Risk Factors for Hypoglycemia
The conventional risk factors for iatrogenic hypoglycemia (5,6,22) are based on the premise that absolute or relative insulin excess is the sole determinant of risk (Table 4). Absolute or relative insulin excess occurs when:
TABLE 4 Risk Factors for Iatrogenic Hypoglycemia
Absolute or relative insulin excess
1. Insulin, or insulin secretagogue dose excessive, ill-timed, or of the wrong type
2. Decreased exogenous glucose delivery Missed meals or snacks, overnight fast
3. Decreased endogenous glucose production Alcohol
4. Increased glucose utilization Exercise
5. Increased sensitivity to insulin
- Insulin sensitizer
- Weight loss
- Late after exercise
- Improved fitness
- Middle of the night
- Glycemic control
6. Decreased insulin clearance
- Renal failure
Compromised glucose counterregulation
1. Insulin deficiency
2. History of severe hypoglycemia, hypoglycemia unawareness, or both
3. Aggressive glycemic therapy per se
- Lower HbAlc
- Lower glycemic goals
- Insulin or insulin secretagogue doses are excessive, ill-timed or of the wrong type.
- Exogenous glucose delivery is decreased, as following missed meals or snacks, or during an overnight fast.
- Endogenous glucose production is decreased, as following alcohol ingestion.
- Glucose utilization is increased, as during exercise.
- Sensitivity to insulin is increased, as during treatment with an insulin sensitizer, late after exercise, in the middle of the night, or following weight loss, increased fitness or improved glycemic control.
- Insulin clearance is decreased, as in renal failure.
However, while they must be considered carefully, these conventional risk factors explain only a minority of episodes of severe iatrogenic hypoglycemia, at least in type 1 diabetes (23).
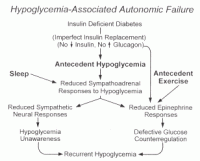
FIGURE 2 Schematic diagram of the concept of hypoglycemia-associated autonomic failure, and the pathogenesis of the syndromes of defective glucose counterregulation and hypoglycemia unawareness, in type 1 diabetes (and in advanced type 2 diabetes). As discussed earlier, iatrogenic hypoglycemia is the result of the interplay of absolute or relative insulin excess and compromised physiological and behavioral defenses against falling plasma glucose concentrations. Risk factors related to compromised defenses (Table 4) include:
- Insulin deficiency.
- A history of severe hypoglycemia, hypoglycemia unawareness, or both.
- Aggressive glycemic therapy per se, as evidenced by lower HbA1C levels, glycemic goals, or both.
These are clinical surrogates of HAAF (5,6). Insulin deficiency indicates that insulin levels will not decrease, and predicts accurately that glucagon levels will not increase, as glucose levels fall.
A history of severe hypoglycemia indicates, and hypoglycemia unawareness or even aggressive glycemic therapy per se implies, recent antecedent hypoglycemia which attenuates sympathoadrenal epinephrine and neurogenic symptom responses to falling glucose levels by shifting the glycemic thresholds for these responses to lower plasma glucose concentrations. Thus, these risk factors are indicative of defective glucose counterregulation and hypoglycemia unawareness, the components of HAAF.
Philip E. Cryer
Washington University School of Medicine, St. Louis, Missouri, U.S.A.
REFERENCES