Health Centers > Diabetes Center > Diabetes Mellitus Management
Diabetes Mellitus Management
Primary treatment goals for diabetes patients include the achieving of blood glucose levels that are as close to normal as possible and the prevention of diabetic complications. Other goals are normal growth and development, normal body weight, the avoidance of sustained hyperglycemia or symptomatic hypoglycemia, the prevention of diabetic ketoacidosis and nonketotic acidosis, and the immediate detection and treatment of long-term diabetic complications.
Diabetes Mellitus and Oral Diseases
Diabetes Introduction
Diabetes Epidemiology and classification
Diabetes Pathophysiology
Clinical Presentation, Laboratory findings, and Diagnosis
Diabetes Complications
Diabetes Management
L Introduction
L Oral Agents
L Insulin
Oral Diseases and Diabetes
Periodontal Health and Diabetes
Dental Management of the Diabetic Patient
Conclusion
References
Diet, exercise, weight control, and medications are the mainstays of diabetic care. Obesity is very common in type 2 diabetes and contributes greatly to insulin resistance. Weight reduction and exercise improve tissue sensitivity to insulin and allow its proper use by target tissues. The primary medication used in type 1 diabetes management is insulin, on which the type 1 diabetic patient is dependent for survival. Type 2 diabetic individuals frequently take oral medications although many also use insulin to improve glycemic control.
Medical management and the goals of therapy for diabetes have changed since the publication of the Diabetes Control and Complications Trial (DCCT) in 1993. This prospective randomized controlled multicenter clinical trial compared the effects of intensive insulin therapy aimed at achieving the near normalization of glycemia with the effects of conventional insulin therapy on the initiation and progression of complications in patients with type 1 diabetes. The conventional control group took 1 or 2 insulin injections each day while the intensive control group took 3 or 4 injections daily or used a subcutaneous insulin infusion pump. The results showed that the intensive group had much better glycemic control during the 3- to 9-year follow-up period.
The risk of developing retinopathy decreased by 76% in intensively managed patients when compared to conventional control group patients. Clinical and laboratory signs and symptoms of nephropathy and neuropathy decreased by 54 to 60%. Macrovascular complications also decreased significantly. The dramatic benefits of intensive insulin therapy led the American Diabetes Association to issue a position statement declaring that the primary treatment goal in type 1 diabetes should be to attain blood glucose control "at least equal to that in the intensively treated cohort" of the DCCT.
Several recent studies have also shown reductions in diabetic complications for intensively managed type 2 diabetic patients. In one 6-year study, maintenance of near-normal glycemia resulted in a decrease of 54 to 70% in the risk of microvascular and macrovascular complications for these patients, compared to conventional controls. Since type 2 diabetic patients make up about 90% of all diabetic Americans, these studies have the potential to affect millions of people. Diabetic patients are increasingly motivated to improve their glycemic control, and physicians have intensified diabetic management in response to recent research.
Oral Agents
A number of different oral agents are available for treating diabetes; most of these are taken by those with type 2 diabetes.
The Hypoglycemic States
Spontaneous hypoglycemia in adults is of two principal types: fasting and postprandial. Symptoms begin ...
The first-generation sulfonylureas, once the only drugs available for treating type 2 diabetes, are not used much today. They have been replaced with second-generation agents that are more potent, have fewer drug interactions, and produce less significant side effects. Sulfonylureas stimulate pancreatic insulin secretion. The increased quantity of secreted insulin helps counteract the qualitative decrease in tissue sensitivity to insulin, allowing greater glucose entry into target cells and thereby lowering blood glucose levels. Sulfonylureas generally have a relatively long duration of action of 12 to 24 hours, depending on the drug, and are taken once or twice per day. Hypoglycemia is a major side effect of sulfonylureas. In patients taking these agents, food intake must be adequate to prevent glucose levels from falling too low.
Like the sulfonylureas, repaglinide stimulates pancreatic insulin secretion. However, its pharmacodynamic properties and mechanism of action are different from those of the sulfonylureas. Repaglinide is rapidly absorbed, reaches peak plasma levels in 30 to 60 minutes, and is then rapidly metabolized. The drug is taken with meals and lowers the peaks of postprandial plasma glucose common with type 2 diabetes to a much greater degree than the sulfonylureas are able to do.
Metformin is a biguanide agent that lowers plasma glucose mainly by preventing glycogenolysis in the liver. Metformin also improves insulin use, counteracting the insulin resistance seen with type 2 diabetes. Because metformin does not stimulate increased insulin secretion, hypoglycemia is much less common with this drug.
The thiazolidinedione agents troglitazone, rosiglitazone, and pioglitazone act to increase tissue sensitivity to insulin, thus increasing glucose utilization and decreasing blood glucose levels. These drugs also decrease hepatic gluconeogenesis. Like metformin, the thiazolidinediones generally do not cause hypoglycemia.
Acarbose has a mechanism of action that is unlike that of the other agents used in diabetes management. Acarbose is taken with meals, and it slows the digestion and uptake of carbohydrates from the gut. This serves to lower postprandial plasma glucose peaks. Acarbose does not cause hypoglycemia, but if the delayed carbohydrate absorption occurs in a patient whose plasma insulin levels are increasing due to the injection of insulin or the use of a sulfonylurea, the level of glucose in the bloodstream will not be sufficient to prevent hypoglycemia.
Insulin
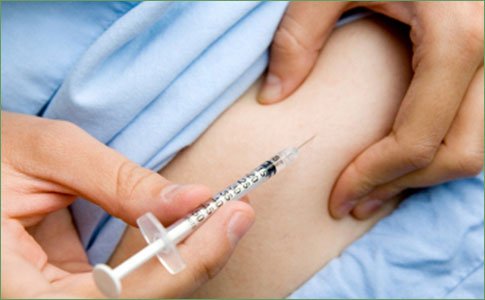
All type 1 diabetic patients use exogenous insulin, as do many with type 2 diabetes. Insulin is taken via subcutaneous injection, most often with a syringe. Insulin infusion pumps deliver insulin through a subcutaneous catheter. There are a variety of insulin preparations available; they vary in their onset, peak, and duration of activity and are classified as long-, intermediate-, short-, or rapid-acting. Although beef and pork insulin species are still available, most individuals use human insulin preparations today.
Ideally, the use of exogenous insulin provides an insulin profile similar to that seen in a nondiabetic individual, with a continuous basal level of insulin availability augmented by increased availability following each meal. There is no single insulin preparation that can achieve this goal with only one or two injections per day. Combinations of different insulin preparations taken three or more times daily or the use of a subcutaneous infusion pump more closely approximate the ideal profile, but even with such regimens, blood glucose levels are often unstable.
Ultralente insulin is the longest-acting insulin. Commonly called "peakless" insulin, Ultralente has a very slow onset of action, minimal peak activity, and a long duration of action. It is usually taken to mimic the basal metabolic rate of insulin secreted from a normally functioning pancreas. The intermediate-acting insulins (lente and neutral protamine Hagedorn [NPH]) take several hours after injection to begin having an effect. Peak activity varies among individuals and sites of injection but generally occurs between 4 and 10 hours after injection. Thus, a patient who injects intermediate-acting insulin in the early morning will reach peak plasma insulin levels at about lunchtime. Regular insulin is short acting, with an onset of activity at about 30 minutes to 1 hour after injection and a peak activity at 2 to 3 hours. The rapid-acting insulin called lispro insulin is rapidly absorbed, becomes active about 15 minutes after injection, and is at peak activity at 30 to 90 minutes. Rapid- and short-acting insulins are usually taken just prior to or during meals. Thus, regular insulin taken prior to breakfast will peak at about midmorning; when taken prior to lunch, it will peak during the midafternoon.
The most common complication of insulin therapy is hypoglycemia, a potentially life-threatening emergency. While hypoglycemia may occur in patients who are taking oral agents such as sulfonylureas, it is much more common in those who are using insulin. Intensified treatment regimens for diabetes increase the risk of hypoglycemia. Thus, the long-term benefit of reduced diabetic complications seen with intensive treatment must be weighed against the increased risk of symptomatic low blood glucose. In the DCCT, the incidence of severe hypoglycemic events in which the patient became unconscious or required the assistance of another person was three times greater in the intensively managed cohort than in the conventional control group. One-third of the severe hypoglycemic episodes resulted in seizure or loss of consciousness. In addition, 36% of the episodes occurred with no warning symptoms for the patient.
The phenomenon known as "hypoglycemia unawareness" is more common in diabetic patients with good glycemic control than in those with poor control. Hypoglycemia unawareness is characterized by an inability to perceive the warning symptoms of hypoglycemia until the blood glucose drops to very low levels. Signs and symptoms of hypoglycemia are most common when blood glucose levels fall to < 60 mg/dL, but they may occur at higher levels in diabetic patients with chronic poor metabolic control. In people with hypoglycemia unawareness, glucose levels can fall to 40 mg/dL or lower before an individual "feels" hypoglycemic.