The Mammogram Report: The Breast Imaging Reporting and Data System (BI-RADS™) Lexicon
Calcifications
The BI-RADS™ lexicon describes calcification morphology (shape) and distribution. Calcification morphology is divided into three groups: typically benign, intermediate level of concern and higher probability of malignancy.
Typically benign morphologies include skin (lucent centered), vascular (parallel tracks), coarse or “popcorn-like” (fibroadenomas), large rod-like (secretory disease), round (often in acini of lobules; when under 0.5 mm, called “punctate”), lucent-centered, eggshell or rim (fat necrosis), milk of calcium (within tiny cysts), suture (may have knots) or dystrophic (after trauma or irradiation). A morphology that is of an intermediate level of concern is amorphous/indistinct (round or “flake shaped,” small or hazy in appearance). Morphologies that have a higher probability of malignancy are pleomorphic or heterogeneous (granular) calcifications (often varying in size and shape, usually less than 0.5 mm in diameter) and fine/linear or fine/linear/branching (casting) calcifications (appear linear but discontinuous, suggests irregular filling of a duct lumen by breast cancer).
Calcification distribution can be described as grouped or clustered (multiple calcifications in less than 2 cc of tissue), linear (arrayed in a line that may have branch points), segmental (suggests deposits in a duct and its branches, raises possibility of multifocal breast cancer in a lobe or segment of the breast), regional (scattered in a large volume of tissue but not necessarily conforming to a duct distribution) or diffuse/scattered (random in arrangement). The term “multiple” is used to indicate more than one group of calcifications similar in morphology and distribution.
The frequency of carcinoma as a function of calcification morphology of lesions that had surgical and distribution in a study by Liberman et al biopsy is shown in Table 6.2.
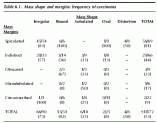
Table 6.1. Mass shape and margins: frequency of carcinoma
The highest frequency of carcinoma was observed in calcifications that had linear morphology or segmental or linear distribution.
Associated Findings
The mammogram report should describe associated findings, including skin or nipple retraction, skin or trabecular thickening, skin lesions, axillary adenopathy and the presence of architectural distortion.
Lesion Location
Lesion location should be indicated by the breast (left, right or both), depth (anterior, middle, or posterior one-third of the breast) and location in relation to the nipple (as if you are using a clock face, facing the patient with 12:00 up, 6:00 down, 3:00 to the patient’s left, and 9:00 to the patient’s right: thus, 9:00 is lateral in the right breast and medial in the left breast).
Assessment Categories
Every report should include an overall summary impression and give one of the BI-RADS™ assessment categories as listed in Table 6.3.
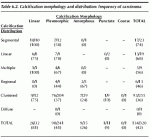
Table 6.2. Calcification morphology and distribution: frequency of carcinoma
In general, additional imaging evaluation is suggested for BI-RADS™ Category 0 lesions. Routine screening mammography is appropriate for BI-RADS™ Category 1 (normal mammogram) or 2 (benign finding). For BI-RADS™ Category 3 (probably benign) lesions, the recommendation is 6 month follow-up of the ipsilateral breast, followed by bilateral mammograms at 1 year, 2 years, and 3 years following the initial screening study. Biopsy is suggested for lesions classified as BI-RADS™ Category 4 (suspicious abnormality) and 5 (highly suggestive of malignancy).