Diagnostic Arguments of Ovarian Cysts in Prepubertal Girls
Diagnostic Arguments of Ovarian Cysts in Prepubertal Girls
Pelvic Ultrasonography
Pelvic ultrasonography is central to the management of ovarian cysts.
Classically, it is carried out by a suprapubic approach with a full bladder, which allows study not only of the cyst but of all the internal genital organs. An analysis of the cyst itself indicates the size, shape and even volume by measurement of the three diameters, the thickness and regularity of the wall and the nature of the cyst content. An anechogenic, purely liquid image with a thin, regular wall is in favor of a functional cyst (fig. 1, 2). Volume measurement is a basis for surveillance and for the decision of possible needle aspiration.
Ultrasonography is then indispensable for topographic localization to guide aspiration. An image which is not purely liquid raises problems of differential diagnosis. If the child is symptomatic, there may be a cystic complication such as hemorrhage or ovarian torsion. The mass may be a tumor with a cystic component, raising the problem of its benign or malignant nature. Certain morphological signs are informative: volume of the tissue component, wall thickness, growths, and rigid septations with angulated junctions. Morphological color Doppler and pulsed Doppler spectral imaging study may also be useful, since these techniques provide information on the vascularization of the mass, for example, by differentiating the avascular but echogenic content of a hemorrhagic cyst from hypervascularized tumoral tissue. At a later stage, ultrasonography is used to investigate the condition of the contralateral ovary and the appearance of the uterus, its dimensions and endometrium. This information is indispensable for therapeutic management.

Fig. 1. Functional cyst of the right ovary: purely fluid appearance, anechogenic and homogeneous with a thin, regular wall.
In the child and adolescent, ultrasonography is limited by the impossibility of using a vaginal approach. However, suprapubic sonography is generally sufficient for appropriate diagnosis and therapeutic management of ovarian cysts. Recourse to other imaging techniques (CT, MRI) is justified essentially in two circumstances: confirmation of the multitissular nature (fat, calcification) of a dermoid cyst and assessment of the extent of a mass that is tissular rather than liquid and suspected of being malignant.
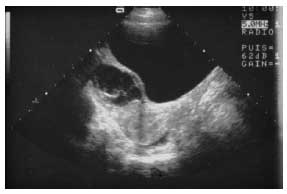
Fig. 2. Complex cyst: heterogeneous, septate appearance. The predominantly fluid component and the curved, pliable septations are in favor of a complicated benign cyst (intracystic hemorrhage in the process of resorption).
Hormonal Investigation
Plasma measurement of sex steroids (estradiol, testosterone and androgens) and basal or stimulated levels of the gonadotropins LH and FSH must be done in any endocrine syndrome.
Estradiol hypersecretion, associated with undetectable levels of LH and FSH that do not respond to stimulation after an LHRH test, confirms the peripheral origin of the autonomous independent gonadotropin secretion and suggests a secretory ovarian tumor. It is also useful to assess the secretory capacity of a cyst by measurement of estrogens and androgens in the aspiration fluid during the procedure or during percutaneous aspiration.
Tumor Markers
Tumor marker measurement is a useful diagnostic aid in lesions that are difficult to analyze by ultrasonography and in surveillance after tumor removal. Certain markers are specific for tumors with an embryonic component, such as α-fetoprotein in embryonic carcinomas and immature teratomas. β-Human chorionic gonadotropins (β-HCG) are more specific markers of choriocarcinomas and dysgerminomas. Elevated levels in pseudocystic tumors indicate a neoplastic component secreting various protein markers according to tumoral origin. However, we must stress the difficulty of interpreting CA-125 levels measured either in peripheral blood or in the cyst fluid after aspiration, as these levels may be high in functional cysts. Such measurements are more generally used in adult women.
Revision date: July 8, 2011
Last revised: by Janet A. Staessen, MD, PhD