Technique of Axillary Dissection
The arm is draped free and rests on an arm board for most of the procedure.
During dissection of the apex of the axilla, the arm can be flexed and abducted to relax the pectoralis major muscle and allow better access. Care is taken to avoid stretching the brachial plexus.
For axillary dissection as an independent procedure, the incision is planned to maximize exposure while allowing for an excellent cosmetic result. A transverse or somewhat u-shaped incision extending from the lateral margin of the pectoralis major to the anterior border of the latissimus dorsi meets these requirements (Fig. 7.9). It is important to avoid a radial incision extending from the breast to the axilla.
While this does provide excellent exposure, scar shortening produces significant distortion, especially after breast irradiation.
During modified radical mastectomy, axillary exposure is excellent after removal of the breast.
Skin flaps are elevated at the level of the axillary fascia. There are no lymph nodes superficial to this; therefore, it is unnecessary to excise the subcutaneous fat. The superior flap is elevated to the level of the transverse skin crease. A medial flap is elevated to expose the lateral margin of the pectoralis major. A lateral flap is raised to expose the anterior border of the latissimus dorsi. The extent of the inferior flap is arbitrary, as there are no bony or muscular landmarks. It is usually extended to about the fifth or sixth intercostal space (Fig. 7.9).
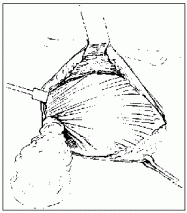 Fig. 7.7. The breast is removed along with the pectoralis fascia in a superomedial to inferolateral direction. The lateral edge of the pectoralis major is exposed. The clavipectoral fascia is then excised along the lateral margin of the pectoralis minor, from the vicinity of the axillary vein to the costal origin of the pectoralis minor. In the upper part, a neurovascular bundle containing the medial pectoral nerve and branches of the thoracoacromial vessels is found, and the nerve is preserved if possible.
Fig. 7.7. The breast is removed along with the pectoralis fascia in a superomedial to inferolateral direction. The lateral edge of the pectoralis major is exposed. The clavipectoral fascia is then excised along the lateral margin of the pectoralis minor, from the vicinity of the axillary vein to the costal origin of the pectoralis minor. In the upper part, a neurovascular bundle containing the medial pectoral nerve and branches of the thoracoacromial vessels is found, and the nerve is preserved if possible.
The incision is carried laterally, in front of the estimated position of the axillary vein (Fig. 7.10). At this time it is important to limit the dissection to the area below the axillary vein. Vigorous traction during dissection can easily lead the surgeon to remove a pad of fat from the front of the vein as well.
Fig. 7.8. The wound is closed over a suction drain (illustration shows a second drain in the axilla) using a subcuticular suture and steri-strips. 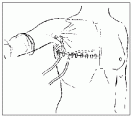 For a more extensive nodal clearance, the pectoralis minor muscle can be excised or divided. Unless there is extensive nodal disease, it is not usually necessary to do this. Retraction of both pectoral muscles after flexion and abduction of the arm usually allows adequate access to the apex of the axilla.
For a more extensive nodal clearance, the pectoralis minor muscle can be excised or divided. Unless there is extensive nodal disease, it is not usually necessary to do this. Retraction of both pectoral muscles after flexion and abduction of the arm usually allows adequate access to the apex of the axilla.
The upper level of dissection is individualized. The axillary lymph nodes are then dissected from the lateral chest wall and from below the axillary vein. Small arteries and tributaries of the vein are ligated. There is usually one large tributary of the axillary vein requiring individual ligation. The second intercostal nerve (the intercostobrachial nerve) traverses the axilla about 2 cm below the axillary vein. It supplies the skin of the axilla and the medial aspect of the upper arm.
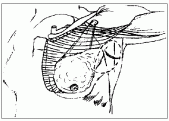 Fig. 7.9. Schematic diagram showing the incision for an axillary dissection and the extent to which flaps are elevated.It is possible to preserve this nerve in most cases, although many surgeons routinely divide it. The long thoracic nerve passes straight down the chest wall in a position about 2 cm posterior to the intercostobrachial nerve. It lifts off the chest wall with the axillary fat and must be deliberately separated from the specimen and placed back on the chest wall (Fig. 7.11). As the dissection of the specimen from the axillary vein progresses, the subscapular vessels appear. The thoracodorsal nerve lies deep and usually medial to these vessels. The nerve and vessels are usually spared, but if there is suspicious nodal disease in the area, they can be sacrificed. Once the long thoracic and thoracodorsal nerves are identified, the tongue of tissue lying between them on the subscapularis muscle is then removed (Fig. 7.12).
Fig. 7.9. Schematic diagram showing the incision for an axillary dissection and the extent to which flaps are elevated.It is possible to preserve this nerve in most cases, although many surgeons routinely divide it. The long thoracic nerve passes straight down the chest wall in a position about 2 cm posterior to the intercostobrachial nerve. It lifts off the chest wall with the axillary fat and must be deliberately separated from the specimen and placed back on the chest wall (Fig. 7.11). As the dissection of the specimen from the axillary vein progresses, the subscapular vessels appear. The thoracodorsal nerve lies deep and usually medial to these vessels. The nerve and vessels are usually spared, but if there is suspicious nodal disease in the area, they can be sacrificed. Once the long thoracic and thoracodorsal nerves are identified, the tongue of tissue lying between them on the subscapularis muscle is then removed (Fig. 7.12).
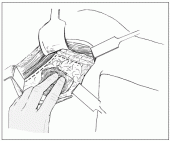 Fig. 7.10. Incision of the clavipectoral fascia along the lateral edge of the pectoralis minor and below the axillary vein. The position of the vein is outlined.
Fig. 7.10. Incision of the clavipectoral fascia along the lateral edge of the pectoralis minor and below the axillary vein. The position of the vein is outlined.
The thoracodorsal nerve is finally dissected free from the specimen. This requires ligation of a few small vessels.
The specimen is marked to identify the apical nodes. Hemostasis is secured, a suction drain is placed, and the wound closed with an absorbable subcuticular suture. Postoperatively, the drain should remain in place until the daily drainage is less than 30 cc.
Patrick I. Borgen and Bruce Mann
Breast conservation therapy for invasive carcinoma of the breast. Current Problems in Surgery 1995; 33:189-256.
Fig. 7.2. The skin and subcutaneous tissue is incised down to the vicinity of the mass.
Fig. 7.3. The mass is grasped with a clamp and excised using sharp dissection.
Fig. 7.4. The wound is closed with a subcuticular suture and steri-strips. The cavity is not closed.
Fig. 7.5. Skin flaps are marked to include the biopsy site. Enough skin is removed to result in a flat scar.
Fig. 7.6. Skin flaps are developed with upward traction on the skin, and countertraction on the breast. The breast is removed with its fascial envelope.
Fig. 7.7. The breast is removed along with the pectoralis fascia in a superomedial to inferolateral direction.
Fig. 7.8. The wound is closed over a suction drain (illustration shows a second drain in the axilla) using a subcuticular suture and steri-strips.
Fig. 7.9. Schematic diagram showing the incision for an axillary dissection and the extent to which flaps are elevated.
Fig. 7.10. Incision of the clavipectoral fascia along the lateral edge of the pectoralis minor and below the axillary vein. The position of the vein is outlined.
Fig. 7.11. Axillary dissection in progress. The anterior tributary of the axillary vein has been divided, the intercostobrachial nerve has been preserved and the long thoracic nerve identified.
Fig. 7.12. Advanced stage of axillary dissection. The thoracodorsal nerve has been preserved, and the tissue between the long thoracic and thoracodorsal nerves has been removed.
References
- Veronesi U, Saccozzi R, Del Vecchio M et al. Comparing radical mastectomy with quadrantectomy, axillary dissection, and radiation therapy in patients with small cancers of the breast. N Engl J Med 1981; 305:6-11.
This is the landmark report of the first randomized prospective trial of breast-conservation therapy. - Fisher B, Bauer M, Margolese R et al. Five-year results of a randomized clinical trial comparing total mastectomy and segmental mastectomy with or without radiation in the treatment of breast cancer. N Engl J Med 1985; 312:665-73.
This is the first report of the major North American trial of breast-conservation therapy from the NSABP. - Borgen PI, Heerdt AS, Moore MP et al. Breast conservation therapy for invasive carcinoma of the breast. Current Problems in Surgery 1995; 33:189-256.
This is a review of all aspects of breast-conservation therapy. - Fisher B, Costantino J, Redmond C et al. Lumpectomy compared with lumpectomy and radiation therapy for the treatment of intraductal breast cancer. N Engl J Med 1993: 1581-6.
This is the major trial of conservative therapy for DCIS - Adair F, Berg J, Joubert L et al. Long-term follow-up of breast cancer: the 30-year report. Cancer 1974; 33:1145-50.
This is an older report from the days before adjuvant therapy that demonstrates the effectiveness of surgery in node-positive disease. - Fisher B, Redmond C, Fisher E et al. Ten year result of a randomized clinical trial comparing radical mastectomy and total mastectomy with of without irradiation. N Engl J Med 1985; 312:674-81.
This is a very influential trial that showed that less-extensive surgery had similar results to radical mastectomy. - Warmuth MA, Bowen G, Prosnitz LR et al. Complications of axillary lymph node dissection for carcinoma of the breast: a report based on a patient survey. Cancer 1998; 83:1362-8.
This report gives a good idea of the range of complications after axillary dissection.