Early Detection of Breast Cancer: Summary
X-ray mammography is now the mainstay for the detection, diagnosis, and localization of breast cancers. It is currently the only medical imaging procedure used as a screening tool. Screening mammography has definitively been shown to reduce, but not eliminate mortality from breast cancer when it is performed at regular intervals and followed by appropriate interventions. In randomized clinical trials, screening mammography reduced breast cancer mortality by about 25 to 30 percent among women ages 50 to 70 and by about 18 percent among women between the ages of 40 and 50. Although the incidence of breast cancer increases with age, data on the benefits of screening for older women are lacking because most randomized trials excluded women over age 70.
Recent observational studies suggest that mammography is also beneficial for women over age 70, but further documentation of benefit is important. There is also some indirect evidence that screening mammography has been effective in reducing the number of deaths from breast cancer in the general population. Mortality from breast cancer in the United States, as well as some European countries, has been decreasing in recent years, and some of this reduction is consistent with the effect of screening.
However, there is clearly room for improvement in the screening and diagnosis of breast cancer because of both the technical and the biological limitations of the current methods. Although the clinical practice of mammography is federally regulated for quality assurance (the only clinical procedure regulated in this way), it is still technically difficult to consistently produce mammograms of high quality, and interpretation is subjective and can be variable among radiologists.
Furthermore, mammography does not detect all breast cancers, including some that are palpable, and as many as three-quarters of all breast lesions biopsied because of a suspicious finding on a mammogram turn out to be benign. Mammograms are particularly difficult to interpret for women with dense breast tissue, who are at increased risk of breast cancer. The dense tissue interferes with the identification of abnormalities associated with tumors. This leads to higher rates of false-negative and false-positive findings in these women. In addition, optimal screening intervals are poorly defined because some tumors develop too quickly to be identified at the current screening intervals, especially in younger women.
The current limitations of mammography and other existing technologies (as described in this section) have been driving forces behind the efforts to improve mammography and other diagnostic techniques and to develop additional novel methods for the early detection of breast cancer. The purpose of the study presented in this report is to examine some of the many technologies under development and to identify potential impediments to the development of new breast cancer screening and diagnostic procedures. Many factors can influence the development, adoption, and use of medical technologies, including the availability of research funds, the regulatory approval process, coverage and reimbursement decisions, acceptability to the target population, and difficulties in ensuring broad access. Although many technologies described in this report are at a relatively early stage of development and it is difficult to predict their ultimate value or use, they all must clear many hurdles if they are to become part of the standard of care for women and thus play a role in reducing the toll of breast cancer.
In assessing new technologies, three distinct goals regarding early detection, listed below, need to be considered and addressed. These are revisited frequently throughout the remaining sections.
1. Identification of a higher percentage of women with an early stage of breast cancer. This aim could be achieved by improving the accuracy (sensitivity and specificity) and accessibility of mammography and also by developing other technologies that can identify cancers that are often missed by mammography.
2. Development of technologies that can detect early changes before the appearance of a true malignancy that increase a woman’s risk of developing invasive or metastatic breast cancer. A number of potential technologies could accomplish this aim, as described in next sections.
However, as these develop, the specificity (that is, the magnitude to which a woman’s risk is increased as a result of having a positive test) must be considered. Women may or may not consider a given magnitude sufficient to accept a given preventive strategy. Thus, it is important that investigators and physicians not assume that if a new technology identifies a breast abnormality, even one that appears, histologically, to represent cancer, it must move a patient to the right on the cancer continuum (as illustrated in Figure 1-6). In the absence of data, such an assumption would unfairly lead a patient to accept therapies that she previously believed were unacceptable.
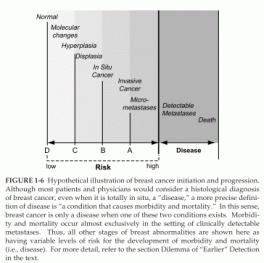
FIGURE 1-6 Hypothetical illustration of breast cancer initiation and progression.