How to Prepare the Patient with Diabetes for Exercise
Cardiovascular System
The incidence of vascular problems such as coronary artery disease is greatly elevated in patients with type 2 diabetes as compared to a healthy population.
Moreover, due to impaired sensation of anginal pain in many individuals uncontrolled exercise may precipitate grave consequences.
Cardiac autonomic neuropathy may be suspected in patients with resting tachycardia (>100/min), orthostasis (fall in blood pressure >20 mmHg during upright standing), or signs of autonomous nervous system dysfunction (skin, pupils, gastrointestinal, genitourinary systems).
In order to minimize harmful side effects of physical exercise in patients with type 2 diabetes they should undergo a careful evaluation prior to increasing their level of physical activity on a regular basis.
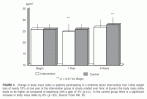 FIGURE 4 Change in body mass index in patients participating in a multirisk factor intervention trial.
FIGURE 4 Change in body mass index in patients participating in a multirisk factor intervention trial.
Initial weight loss of nearly 10% at one year in the intervention group is slowly eroded over time; at 6 years the body mass index tends to be higher as compared to beginning with a gain of 4% (p:n.s.). In the control group there is a significant increase in body mass index by 8% (p
< 05). Source: From Ref. 55.The following recommendations have been modified from the Health Professional’s Guide to Diabetes and Exercise. A graded treadmill exercise test should be performed in all patients in order to detect myocardial ischemia, and to determine the individual cardiopulmonary fitness and exercise tolerance.
The optimal training heart rate is determined as 80% of the maximal symptom free heart rate. In patients with questionable results alternative stress tests (stress echocardiography, radionuclide stress test) can be employed to increase the diagnostic precision. In patients with typical anginal symptoms or significant ST-segment changes invasive diagnostic coronary angiography is indicated. Patients with hemodynamically significant coronary lesions should undergo either interventional or surgical treatment as indicated prior to embarking on an exercise program.
Long-standing diabetes may result in significant impairment of myocardial function and cause symptoms and signs of congestive heart failure (diabetic cardiomyopathy) (35, 41).
Myocardial hypertrophy combined with an increase in interstitial fibrosis may cause diastolic heart failure, indistinguishable from systolic heart failure on clinical grounds.
Echocardiography is used to assess left ventricular performance, rule out valvular heart disease and determine left ventricular compliance in patients with myocardial hypertrophy.
The magnitude of left ventricular hypertrophy is correlated to the degree and duration of hyperinsulinemia, whereas the degree of left ventricular dysfunction seems to be mainly the result of hyperglycemia.
Peripheral Arterial Disease
Intermittent claudication and trophic changes of the feet are indicators of Peripheral arterial disease and should prompt evaluation by duplex sonography and treadmill testing. The presence of palpable pulses does not rule out microangiopathy.
Retinopathy
Patients with proliferative diabetic retinopathy are at risk to develop vitreous hemorrhage or traction retinal detachment during strenuous physical exercise. Their activity should be tailored to their individual need and avoid anaerobic, strenuous exercises. Swimming, walking, or bicycle ergometry are alternative activities recommended for these patients.
Peripheral Neuropathy
Loss of peripheral sensation particularly in the feet may ultimately result in skin ulcerations and fractures. Peripheral neuropathy can be detected by evaluating the tendon reflexes, the vibratory sense, and touch sensation. Weight bearing and repetitive exercises should be limited in these patients.
Gerhard Schuler and Axel Linke
Department of Internal Medicine/Cardiology, University of Leipzig, Leipzig, Germany
REFERENCES