Axillary Surgery
Axillary dissection (AD) has been part of breast cancer surgery from the time of Halsted. The status of the axillary nodes remains the most powerful prognostic indicator in the treatment of invasive breast cancer. Debate exists concerning the therapeutic value of AD; however, intuitively, removing lymph nodes containing metastatic breast cancer should have a small but identifiable survival benefit.
Historically, this was the rationale for the inclusion of a full axillary dissection in the radical mastectomy. Adair reviewed 1,458 patients who had had radical mastectomy as sole treatment in the 1940s and showed that there were many women among them whose breast cancer had included ymph node involvement who were long-term survivors (all levels of lymph node involvement were represented among them). Presumably, removing the disease was curative in these patients.
The NSABP-B04 trial challenged the rationale for axillary dissection. It compared radical mastectomy, total mastectomy with radiation therapy to the axilla and total mastectomy alone, with subsequent axillary dissection for isolated axillary recurrence. There was no statistically significant survival difference between the three arms of the study. This has been interpreted as showing that axillary dissection does not confer a survival benefit.
Many clinicians, however, are uncomfortable with this interpretation. Close examination of the NSABP-04 study shows that it was not powerful enough to detect a 5-10% difference between the treatment arms; furthermore, surgeons were allowed to remove nodes in the total-mastectomy arm, greatly confounding trial results. It is worth noting that even the NSABP continued to mandate a full axillary dissection in all subsequent trials involving invasive breast cancer.
Recently, an important analysis of a large number of patients from the National Cancer Registry showed a clear survival benefit in women in whom axillary nodes were removed compared with those in whom nodes were not removed. Other studies have found a survival advantage for axillary dissection over both axillary sampling (removal of a small number of nodes) and observation. Currently, the issue remains unresolved.
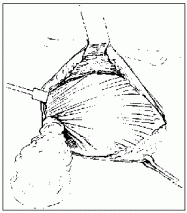
The breast is removed along with the pectoralis fascia in a superomedial to inferolateral direction. Axillary dissection is not necessary for pure DCIS. With invasive carcinoma, if the patient is clinically node positive, axillary dissection is the most effective method of gaining local control and offers the best chance of cure. It also provides staging and prognostic information. In clinically node-negative disease, the main objectives of dissection are to obtain information used to guide the selection of adjuvant therapy and to gain prognostic information.
About one-third of clinically nonsuspicious axillae will contain lymph node metastases, and in these patients, the dissection provides local control and, possibly, a survival benefit.
Nodal status remains the most significant prognostic factor in breast cancer, and the incidence of nodal metastases is closely related to the size of the tumor. As greater numbers of small breast cancers are being diagnosed, the wisdom of routine axillary dissection has been called into question. There has been considerable debate over the true incidence of axillary nodal disease in invasive breast cancer less than 5 mm in size (T1a lesions).
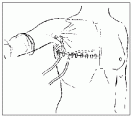
The wound is closed over a suction drain (illustration shows a second drain in the axilla) using a subcuticular suture and steri-strips. One study found an incidence of nodal metastases in these patients of 3%, and consequently, some have advocated omission of axillary surgery in these patients. A large series from Memorial Sloan-Kettering Cancer Center found that the incidence of nodal metastases in T1a tumors was 10% and 15% in T1b tumors, with no subgroup having an insignificant incidence. Other series have also found an incidence of about 10%.
The problem with axillary dissection is that the incidence of morbidity is high. This is discussed in detail later in this chapter. Sentinel node mapping has been developed and introduced in response to the problem of the “unnecessary” morbidity of a negative lymph node dissection.
In the absence of sentinel node biopsy, it is reasonable to tailor the extent of axillary dissection to the individual situation, such as in the case of an elderly woman with a small ER-positive tumor. In the case of a T1 or T2 tumor with clinically negative nodes, a level 1 and 2 dissection should be performed. The incidence of level 3 nodal involvement in this case is low. In cases involving gross disease within the axilla, a full, three-level dissection should be performed.
Patrick I. Borgen and Bruce Mann
Breast conservation therapy for invasive carcinoma of the breast. Current Problems in Surgery 1995; 33:189-256.
References
- Veronesi U, Saccozzi R, Del Vecchio M et al. Comparing radical mastectomy with quadrantectomy, axillary dissection, and radiation therapy in patients with small cancers of the breast. N Engl J Med 1981; 305:6-11.
This is the landmark report of the first randomized prospective trial of breast-conservation therapy. - Fisher B, Bauer M, Margolese R et al. Five-year results of a randomized clinical trial comparing total mastectomy and segmental mastectomy with or without radiation in the treatment of breast cancer. N Engl J Med 1985; 312:665-73.
This is the first report of the major North American trial of breast-conservation therapy from the NSABP. - Borgen PI, Heerdt AS, Moore MP et al. Breast conservation therapy for invasive carcinoma of the breast. Current Problems in Surgery 1995; 33:189-256.
This is a review of all aspects of breast-conservation therapy. - Fisher B, Costantino J, Redmond C et al. Lumpectomy compared with lumpectomy and radiation therapy for the treatment of intraductal breast cancer. N Engl J Med 1993: 1581-6.
This is the major trial of conservative therapy for DCIS - Adair F, Berg J, Joubert L et al. Long-term follow-up of breast cancer: the 30-year report. Cancer 1974; 33:1145-50.
This is an older report from the days before adjuvant therapy that demonstrates the effectiveness of surgery in node-positive disease. - Fisher B, Redmond C, Fisher E et al. Ten year result of a randomized clinical trial comparing radical mastectomy and total mastectomy with of without irradiation. N Engl J Med 1985; 312:674-81.
This is a very influential trial that showed that less-extensive surgery had similar results to radical mastectomy. - Warmuth MA, Bowen G, Prosnitz LR et al. Complications of axillary lymph node dissection for carcinoma of the breast: a report based on a patient survey. Cancer 1998; 83:1362-8.
This report gives a good idea of the range of complications after axillary dissection.