Observation for prostate cancer questioned in blacks
African American men with very low-risk prostate cancer may not do as well with a wait-and-see treatment approach as white men, suggests a new study.
Researchers found that black men who had their prostates removed soon after being diagnosed with low-risk cancer were more likely to have the severity of their cancer upgraded based on a doctor’s second look, compared to their white counterparts.
“It’s known that outcomes for African Americans with prostate cancer are less good. That’s a known fact,” said Dr. Edward Schaeffer, the study’s senior author from Johns Hopkins Hospital in Baltimore.
“This study’s number one highlight is that because of that observation, we don’t think you should just recommend active surveillance,” he told Reuters Health.
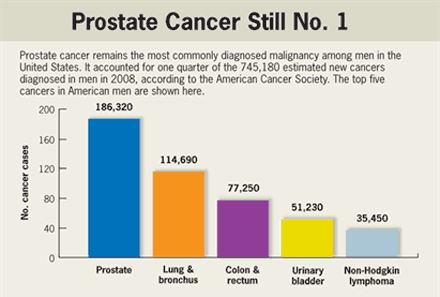
The American Cancer Society estimates about one in six U.S. men will be diagnosed with prostate cancer during his lifetime, and one in 36 will die of the disease.
About 20 percent of cancers are very low-risk and it’s recommended that doctors use “active surveillance” among men who are expected to live for less than 20 years, write Schaeffer and his colleagues in the Journal of Clinical Oncology.
 With active surveillance, the prostate cancer is closely monitored but not treated. That allows men to avoid the potential side effects of radiation and surgery, such as incontinence and impotence. It also gives doctors a chance to intervene if the cancer worsens.
With active surveillance, the prostate cancer is closely monitored but not treated. That allows men to avoid the potential side effects of radiation and surgery, such as incontinence and impotence. It also gives doctors a chance to intervene if the cancer worsens.
But the data used to advise doctors on who the best candidates are for active surveillance are based on studies that included mostly white men. Therefore, the guidelines may not apply to black men, who are known to have worse prostate cancer outcomes, researchers said.
For the new study, Schaeffer and his colleagues analyzed data on 256 black men, 1,473 white men and 72 men of other races who were diagnosed with very low-risk prostate cancer after 1992.
The men all had their prostates surgically removed at Johns Hopkins Hospital soon after they were diagnosed.
The researchers then looked at what doctors actually found when they removed the men’s prostates and whether there were any differences in cancer characteristics between black men and white men.
 Overall, about 27 percent of black men ended up having worse cancers than doctors originally thought, compared to about 14 percent of white men.
Overall, about 27 percent of black men ended up having worse cancers than doctors originally thought, compared to about 14 percent of white men.
Researchers also found more black men had cancers that were likely to return after they were removed.
What’s more, additional research from Schaeffer and his colleagues, published in The Journal of Urology, found that black men tend to have larger tumors located in areas of the prostate that aren’t easily accessible for doctors to biopsy.
“If you have an African American man with very low-risk prostate cancer, our recommendation at this time is that they strongly consider a MRI of their prostate (to look for these tumors),” Schaeffer said.
Theresa W. Gillespie, who was not involved with the new research but has studied prostate cancer in black men, said the new study alone won’t change existing treatment guidelines.
She added, however, that it sheds light on the fact that medical research needs to include more African Americans to get better population-based guidelines.
“We need to have more African Americans involved in research. All of the studies that were cited… the number of African Americans involved in those studies … are very small numbers,” Gillespie, from the Emory University School of Medicine in Atlanta, told Reuters Health.
Schaeffer said the new findings need to be validated in other groups and that his team is currently working on additional research.
SOURCE: Journal of Clinical Oncology, online June 17, 2013 and The Journal of Urology, online June 14, 2013.
###
African American Men With Very Low - Risk Prostate Cancer Exhibit Adverse Oncologic Outcomes After Radical Prostatectomy: Should Active Surveillance Still Be an Option for Them?
Results AA men with very low–risk PCa had more adverse pathologic features at RP and poorer oncologic outcomes. AA men were more likely to experience disease upgrading at prostatectomy (27.3% v 14.4%; P
< .001), positive surgical margins (9.8% v 5.9%; P = .02), and higher Cancer of the Prostate Risk Assessment Post-Surgical scoring system (CAPRA-S) scores. On multivariable analysis, AA race was an independent predictor of adverse pathologic features (odds ratio, [OR], 3.23; P = .03) and pathologic upgrading (OR, 2.26; P = .03).
Conclusion AA men with very low–risk PCa who meet criteria for AS but undergo immediate surgery experience significantly higher rates of upgrading and adverse pathology than do white men and men of other races. AA men with very low–risk PCa should be counseled about increased oncologic risk when deciding among their disease management options.
Debasish Sundi,
Ashley E. Ross,
Elizabeth B. Humphreys,
Misop Han,
Alan W. Partin,
H. Ballentine Carter and
Edward M. Schaeffer