A treatment for one form of albinism?
Individuals with oculocutaneous albinism, type 1 (OCA1) have white hair, very pale skin, and light-colored irises because they have none, or very little, of the pigment melanin in their skin, hair, and eyes. Affected individuals have impaired eyesight and a substantially increased risk of skin cancer. Current treatment options are limited to attempts to correct eyesight and counseling to promote the use of sun protective measures. A team of researchers, led by Brian Brooks, at the National Eye Institute, Bethesda, has now generated data in mice that provide hope for a new treatment for a subset of patients with OCA1.
OCA1 is caused by mutations in the gene Tyr that result in either complete loss of activity of the protein tyrosinase (which is key to the generation of melanin) or the generation of a tyrosinase protein with reduced activity. Brooks and colleagues found that treating mice that model OCA1 caused by mutations that generate a tyrosinase protein with reduced activity (OCA-1B) with nitisinone, which is already FDA-approved for treating a blood condition known as hereditary tyrosinemia type 1, increases their eye and hair pigmentation. They therefore suggest that nitisinone could improve pigmentation in patients with OCA-1B and potentially ameliorate their vision loss.
In an accompanying commentary, Seth Orlow and Prashiela Manga, at New York University School of Medicine, New York, discuss the inspired study of Brooks and colleagues but caution that there are issues that might limit the use of nitisinone as a treatment for OCA-1B.
TITLE: Nitisinone improves eye and skin pigmentation defects in a mouse model of oculocutaneous albinism
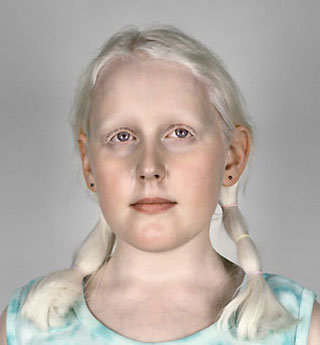
The word “albinism” refers to a group of inherited conditions. People with albinism have little or no pigment in their eyes, skin, or hair. They have inherited altered genes that do not make the usual amounts of a pigment called melanin. One person in 17,000 in the U.S.A. has some type of albinism. Albinism affects people from all races. Most children with albinism are born to parents who have normal hair and eye color for their ethnic backgrounds. Sometimes people do not recognize that they have albinism. A common myth is that people with albinism have red eyes. In fact there are different types of albinism and the amount of pigment in the eyes varies. Although some individuals with albinism have reddish or violet eyes, most have blue eyes. Some have hazel or brown eyes. However, all forms of albinism are associated with vision problems.
Vision Problems
People with albinism always have problems with vision (not correctable with eyeglasses) and many have low vision. The degree of vision impairment varies with the different types of albinism and many people with albinism are “legally blind,” but most use their vision for many tasks including reading and do not use Braille. Some people with albinism have sufficient vision to drive a car. Vision problems in albinism result from abnormal development of the retina and abnormal patterns of nerve connections between the eye and the brain. It is the presence of these eye problems that defines the diagnosis of albinism. Therefore the main test for albinism is simply an eye examination.
AUTHOR CONTACT:
Brian P. Brooks
National Eye Institute, National Institutes of Health, Bethesda, Maryland, USA.
Phone: 301.451.2238; Fax: 301.402.1214; E-mail: .(JavaScript must be enabled to view this email address).
Types of Albinism
While most people with albinism have very light skin and hair, not all do. Oculocutaneous (pronounced ock-you-low-kew-TAIN-ee-us) albinism (OCA) involves the eyes, hair and skin. Ocular albinism (OA), which is much less common, involves primarily the eyes, while skin and hair may appear similar or slightly lighter than that of other family members.
Over the years, researchers have used various systems for classifying oculocutaneous albinism. In general, these systems contrasted types of albinism having almost no pigmentation with types having slight pigmentation. In less pigmented types of albinism, hair and skin are cream-colored and vision is often in the range of 20/200. In types with slight pigmentation, hair appears more yellow or red-tinged and vision may be better. Early descriptions of albinism called these main categories of albinism “complete” and “incomplete” albinism. Later researchers used a test that involved plucking a hair root and seeing if it would make pigment in a test tube. This test separated “ty-neg” (no pigment) from “ty-pos” (some pigment). Further research showed that this test was inconsistent and added little information to the clinical exam.
Recent research has used analysis of DNA, the chemical that encodes genetic information, to arrive at a more precise classification system for albinism. Four forms of OCA are now recognized – OCA1, OCA2, OCA3 and OCA4; some are further divided into subtypes.
Oculocutaneous albinism type 1 (OCA1 or tyrosinase-related albinism) results from a genetic defect in an enzyme called tyrosinase (hence ‘ty’ above). This enzyme helps the body to change the amino acid tyrosine into pigment. (An amino acid is a “building block” of protein.) There are two subtypes of OCA1. In OCA1A, the enzyme is inactive and no melanin is produced, leading to white hair and very light skin. In OCA1B, the enzyme is minimally active and a small amount of melanin is produced, leading to hair that may darken to blond, yellow/orange or even light brown, as well as slightly more pigment in the skin.
Oculocutaneous albinism type 2 (OCA2 or P gene albinism) results from a genetic defect in the P protein that helps the tyrosinase enzyme to function. Individuals with OCA2 make a minimal amount of melanin pigment and can have hair color ranging from very light blond to brown.
Oculocutaneous albinism type 3 (OCA3) is rarely described and results from a genetic defect in TYRP1, a protein related to tyrosinase. Individuals with OCA3 can have substantial pigment.
Oculocutaneous albinism type 4 (OCA4) results from a genetic defect in the SLC45A2 protein that helps the tyrosinase enzyme to function. Individuals with OCA4 make a minimal amount of melanin pigment similar to persons with OCA2.
Researchers have also identified several other genes that result in albinism with other features. One group of these includes at least eight genes leading to Hermansky-Pudlak Syndrome (HPS). In addition to albinism, HPS is associated with bleeding problems and bruising. Some forms are also associated with lung and bowel disease. HPS is a less common form of albinism but should be suspected if a person with albinism shows unusual bruising or bleeding.
ACCOMPANYING COMMENTARY
TITLE: Informed reasoning: repositioning of nitisinone to treat oculocutaneous albinism
AUTHOR CONTACT:
Seth J. Orlow
New York University School of Medicine, New York, New York, USA.
Phone: 212.263.5245; Fax 212.263.5819; E-mail: .(JavaScript must be enabled to view this email address).
###
Karen Honey
.(JavaScript must be enabled to view this email address)
734-546-5242
Journal of Clinical Investigation