Unipolar disorders
Unipolar disorders are major depressive disorder and dysthymic disorder.
Major Depressive Disorder
Major depressive disorder is diagnosed after a single episode of major depression (Table 2-2). It is characterized by emotional changes, primarily depressed mood, and by so-called vegetative changes, consisting of alterations in sleep, appetite, and energy levels.
Epidemiology
The lifetime prevalence (will occur at some point in a person’s life) rate for major depressive disorder is 5% to 20%. The female-male ratio is 2: 1. Race distributions appear equal, and socioeconomic variables do not seem to be a factor. The incidence (rate of new cases) is greatest between the ages of 20 and 40 and decreases after the age of 65.
Etiology
Psychological theories of depression generally view interpersonal losses (actual or perceived) as risk factors for developing depression. In fact, available evidence suggests that childhood loss of a parent or loss of a spouse are associated with depression.
Classic psychoanalytic theories center on ambivalence toward the lost object (person), although more recent theories focus on the critical importance of the object relationship in maintaining psychic equilibrium and self-regard. The cognitive-behavioral model views cognitive distortions as the primary events that foster a negative misperception of the world, which in turn generate negative emotions. The learned helplessness model (based on animal studies) suggests that depression arises when individuals come to believe they have no control over the stresses and pains that beset them.
Biologic, familial, and genetic data support the idea of a biologic diathesis in the genesis of depression. Genetic studies show that depression is found to be concordant more often in monozygotic twins than in dizygotic twins. Unipolar depression in a parent leads to an increased incidence in the offspring of both unipolar and bipolar mood disorders.
Neurotransmitter evidence points to abnormalities in amine neurotransmitters as mediators of depressive states: The evidence is strongest for deficiencies in norepinephrine and serotonin.
Neuroendocrine abnormalities in the hypothalamic-pituitary-adrenal axis are often present In depression and suggest a neuroendocrine link.
Sleep disturbances are near universal complaints in depressed persons. Objective evidence from sleep studies reveals that deep sleep (delta sleep, stages 3 and 4) is decreased in depression and that rapid-eye-movement (REM) sleep alterations include increased time spent in REM and earlier onset of REM in the sleep cycle (decreased latency to REM).
Clinical Manifestations
History and Mental Status Examination
A major depressive disorder is diagnosed if a patient has at least one episode of major depression and does not meet criteria for bipolar disorder or etiologic mood disorder. Major depression is characterized by emotional and vegetative changes. Emotional changes most commonly include depressed mood with feelings of sadness, hopelessness, guilt, and despair. Irritability may be the primary mood complaint in some cases. Vegetative symptoms include alterations in sleep, appetite, energy, and libido.
Major depression is frequently recurrent. The usual duration of an untreated episode (Fig. 2-1A) is 6 to 12 months. Fifteen percent of patients diagnosed with major depression die by suicide at some point in their lifetime.
Differential Diagnosis
Mood disorders secondary to (induced by) medical illnesses or substance abuse are the primary differential diagnoses. Psychotic depression must be differentiated from schizophrenia; negative symptoms of schizophrenia can mimic depression. Persons with major depression may eventually meet criteria for bipolar disorder.
Management
Depression is responsive to psychotherapy and pharmacotherapy. Milder cases may be treated with brief psychotherapy interventions alone. For more severe cases, antidepressant medications combined with psychotherapy are superior to medications or psychotherapy alone. Among the psychotherapies, supportive, cognitive-behavioral, and brief interpersonal therapies have the most data to support their efficacy. There is a long tradition of psychodynamic psychotherapy in treating depression, although it has not been empirically well studied.
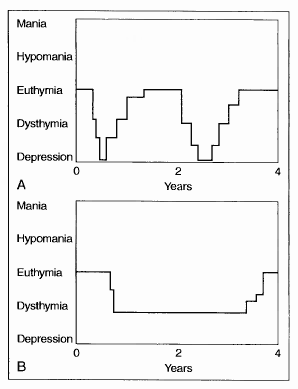
Figure 2-1 . Unipolar mood disorders. (A) Major depressive disorder and (B) dysthymic disorder.
There are many classes of antidepressants available that are effective and are usually chosen according to side-effect profiles. Presently, available classes of antidepressants include tricyclic antidepressants, selective serotonin reuptake inhibitors, monoamine oxidase inhibitors, and atypical antidepressants. In addition, lithium, thyroid hormone, and psychostimulants may be used as augmentative treatments. Electroconvulsive therapy (ECT) is used in psychotic, severe, or treatment refractory depressions or when medications are contraindicated (e.g., in the elderly or debilitated). Antipsychotic medications are an essential adjunct to antidepressants in psychotic depressions. Anxiolytics may be used as adjuncts to antidepressants in depression with high levels of anxiety, although more sedating antidepressants may suffice. Phototherapy can be used for seasonal mood disorders.
KEY POINTS
1. Major depression is a unipolar mood disorder.
2. It is often recurrent.
3. Major depression has a 1 S% suicide rate.
4. Combined psychotherapy and pharmacotherapy are the best treatment.
Revision date: July 9, 2011
Last revised: by Sebastian Scheller, MD, ScD