Gene therapy for human skin disease produces long-term benefits
Stem cell-based gene therapy holds promise for the treatment of devastating genetic skin diseases, but the long-term clinical outcomes of this approach have been unclear. In a study online December 26th in the ISSCR’s journal Stem Cell Reports, published by Cell Press, researchers evaluated a patient with a genetic skin disorder known as epidermolysis bullosa (EB) nearly seven years after he had undergone a gene therapy procedure as part of a clinical trial. The study revealed that a small number of skin stem cells transplanted into the patient’s legs were sufficient to restore normal skin function, without causing any adverse side effects.
“These findings pave the way for the future safe use of epidermal stem cells for combined cell and gene therapy of epidermolysis bullosa and other genetic skin diseases,” says senior study author Michele De Luca of the University of Modena and Reggio Emilia.
EB is a painful condition that causes the skin to be very fragile and to blister easily, and it can also cause life-threatening infections. Because there is no cure for the disease, current treatment strategies focus on relieving symptoms. To evaluate stem cell-based gene therapy as a potential treatment, De Luca and his colleagues previously launched a phase I/II clinical trial at the University of Modena and recruited an EB patient named Claudio. The researchers took skin stem cells from Claudio’s palm, corrected the genetic defect in these cells, and then transplanted them into Claudio’s upper legs.
In the new study, De Luca and his team found that this treatment resulted in long-term restoration of normal skin function. Nearly seven years later, Claudio’s upper legs looked normal and did not show signs of blisters, and there was no evidence of tumor development. Remarkably, a small number of transplanted stem cells was sufficient for long-lasting skin regeneration.
Even though Claudio’s skin had undergone about 80 cycles of renewal during this time period, the transplanted stem cells still retained molecular features of palm skin cells and did not adopt features of leg skin cells. “This finding suggests that adult stem cells primarily regenerate the tissue in which they normally reside, with little plasticity to regenerate other tissues,” De Luca says. “This calls into question the supposed plasticity of adult stem cells and highlights the need to carefully chose the right type of stem cell for therapeutic tissue regeneration.”
###
Epidermolysis bullosa
Epidermolysis bullosa (ep-ih-dur-MOL-uh-sis buhl-LO-sah) is a group of skin conditions whose hallmark is blistering in response to minor injury, heat, or friction from rubbing, scratching or adhesive tape. Four main types of epidermolysis bullosa exist, with numerous subtypes. Most are inherited.
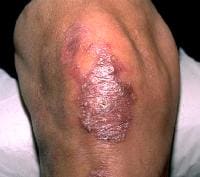 Most types of epidermolysis bullosa initially affect infants and young children, although some people with mild forms of the condition don’t develop signs and symptoms until adolescence or early adulthood. Mild forms of epidermolysis bullosa may improve with age, but severe forms may cause serious complications and can be fatal.
Most types of epidermolysis bullosa initially affect infants and young children, although some people with mild forms of the condition don’t develop signs and symptoms until adolescence or early adulthood. Mild forms of epidermolysis bullosa may improve with age, but severe forms may cause serious complications and can be fatal.
There’s currently no cure for epidermolysis bullosa. For now, treatment focuses on addressing the symptoms, including pain prevention, wound prevention, infection and severe itching that occurs with continuous wound healing.
 Stem Cell Reports, De Rosa et al.: “LONG-TERM STABILITY AND SAFETY OF TRANSGENIC CULTURED EPIDERMAL STEM CELLS IN GENE THERAPY OF JUNCTIONAL EPIDERMOLYSIS BULLOSA.”
Stem Cell Reports, De Rosa et al.: “LONG-TERM STABILITY AND SAFETY OF TRANSGENIC CULTURED EPIDERMAL STEM CELLS IN GENE THERAPY OF JUNCTIONAL EPIDERMOLYSIS BULLOSA.”
What causes epidermolysis bullosa simplex?
The top layer of skin (the epidermis) is composed of layers of cells. Each cell has an internal skeleton formed from proteins (keratins), giving it strength and shape. In EB simplex, there is a weakness in one of these proteins (usually type 5 or type 14 keratin, but very occasionally another protein called plectin), which causes affected cells to be less resilient and to rupture when subjected to even minor physical stress. When the cells break, they separate from each other, fluid accumulates between them and a blister forms.
Weakness of the protein is caused by a minor abnormality (a mutation) in the gene responsible for producing that protein. A variety of such mutations have been identified in EB simplex, some of which are common amongst sufferers of the condition while others are only found in single families.
Is epidermolysis bullosa simplex hereditary?
Yes. It is inherited in a dominant fashion. This means that one parent of an affected person will also usually have the condition, although it is possible for EB simplex to appear for the first time in a person who has no other affected family member. Anyone who has EB simplex can pass the condition on to his or her children: there is a 50% chance that the child of an affected parent will inherit the blistering tendency. EB simplex affects men and women equally. It is not an infection, it is not contagious and it is not due to an allergy.
###
Mary Beth O’Leary
.(JavaScript must be enabled to view this email address)
617-397-2802
Cell Press