Normal cognitive changes in aging
Cognitive abilities include perception, memory, judgment, perceptual speed, spatial manipulation and reasoning. Both cross sectional and longitudinal studies have shown that different cognitive abilities have different developmental trajectories across the lifespan, and may be grouped into two broad types.
The first type is described as ‘crystallised’ and involves accumulated knowledge and expertise and relies on long term memory. Crystallised abilities are assessed with tests of vocabulary, word knowledge, general knowledge, understanding proverbs, and measures of occupational expertise.
The second type are known as ‘fluid’ and involve novel problem solving, spatial manipulation, mental speed, and identifying complex relations among stimulus patterns.
These are usually measured with tests that involve identifying the next in a series of abstract patterns, matrices or a series of numbers. Fluid abilities rely on short term memory storage while processing information.
Normal cognitive aging
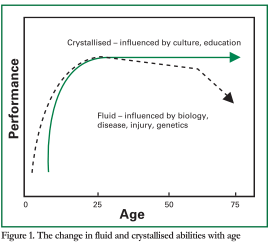
As shown in Figure 1, the developmental trajectory of fluid abilities is thought to follow neurological maturation, peaking in the mid 20s and thereafter declining gradually until the 60s when a more rapid decline takes place. Fluid abilities are affected by neurological insult, genetics and biological aging processes. In contrast, crystallised abilities increase during the lifespan through education, occupational and cultural experience and exposure to culture and intellectual pursuits. They are less affected by aging and disease and often remain intact in the early stages of dementia or after brain injury. The rate of increase in crystallised abilities is thought to slow in late adulthood, and there is some evidence they may decrease slowly from the ninth decade onward. The observation that older adults often have intact long term memory but poor short term memory, reflects the different effects of age on these abilities.
Behavioural changes also accompany normal cognitive aging. Older adults are more variable in their responses on cognitive tests than younger adults. For example, on a test of reaction time, older adults may have a higher mean performance indicating that overall they are slower than younger adults, but they will also have more very long trials and very short trials indicating greater variability about the mean. Compared with younger adults, older adults are more likely to fluctuate in their performance from day-to-day, and week-to-week, and those with neurological conditions fluctuate more than healthy older adults. Cognitive aging is also characterised by generalised behavioural slowing, both in laboratory tasks and everyday situations. Older adults also have more difficulty selectively attending to information and inhibiting irrelevant information or stimuli. This has been linked with frontal lobe atrophy in aging.
How much cognitive decline is normal?
 There are large individual differences in the amount of decline experienced by individuals and in the patterns of decline across different abilities within an individual. At a group level, there is a decline of between one and two standard deviations (15-30 IQ points) in fluid type abilities between the ages of 20-70. After then, the average decline in fluid abilities accelerates to about 0.5 of a standard deviation per decade.
There are large individual differences in the amount of decline experienced by individuals and in the patterns of decline across different abilities within an individual. At a group level, there is a decline of between one and two standard deviations (15-30 IQ points) in fluid type abilities between the ages of 20-70. After then, the average decline in fluid abilities accelerates to about 0.5 of a standard deviation per decade.
A practical indication of the amount of decline in normal aging can be gained from the norms for commonly used cognitive tests. On a 33 item vocabulary test, there will be no difference in the average score for a 25 year old and a 70 year old. However, on test of recall of digits in the order in which they are presented, the average 25 year old will recall about seven, whereas the average 65 year old will recall about 5. On a test of coding speed conducted within a time limit of 90 seconds, the average 25 year old will code about 78 items correctly, whereas the average 70 year old will code about 51 items correctly.
Clinical evaluation of premorbid cognitive function
The significance of decline in cognitive abilities is partially determined by the individual’s previous level of cognitive function. This is called their ‘premorbid’ intelligence, and is assessed by measures of verbal reasoning and word knowledge (crystallised abilities). Those who start at a low level may reach the threshold for a cognitive disorder after a small amount of decline, whereas those who start at a higher level will need to decline more before they are diagnosed as clinically impaired. Any assessment of cognitive impairment by a neuropsychologist would involve assessing premorbid cognitive function through psychometric testing and interview. Information about previous occupational level, interests, educational level from the individual, and an informant, additionally contribute to a clinical estimate of premorbid ability.
Memory complaints in normal aging
Memory complaints are common among older adults and are more prevalent among the very old, women, and those with low levels of education. A number of studies have been conducted to determine whether individuals who complain of memory difficulties have memory disorders or are at greater risk of developing memory disorders or dementia.
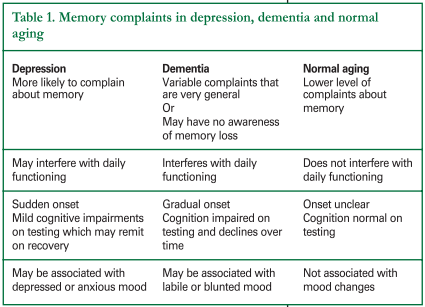
Results of individual studies have been inconsistent and a recent review reported that self referrals for memory complaints are not a good indicator of cognitive impairment and are more likely to be associated with depression in older adults. On the other hand, memory complaints are a diagnostic criteria for mild cognitive impairment (MCI) and in patients with cognitive impairment, memory complaints are predictive of cognitive decline. Table 1 outlines the different patterns accompanying memory complaints in normal aging, depression and dementia.
Mild cognitive impairment
While moderate to severe cognitive deficits impair the individual’s capacity to conduct activities of daily living, the cognitive changes in the preclinical stages of dementia do not. Over the past 15 years, a large amount of research has been directed toward developing screening tests and criteria to identify individuals in the preclinical phase of dementia. The diagnosis of MCI has been developed for research studies, particularly drug trials that focus on the detection and early intervention of dementia. The criteria for MCI include: