Bipolar disorders
The bipolar disorders are bipolar 1 disorder, bipolar II disorder, and cyclothymia.
Bipolar I Disorder
Bipolar I disorder is the most serious of the bipolar disorders and is diagnosed after at least one episode of mania (Table 2-3). Patients with bipolar I disorder typically also have major depressive episodes in the course of their lives.
Epidemiology
The lifetime prevalence is 0.4% to 1.6% and the male-female ratio is equal. There are no racial variations in incidence.
Etiology
Genetic and familial studies reveal that bipolar I disorder is associated with increased bipolar I, bipolar II, and major depressive disorders in first-degree relatives. X linkage has been demonstrated in some studies but remains controversial. Mania can be precipitated by psychosocial stressors, and there is evidence that sleep/wake cycle perturbations may predispose a person to mania.
Clinical Manifestations
History and Mental Status Examination
Bipolar J disorder is defined by the occurrence of mania (or a mixed episode). A single manic episode is sufficient to meet diagnostic requirements; most patients, however, have recurrent episodes of mania typically intermixed with depressive episodes. The criteria for a manic episode are outlined in Table 2-3.
The first episode of mania usually occurs in the early 20s. Manic episodes are typically briefer than depressive episodes. The transition between mania and depression occurs without an intervening period ofeuthymia in abouttwo of three patients (Fig. 2-2A).
Lifetime suicide rates range from 10% to 15%.
Differential Diagnosis
Mania may be induced by antidepressant treatment, including antidepressant medications, psychostimulants, ECT, and phototherapy. When this occurs, the patient is diagnosed with substance-induced mood disorder, not bipolar disorder. Mood disorder due to a general medical condition is the other major differential consideration. Schizo affective disorder, borderline personality disorder, and depression with agitation are also considerations.
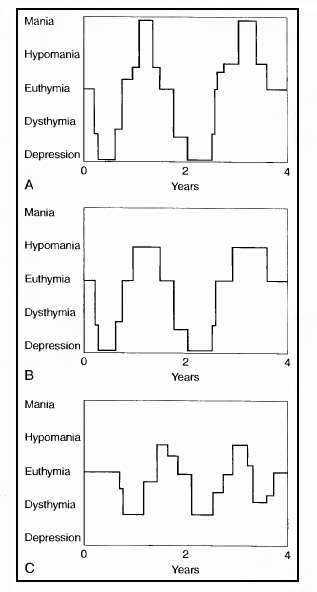
Figure 2-2. Bipolar mood disorders. (A) bipolar I disorder, (B) bipolar II disorder, (C) cyclothymic disorder.
Management
Persons experiencing a manic episode often have poor insight and resist treatment. Pharmacological interventions for acute mania include antipsychotics in conjunction with benzodiazepines (for rapid tranquilization) and initiation of mood stabilizer medication. Antipsychotics are frequently used in mania with and without psychotic features. Lithium is the most commonly used mood stabilizer, but valproic acid is quite effective and is more effective for the rapid-cycling variant of mania. Carbamazepine, lamotrigine, gabapentin, and long-acting benzodiazepines are used if first-line treatments fail. ECT is used in patients with medication intolerance and where a more immediate response is medically or psychiatrically needed.
Mood stabilizer maintenance therapy is essential in preventing the recurrence of mania and appears to decrease the recurrence of depression. Psychotherapy is used to encourage medication compliance, to help patients come to terms with their illness, and to help repair some of the interpersona1 damage done while ill (e.g., infidelity, hostility, squandering money). Care must be taken when prescribing antidepressants for depression or dysthymia because of their role in prompting more severe or more frequent manic episodes.
KEY POINTS
1. Bipolar I disorder is a biphasic mood disorder.
2. It is cyclic.
3. It has a suicide rate of 10% to 15%.
4. Maintenance treatment with mood stabilizers is required.
Revision date: June 18, 2011
Last revised: by Andrew G. Epstein, M.D.