosis and Treatment of Nontrichomonal Purulent Vaginal Discharge
As previously stated, the subtypes of HPV that cause condylomata do not usually lead to malignancy. However, other HPV subtypes, known as “high risk” or oncogenic types, may be associated with or may predispose to cervical, vaginal, or vulval neoplasias. Screening for the oncogenic types of HPV is now available and is performed routinely on Pap test specimens that show atypical squamous cells of undetermined significance. There is presently no effective treatment that will eliminate HPV, and HPV typing does not preclude the need for cytology screening on an annual basis or more frequently if indicated by an atypical Pap test result. The Food and Drug Administration has approved a vaccine that targets HPV types 6, 11, 16, and 18. HPV types 6 and 11 cause 90% of genital warts, and HPV types 16 and 18 cause 70% of cervical cancers. The vaccine is approved for women ages 9-26 years.
Herpes Simplex
Herpes simplex is a highly contagious, recurrent, incurable sexually transmitted disease; 75% of sex partners of infected individuals will be affected.
The incubation period ranges from 3 to 7 days.
Herpes simplex typically presents as multiple small vesicles on an erythematous base; the appearance of these vesicles is followed by the appearance of one or more painful, shallow ulcers. These ulcers can occur on any part of the vulva and can be extremely painful when they occur on the labia minora or close to the urethra. Symptoms, including the vesicular phase, may persist for 10-14 days. Patients often report a prior history of herpetic lesions that began as a vesicular rash. Herpetic lesions may also be associated with tender inguinal lymphadenopathy. Viral cultures can be done to confirm the diagnosis, but it takes 2-4 days to get the results, and it is usually not practical to delay treatment until the results are received. Several therapies are available that may alleviate the pain and accelerate healing of the ulcers (Table 15-3).
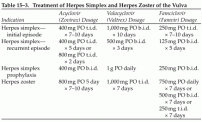 Table 15-3. Treatment of Herpes Simplex and Herpes Zoster of the Vulva
Table 15-3. Treatment of Herpes Simplex and Herpes Zoster of the Vulva
Topical treatment with solutions that contain aluminum acetate and acetic acid is soothing. Daily suppressive therapy in patients who have more than six recurrences per year decreases the frequency of outbreaks by approximately 75%. Patients are infectious while lesions or prodromal symptoms (burning, tingling, pruritis) are present, but importantly, asymptomatic viral shedding frequently occurs.
Herpes Zoster
Herpes zoster of the vulva is exceedingly rare. The presentation and management of herpes zoster of the vulva are the same as the presentation and management of herpes zoster at other sites. Patients with herpes zoster who are receiving chemotherapy, particularly high-dose chemotherapy, should be treated with the same antiviral agents that are used to treat herpes simplex. In severely immunocompromised patients and those with disseminated herpes zoster, intravenous treatment may be required. Such patients should also usually receive antiviral agents as prophylaxis during and immediately after the administration of high-dose chemotherapy.
Elizabeth R. Keeler, Pedro T. Ramirez, and Ralph S. Freedman
Committee on Gynecological Practice, the American College of Obstetricians and Gynecologists. Obstet Gynecol 2007