Alternative Interventions for Management of Menopause
Many alternative approaches are available to correct or palliate the sequelae of estrogen deficiency, some of which are listed in Table 18-1.
Cardiovascular Health
That cardiovascular disease constitutes the most serious threat to the health of aging women has been amply emphasized in recent years. Constitutional factors that increase the risk of cardiovascular disease include a family history of CHD at a young age; hypertension; a history of claudication or stroke; diabetes mellitus; and hyperlipidemia. Lifestyle factors such as smoking, obesity, and physical inactivity are also important.
Clearly, smoking cessation, weight regulation, and physical fitness are important goals for preserving cardiovascular health and for maintaining a sensible, healthy lifestyle in general. Meticulous control of hypertension, hyperlipidemia, and diabetes is critically important to avoid vascular complications in all affected patients regardless of their age and gender; the panoply of available medications and therapeutic algorithms are outlined in standard medical textbooks.
Osteoporosis
Progressive bone loss occurs with advancing age, and in women, the rate of bone loss is accelerated after menopause. Nevertheless, clinically significant osteoporosis with disabling vertebral or hip fractures is far from inevitable. While estrogen deficiency remains a very important correlate with osteoporosis, hereditary and racial influences on bone mass are becoming increasingly appreciated. Thin frame, sedentary lifestyle, white race, and smoking are all important risk factors for osteoporosis. Currently, two classes of agents are available for the treatment of osteoporosis: antiresorptive and anabolic agents. Antiresorptive agents include bisphosphonates, calcitonin, and selective estrogen receptor modulators; anabolic agents include teriparatide (recombinant human parathyroid hormone) and strontium ranelate. Vitamin D and calcium supplements are integral components of any approach to fracture prevention in postmenopausal patients.
Bisphosphonates
In recent years, bisphosphonates have emerged as an effective and welltolerated group of compounds that support and even enhance bone mineral density, primarily through the inhibition of osteoclast attachment to the bone matrix. The bisphosphonates are the most widely prescribed antiresorptive agents and should be regarded as first-line agents for the prevention and treatment of osteoporosis. The available data indicate that the benefits of bisphosphonates persist during several years of continuous therapy.
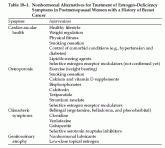 Table 18-1. Nonhormonal Alternatives for Treatment of Estrogen-Deficiency Symptoms in Postmenopausal Women with a History of Breast Cancer
Table 18-1. Nonhormonal Alternatives for Treatment of Estrogen-Deficiency Symptoms in Postmenopausal Women with a History of Breast Cancer
The impact of bisphosphonates on long-term morbidity and mortality from skeletal fractures is still under investigation but appears promising on the basis of results of initial studies spanning several years of continued use (Tonino et al., 2000; Bone et al., 2004). The available bisphosphonates include alendronate and risedronate, both of which have been shown to reduce the incidence of hip, vertebral, and other nonvertebral fractures by nearly 50%. Ibandronate is a newer bisphosphonate, but there is less clinical experience with this drug than with other bisphosphonates.
The most significant side effect of bisphosphonates is esophageal irritation, which can be minimized by taking the drug on an empty stomach in an upright position with at least 6 ounces of water and maintaining the upright position for 30 minutes. For patients unable to tolerate oral administration, intravenous bisphosphonates, such as pamidronate and zoledronate, may be considered. However, the efficacy of the intravenous bisphosphonates in preventing fractures in postmenopausal women has not been established.
Calcitonin
Calcitonin is approved for the treatment of osteoporosis. It prevents bone loss and has important analgesic properties, although there is no good evidence that it reduces the incidence of hip fracture. Calcitonin administered as a daily injection frequently causes nausea and flushing; these side effects can be especially disturbing to women with a history of cancer and prior exposure to chemotherapy. The nasal-spray formulation appears to be tolerated better.
Teriparatide
Teriparatide, a synthetic human parathyroid hormone analogue, has been demonstrated to have anabolic effects on bone and was recently approved for the treatment of osteoporosis. In patients treated with teriparatide, both vertebral and nonvertebral fractures were decreased by more than 50% (Neer et al., 2001). Use of teriparatide is limited to 2 years because of a lack of information regarding safety beyond that duration. Teriparatide is recommended for use in patients with moderate to severe osteoporosis. Paradoxically, concurrent use with bisphosphonates has been shown to dampen the effect of teriparatide on bone formation. Side effects include nausea, dizziness, and leg cramps. Development of osteosarcoma was noted in animal models but has yet to be observed in human subjects. However, given the theoretical risk, patients with or at risk for osteosarcoma should not receive teriparatide.
Breast cancer patients who have received radiation therapy to the chest for their breast cancer have an increased risk of radiation-induced osteosarcoma and, likewise, should not receive teriparatide. Breast cancer patients with established metastatic bone disease should not be treated with teriparatide.
Since the drug is associated with a modest increase in serum calcium levels, it should not be administered to anyone with hypercalcemia.
Strontium Ranelate
Strontium ranelate has recently been the subject of renewed interest because of its anabolic effects on bone. Unlike other available therapies for the prevention and treatment of osteoporosis, strontium ranelate may simultaneously decrease bone resorption and promote bone formation. Recent reports indicate that this drug decreases both vertebral and nonvertebral fractures, but long-term studies of efficacy are lacking. Side effects of strontium ranelate include nausea and diarrhea, which generally abates after 3 months of use.
Prevention of Calcium and Vitamin D Deficiency
Prevention of calcium and vitamin D deficiency is an important measure for the maintenance of skeletal integrity. Calcium supplementation significantly slows bone loss in healthy postmenopausal women and is generally included in regimens designed to prevent or treat osteoporosis. The issue of whether pharmacologic administration of vitamin D can significantly reduce the risk of vertebral or hip fracture remains controversial.
Analysis of data pooled from randomized trials in the Cochrane database indicates that co-administration of 1,000 mg calcium with 700-800 IU vitamin D results in a statistically significant reduction in the incidence of hip fractures and of all nonvertebral fractures in the populations studied (Avenell et al., 2005). Recent data from the WHI trial have raised questions about the benefit of calcium and vitamin D use in reducing the risk of hip fracture. Issues surrounding the doses of calcium and vitamin D in that trial and the design of the trial to achieve suitable power make the data difficult to interpret. It remains our policy to ensure that all women with or at risk for osteoporosis receive adequate daily calcium and vitamin D.
Additional Interventions to Prevent or Treat Osteoporosis
Benefit of exercise in the prevention of osteoporosis is an intuitive concept but has been difficult to document. While immobilization and weightlessness result in significant bone loss, neither endurance nor weight-bearing-exercise programs have been shown to prevent or reverse menopause-induced osteopenia. Perhaps the single most important measure that can reduce the cost and suffering associated with osteoporosis is the prevention of accidental falls, which are the most frequent immediate cause of hip fractures.