Health Centers > Hypertension Health Center > Hypertension symptoms and signs
Hypertension symptoms and signs
The clinical and laboratory findings are mainly referable to involvement of the target organs: heart, brain, kidneys, eyes, and peripheral arteries.
A. SYMPTOMS
Mild to moderate primary (essential) hypertension is largely asymptomatic for many years. The most frequent symptom, headache, is also very nonspecific. Suboccipital pulsating headaches, occurring early in the morning and subsiding during the day, are said to be characteristic, but any type of headache may occur. Accelerated hypertension is associated with somnolence, confusion, visual disturbances, and nausea and vomiting (hypertensive encephalopathy).
Systemic Hypertension - High Blood Pressure
- Introduction
L Prehypertension - Hypertension Etiology & Classification
L Primary (Essential) Hypertension
L Secondary Hypertension - Complications of Untreated Hypertension
- Hypertension symptoms and signs
- Goals of Hypertension Treatment
- Hypertension Nonpharmacologic Therapy
- Hypertension Drug Therapy
- Developing an Antihypertensive Regimen
- Special Considerations in the Treatment
- Hypertensive Urgencies & Emergencies
L Introduction
L Pharmacologic Management
Hypertension in patients with pheochromocytomas that secrete predominantly norepinephrine is usually sustained but may be episodic. The typical attack lasts from minutes to hours and is associated with headache, anxiety, palpitation, profuse perspiration, pallor, tremor, and nausea and vomiting. Blood pressure is markedly elevated, and angina or acute pulmonary edema may occur. In primary aldosteronism, patients may have muscular weakness, polyuria, and nocturia due to hypokalemia; malignant hypertension is rare. Chronic hypertension often leads to left ventricular hypertrophy, which may be associated with diastolic or, in late stages, systolic dysfunction. Exertional and paroxysmal nocturnal dyspnea may result, and ischemic heart disease is more common (especially when concomitant coronary artery disease is present).
Cerebral involvement causes (1) stroke due to thrombosis or (2) small or large hemorrhage from microaneurysms of small penetrating intracranial arteries. Hypertensive encephalopathy is probably caused by acute capillary congestion and exudation with cerebral edema. The findings are usually reversible if adequate treatment is given promptly. There is no strict correlation of diastolic blood pressure with hypertensive encephalopathy; but it usually exceeds 130 mm Hg.
B. SIGNS
Like symptoms, physical findings depend on the cause of hypertension, its duration and severity, and the degree of effect on target organs.
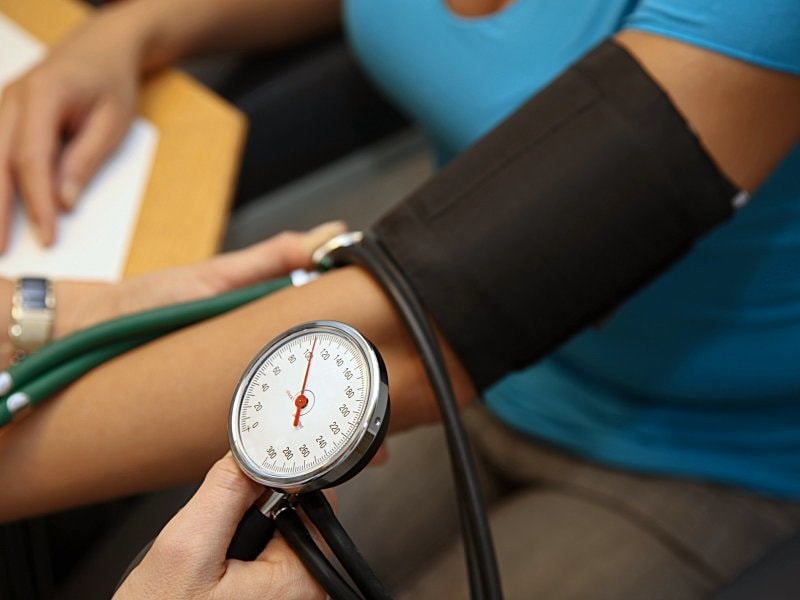
1. Blood pressure - On initial examination, pressure is taken in both arms and, if lower extremity pulses are diminished or delayed, in the legs to exclude coarctation of the aorta. An orthostatic drop is present in pheochromocytoma. Older patients may have falsely elevated readings by sphygmomanometry because of noncompressible vessels. This may be suspected in the presence of Osler's sign - a palpable brachial or radial artery when the cuff is inflated above systolic pressure. Occasionally, it may be necessary to make direct measurements of intra-arterial pressure, especially in patients with apparent severe hypertension who do not tolerate therapy.
2. Retinas - Narrowing of arterial diameter to less than 50% of venous diameter, copper or silver wire appearance, exudates, hemorrhages, or papilledema are associated with a worse prognosis.
3. Heart and arteries - Left ventricular enlargement with a left ventricular heave indicates severe or long-standing hypertrophy. Older patients frequently have systolic ejection murmurs resulting from calcific aortic sclerosis, and these may evolve to significant aortic stenosis in some individuals. Aortic insufficiency may be auscultated in up to 5% of patients, and hemodynamically insignificant aortic insufficiency can be detected by Doppler echocardiography in 10-20%. A presystolic (S4) gallop due to decreased compliance of the left ventricle is quite common in patients with sinus rhythm.
4. Pulses - The timing of upper and lower extremity pulses should be compared to exclude coarctation of the aorta. All major peripheral pulses should be evaluated to exclude aortic dissection and peripheral atherosclerosis, which may be associated with renal artery involvement.
C. LABORATORY FINDINGS
Recommended testing includes the following: hemoglobin; urinalysis and renal function studies, to detect hematuria, proteinuria, and casts, signifying primary renal disease or nephrosclerosis; fasting blood sugar level, since hyperglycemia is noted in diabetes and pheochromocytoma; plasma lipids, as an indicator of atherosclerosis risk and an additional target for therapy; serum uric acid which, if elevated, is a relative contraindication to diuretic therapy; and basal electrolytes. Measurement of the plasma aldosterone/renin ratio is indicated to screen for mineralocorticoid excess in hypertensive patients with hypokalemic alkalosis (even if they are taking diuretics), resistant hypertension, or an adrenal "incidentaloma."
D. ELECTROCARDIOGRAPHY AND CHEST RADIOGRAPHS
Electrocardiographic criteria are highly specific but not very sensitive for left ventricular hypertrophy. The "strain" pattern of ST-T wave changes is a sign of more advanced disease and is associated with a poor prognosis. A chest radiograph is not necessary in the workup for uncomplicated hypertension since it usually does not yield additional information.
E. ECHOCARDIOGRAPHY
Although echocardiography has been advocated to determine the need for drug therapy in patients with borderline or mildly elevated pressures, it is unusual to find left ventricular mass readings above the upper 75% confidence limits in the absence of systolic hypertension. The primary role of echocardiography should be to evaluate patients with clinical symptoms or signs of cardiac disease.
F. DIAGNOSTIC STUDIES
Additional diagnostic studies are indicated only if the clinical presentation or routine tests suggest secondary or complicated hypertension. These may include tests such as 24-hour urine free cortisol, plasma metanephrine and the plasma aldosterone/renin ratio for endocrine causes of hypertension, renal ultrasound to diagnose primary renal disease (polycystic kidneys, obstructive uropathy), and testing for renal artery stenosis. Further evaluation may include abdominal imaging studies (ultrasound, CT scan, or MRI) or renal arteriography.
G. SUMMARY
Since most hypertension is "primary," few studies are necessary beyond those listed above. If conventional therapy is unsuccessful or if symptoms suggest a secondary cause, further studies are indicated.