Adults with eosinophilic esophagitis should consider a diet change
Dietary elimination is a successful method of treatment for adults with eosinophilic esophagitis (EoE), according to a new study1 in Clinical Gastroenterology and Hepatology, the official clinical practice journal of the American Gastroenterological Association.
“By eliminating specific foods from patients’ diets, symptoms improved in 71 percent of patients, and endoscopic appearance improved in 54 percent,” said lead study author, W. Asher Wolf, MD, MPH, and co-author Evan S. Dellon, MD, MPH, from the division of gastroenterology and hepatology, University of North Carolina School of Medicine. “These strong results support dietary elimination therapy as an effective treatment for adults suffering from EoE.”
Researchers conducted a retrospective cohort study using the University of North Carolina EoE database from 2006-2012. Subjects were 18 years of age or older and diagnosed with EoE based on consensus guidelines. The study analyzed two diet elimination plans. For the first therapy - targeted elimination - patients underwent evaluation with skin prick testing, and foods that had a positive reaction, as well as any foods identified by patient self-report as being possible triggers regardless of the severity of response, were eliminated. For the other diet prescribed - the six-food elimination diet - dairy, wheat, eggs, soy, nuts and seafood were eliminated from the patient’s diet regardless of skin-prick test results.
Sixty-eight percent of patients who received targeted diet elimination experienced symptom improvement, compared with 78 percent of those who followed a six-food elimination diet plan. For those subjects who responded to six-food elimination diet, one food (or food group) was added back every six weeks, and endoscopy was repeated. Eggs and dairy were found to be the most common triggers, both impacting 44 percent of patients.
Importantly, because this study included patients who failed steroid therapy, the overall study population likely represents harder to treat EoE patients. The success of dietary elimination in this population indicates its utility for therapy in patients resistant to steroids.
Because EoE is an allergen/immune mediated condition, dietary elimination therapy has been extensively studied in children and is now a well-established modality in pediatric patients. Until recently, the utility of dietary elimination was unknown in adults. However, evidence is mounting; a June 2014 Gastroenterology meta-analysis2 reported that dietary interventions are effective in producing histologic remission in both pediatric and adult patients with EoE.
Eosinophilic Esophagitis
Eosinophilic esophagitis (EE) has only recently been recognized, and it is being found in many allergic children. Its symptoms mimic gastroesophageal reflux disease (GERD). It is an allergic inflammatory reaction of the esophagus, the muscular tube that carries food from the throat to the stomach.
To distinguish between GERD and EE, a biopsy of the esophagus and GERD studies are preformed. In EE, high levels of eosinophils are detected in the esophagus only, and not other parts of the digestive tract. EE is simply an inflammation of the esophagus caused by the presence of high levels of eosinophils.
Eosinophils are a type of white blood cell that are not normally found in the esophagus. High levels of eosinophils often indicate an allergic response.
Studies have revealed that symptoms from EE do not improve with aggressive acid blockage therapy used for the treatment of GERD. They do improve with an elimination diet or corticosteroid treatment. Skin prick testing and patch testing can help identify which foods might contribute to this disease. The foods most commonly associated with EE are cow’s milk, soy, egg and wheat. Airborne allergens may also be a contributing factor. Many children with this disorder have more than one allergy problem.
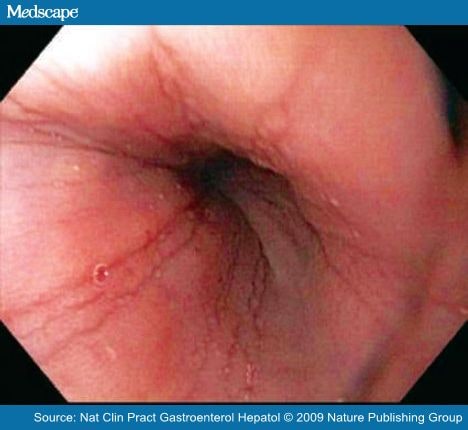 While the current treatment of swallowed corticosteroids acts topically to reduce esophageal inflammation, no corticosteroid is FDA approved, not all patients respond and, when discontinued, EoE almost always recurs. As such, there is a growing need for a new treatment for patients with EoE.
While the current treatment of swallowed corticosteroids acts topically to reduce esophageal inflammation, no corticosteroid is FDA approved, not all patients respond and, when discontinued, EoE almost always recurs. As such, there is a growing need for a new treatment for patients with EoE.
Further research should emphasize which factors can predict effective dietary therapy, to target therapy to patients most likely to respond.
###
Eosinophilic esophagitis is a chronic immune system disease caused by a buildup of white blood cells in the lining of the esophagus. This build up, which is a reaction to food, allergens or acid reflux, can inflame or injure esophageal tissue, making swallowing and eating a challenge for patients.
About the AGA Institute
The American Gastroenterological Association is the trusted voice of the GI community. Founded in 1897, the AGA has grown to include 17,000 members from around the globe who are involved in all aspects of the science, practice and advancement of gastroenterology. The AGA Institute administers the practice, research and educational programs of the organization. http://www.gastro.org.
About Clinical Gastroenterology and Hepatology
The mission of Clinical Gastroenterology and Hepatology is to provide readers with a broad spectrum of themes in clinical gastroenterology and hepatology. This monthly peer-reviewed journal includes original articles as well as scholarly reviews, with the goal that all articles published will be immediately relevant to the practice of gastroenterology and hepatology.
###
Rachel Steigerwald
.(JavaScript must be enabled to view this email address)
301-272-1603
American Gastroenterological Association