More evidence not all prostate cancers need treatment
In a study of older men who had died from causes other than prostate cancer, almost half were found to have prostate tumors.
And up to half of those tumors detected on autopsy would have qualified for treatment had doctors known about them while the men lived, though none had been the cause of death.
That suggests the criteria for treatment “might be worth reexamining,” according to the study authors, and adds to a growing body of evidence that a wait-and-see approach might be better than treatment for many prostate cancers.
“The study suggests that the progression of early prostate cancer, including some more aggressive forms of the disease, is far from inevitable within a man’s lifetime as many such tumors are found in men who died from other causes when their prostate is analyzed on autopsy,” said lead author Dr. Alexandre Zlotta, director of Uro-oncology at Mount Sinai Hospital in New York.
“The study concludes that it is probably worth re-examining our current definitions of clinically unimportant and clinically significant prostate cancer,” Zlotta told Reuters Health by email.
He and his colleagues examined the prostate glands of more than 300 men over 60 who had died from a variety of causes, but not prostate cancer. They autopsied 220 men in Russia and 100 in Japan, both countries where the prostate-specific antigen (PSA) screening test is not as commonly used as in the United States.
 Medicare currently covers a yearly PSA test for men over 50 who qualify.
Medicare currently covers a yearly PSA test for men over 50 who qualify.
Zlotta and his colleagues selected a Caucasian population of Russian men similar in lifestyle and risk factors for prostate cancer to U.S. men in order to look at how common the cancer is in older men who have not been routinely screened.
In the U.S., the number of tumors they found would have been much lower because many would have been identified by screening and treated or removed before death, Zlotta pointed out.
Death Rates by Race/Ethnicity
From 1999–2009, the rate of men dying from prostate cancer has varied, depending on their race and ethnicity. The graph below shows that in 2009, black men were more likely to die of prostate cancer than any other group, followed by white, Hispanic, American Indian/Alaska Native, and Asian/Pacific Islander men.
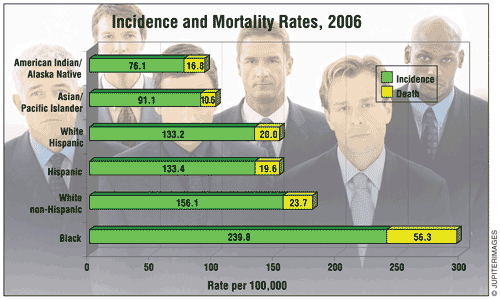
Incidence Rates by Race/Ethnicity
“Incidence rate” means how many men out of a given number get the disease each year. The graph below shows how many men out of 100,000 got prostate cancer each year during the years 1999–2009. The year 2009 is the most recent year for which numbers have been reported. The prostate cancer incidence rate is grouped by race and ethnicity.
The graph below shows that in 2009, black men had the highest rate of getting prostate cancer, followed by white, Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native men.

###
Mortality source: U.S. Mortality Files, National Center for Health Statistics, CDC.
For comparison, he said, “we chose an Asian population in Japan because clinically detected prostate cancer and mortality are much lower among Asian men compared with Caucasian men and their lifestyles/diet are dramatically different.”
Though many fewer Japanese men are diagnosed with or die from prostate cancer than men in the U.S., the new study found that the disease is present in the same proportion of men, and serious tumors are even more common in Japan, based on posthumous prostate examinations.
 Almost 40 percent of the Russian men, had tumors of the prostate, compared to 35 percent of the Japanese men, according to the results published in the Journal of the National Cancer Institute.
Almost 40 percent of the Russian men, had tumors of the prostate, compared to 35 percent of the Japanese men, according to the results published in the Journal of the National Cancer Institute.
One in four tumors in the Russian men were deemed serious and would likely have been treated with surgery or radiation in the U.S., compared to one in two tumors in the Japanese men.
But there are still many differences between Russian and American men, so it is difficult to generalize the results, according to Dr. Stacy Loeb, a urologist at NYU Langone Medical Center in New York.
Prevalence of prostate cancer in the U.S.A.
A report from the Centers for Disease Control, issued last week, suggests that as of January 1, 2007 there were nearly 2.3 million men living in the U.S. after a diagnosis of prostate cancer. The total number of people living with a specific disorder in a defined area at a point in time is known as the “prevalence” of that disorder (as compared to the “incidence,” which is the number of new cases of that disorder each year).
The relatively brief article in the March 11 issue of MMWR (the Morbidity and Mortality Weekly Report) addressed the continuing increase in the number of Americans who are living - and often for a very long time - after an initial diagnosis of cancer: 11.7 million in January 2007 as compared to 3.0 million in 1971 and 9.8 million in 2001.
Estimated data about prostate cancer that appear in the report include the following:
Total prevalence: 2.276 million
Prevalence among men > 85 years of age: 0.262 million
Prevalence among men of 65 to 84 years of age: 1.550 million
Prevalence among men of 40 to 64 years of age: 0.463 million
Prevalence among men of 20 to 39 years of age: less than 500
These data are, of course, only estimates based on information from nine of the Surveillance, Epidemiology, and End Results (SEER) program centers around the country, so they should be interpreted with a degree of caution, but they do continue to confirm what one might reasonably expect to see:
The vast majority of men living with prostate cancer (79.6 percent) are more than 65 years of age.
Prostate cancer occurs, but is extremely rare, in men of less than 40 years of age (0.2 percent).
“We should be cautious about trying to apply the results to Americans where we have a very heterogeneous population including very high risk groups such as African Americans,” Loeb told Reuters Health.
 In the United States, about 239,000 men are expected to be diagnosed with prostate cancer in 2013, but far fewer - less than 30,000 - will die of it, according to the American Cancer Society.
In the United States, about 239,000 men are expected to be diagnosed with prostate cancer in 2013, but far fewer - less than 30,000 - will die of it, according to the American Cancer Society.
That’s still more than will die of the disease in Japan, despite the American men getting more screenings and treatments - a curious inconsistency researchers do not understand and Zlotta called the “million dollar question.”
Prostate cancer screening does ultimately reduce the number of painful advanced cancers and deaths from the disease, but it also picks up smaller cancers, and treating those aggressively could lead to unnecessary side effects, Loeb said.
Prostate removal costs about $13,000, and may lead to impotence or incontinence.
The study authors note that the lifetime risk of a man in the U.S. being diagnosed with prostate cancer is 17 percent, but his risk of dying from prostate cancer is 3.4 percent.
That suggests many of those cancers would not advance quickly or at all, and something else would kill the man long before the prostate tumor. The problem is how to know which tumors will be harmless.
Experts said a new screening test may be needed that differentiates between more dangerous cancers and the many tumors that will not eventually kill, thereby avoiding the expense and risks of treatment and removal.
“An example is the Prostate Health Index (phi) which was recently approved by the FDA,” Loeb said. “It is a simple blood test that combines PSA with 2 other tests, and was shown to better predict the risk of aggressive cancer.”
“The holy grail is to find only those prostate cancers which are life threatening,” she said. “The good news is that this is a very active area of research, and the whole process of screening and assessing continues to improve all the time.”
SOURCE: Journal of the National Cancer Institute online July 11, 2013
###
Prevalence of Prostate Cancer on Autopsy: Cross-Sectional Study on Unscreened Caucasian and Asian Men
Three hundred twenty prostates were collected, 220 from CAU men and 100 from ASI mean. The mean age was 62.5 in CAU men and 68.5 years in ASI men (P
< .001). PCa prevalences of 37.3% in CAU men and 35.0% in ASI men were observed (P = .70). Average tumor volume was 0.303cm3. In men aged greater than 60 years, PCa was observed in more than 40% of prostates, reaching nearly 60% in men aged greater than 80 years. GS 7 or greater cancers accounted for 23.1% and 51.4% of all PCa in CAU and ASI men, respectively, (P = .003). When adjusted for age and prostate weight, ASI men still had a greater probability of having GS 7 or greater PCa (P = .03).
Conclusions PCa is found on autopsy in a similar proportion of Russian and Japanese men. More than 50% of cancers in ASI and nearly 25% of cancers in CAU men have a GS of 7 or greater. Our results suggest that the definition of clinically insignificant PCa might be worth re-examining.
Alexandre R. Zlotta,
Shin Egawa,
Dmitry Pushkar,
Alexander Govorov,
Takahiro Kimura,
Masahito Kido,
Hiroyuki Takahashi,
Cynthia Kuk,
Marta Kovylina,
Najla Aldaoud,
Neil Fleshner,
Antonio Finelli,
Laurence Klotz,
Jenna Sykes,
Gina Lockwood and
Theodorus H. van der Kwast