Costly prostate therapy common when docs own the machine
A new study of an intensive and expensive form of prostate cancer therapy finds that doctors who stand to profit from the treatment are twice as likely to recommend it, even though there is no definitive evidence that it is better.
The treatment, known as intensity-modulated radiation therapy or IMRT, typically costs more than $31,000 while options costing about half that - or less - are available.
For instance, there is little evidence that it helps patients live longer, said the study’s author, Jean Mitchell of Georgetown University in Washington, D.C.
Published in the New England Journal of Medicine, the study was financed by the American Society for Radiation Oncology, whose members have done IMRT therapy for years but have been losing business to the urologists who have bought their own IMRT machines and hired radiation specialists to operate them.
Federal law prohibits what is known as self-referral, when doctors send patients for tests or treatment from which the physician stands to gain financially, but makes an exception for “in house” services.
The urologists are taking advantage of a loophole in federal law that doesn’t make it a conflict of interest for the doctors to benefit from such an arrangement, Mitchell said.
 The society released a statement quoting its chairman, Dr. Colleen Lawton, as saying the “study provides clear, indisputable evidence that many men are receiving unnecessary radiation therapy for their prostate cancer due to self-referral.”
The society released a statement quoting its chairman, Dr. Colleen Lawton, as saying the “study provides clear, indisputable evidence that many men are receiving unnecessary radiation therapy for their prostate cancer due to self-referral.”
The American Urological Association (AUA) responded by releasing a statement alleging the new study has “inherent biases and flawed methodologies” and questioning whether Mitchell “chose the control groups to arrive at results that were acceptable to the study’s sponsors.”
In July, when the U.S. Government Accountability Office (GAO) issued a report that reached a similar conclusion to that of the new study, the AUA and other urologist groups called that report “flawed and misleading,” saying the GAO “provided no evidence that patients were being provided radiation therapy inappropriately” by groups that had acquired IMRT.
The current study is only the latest to show that doctors tend to order more tests and treatments or to select particular treatments over others when they have a financial interest in those services.
“I don’t think this is any different than oncologists who might give a more expensive cancer drug because 6 percent of a more expensive drug brings more money into a practice than 6 percent of a cheaper drug,” said Dr. Bruce Roth, an oncologist at Washington University School of Medicine in St. Louis who was not involved in the new research. “It’s one more symptom of the underlying problem of reimbursing people for doing more stuff to patients.”
However, he told Reuters Health that the current study is incomplete because, for example, it did not attempt to survey urologists to determine their motivation for more referrals to IMRT.
“The wrong thing to look at is total cost,” he said. “It’s no doubt that (IMRT) costs more, but it’s probably better than conventional radiotherapy. But if you’re going to make the hypothesis that the urologists are doing it for financial reasons, you should look at the flow of money back to the physicians, not just the costs, because this technology doesn’t come free and all of that difference in dollars isn’t flowing into the urologists’ pockets.”
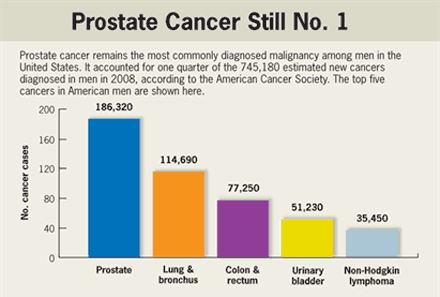 Nearly 241,000 U.S. men are diagnosed with prostate cancer each year and the 10-year survival rate is 98 percent. The tumor often grows so slowly, a man will die from some other cause before his prostate tumor has a chance to kill him.
Nearly 241,000 U.S. men are diagnosed with prostate cancer each year and the 10-year survival rate is 98 percent. The tumor often grows so slowly, a man will die from some other cause before his prostate tumor has a chance to kill him.
“You have to question (IMRT therapy) for men who are late 70s and into their 80s who are more likely to die from something other than their prostate cancer,” Mitchell said. “Medicare is paying a lot of money for aggressive treatment of prostate cancer where it’s basically not going to change anything in terms of giving a patient more years of life.”
The new study looked at Medicare claims for men who had just received a diagnosis of prostate cancer but the tumor had not spread. Treatment options in those circumstances include watching the tumor to see how fast it is growing, hormone treatment, surgical removal or implanting radioactive seeds into the tumor to try to kill it.
Mitchell analyzed records covering 2005 through 2010.
At the beginning of the period, before IMRT treatment accelerated, it was used in 13.1 percent of cases by urology groups that were destined by the end of the study to buy their own machines. Ultimately, those groups were sending 32.3 percent of their patients for IMRT therapy.
In contrast, among doctors who didn’t stand to make money from IMRT, the rate of referral barely grew, rising just 1.3 percentage points from 14.3 percent to 15.6 percent.
“Their behavior didn’t change at all,” Mitchell told Reuters Health in a telephone interview. “Given the lack of difference in clinical outcomes, if you’re a patient you have to ask yourself why you’re getting this extensive treatment. I know one of these centers has limousine service that picks people up 50 miles away.”
The July GAO report also looked at IMRT use on Medicare beneficiaries, covering a shorter time period from 2006 to 2010. It found urology groups that recommended IMRT for 37 percent of patients before they acquired the equipment themselves ended up referring 54 percent of patients for the treatment afterward.
Setting up a center typically requires a capital investment of $2 million, Mitchell said, citing marketing materials from one company that told urologists by treating 1.5 new patients a month with IMRT they can each generate $425,000 per year in additional revenue.
Roth said patients should be wary of such arrangements.
“It’s reasonable to query doctors when they are referred within a practice - whether it’s a laboratory or radiation therapy - to ask the doctor what the alternatives are, and I would probably get a second opinion,” he said. “If that second opinion told me, ‘They forgot to tell you about these two alternatives,’ then I would probably get treated somewhere else.”
“A lot of these people getting this treatment have no idea that their urologist has ownership” and patients should ask, Mitchell said. “I’d want to know whether am I getting this because it’s the best treatment, or am I getting it because it’s going to put more money in my referring physician’s pocket?”
In its statement Wednesday, the AUA said such ownership arrangements “should be transparent and in the patient’s best interest,” and “patients should be reassured that their urologic care will not be disrupted or penalized if they seek an alternate physician supplier or provider of IMRT.”
SOURCE: New England Journal of Medicine, online October 23, 2013.
###
Urologists’ Use of Intensity-Modulated Radiation Therapy for Prostate Cancer
In 2011, nearly 240,900 men in the United States received a new diagnosis of prostate cancer. Approximately 90% of these men had clinically localized disease, which was indolent in most cases. The relative 10-year survival rate among all men with prostate cancer is 98%.1,2 Primary definitive treatments include prostatectomy, external-beam radiation therapy, and brachytherapy. Alternatively, the patient may opt for a less aggressive (monitoring) approach that includes active surveillance or hormone therapy.
Despite substantial variation in reimbursement, evidence suggests that for low-risk disease, the three primary definitive treatments are clinically equivalent when measured in terms of survival. Moreover, clinical studies indicate that no single treatment approach is preferable with respect to the risk of adverse events and implications for quality of life. When selecting a treatment option, the patient will consider the recommendations of his physicians, the tumor attributes, whether monitoring is preferable to definitive treatment, the costs of and time required for treatment, potential side effects (urinary, bowel, and sexual dysfunction), and individual characteristics (e.g., age, race or ethnic group, and highest educational level attained). Lacking clinical expertise, the patient must rely on his treating physician to act as his agent in the health care decision-making process. Given this asymmetrical information problem, the physician’s recommendation has considerable influence on the patient’s decision.
Conclusions
Urologists who acquired ownership of IMRT services increased their use of IMRT substantially more than urologists who did not own such services. Allowing urologists to self-refer for IMRT may contribute to increased use of this expensive therapy. (Funded by the American Society for Radiation Oncology.)
Jean M. Mitchell, Ph.D.
N Engl J Med 2013; 369:1629-1637October 24, 2013DOI: 10.1056/NEJMsa1201141