Vulnerability, Stress, and Psychiatric Diatheses: A Hypothetical Model
Figure 21 depicts an integrative schema that conceptualizes the interplay of extrinsic and intrinsic factors with the schizophrenia diathesis. The basis for this formulation is the familiar stress-diathesis model of schizophrenia (Nuechterlein and Dawson 1984; Zubin and Spring 1977), supported by more recent understanding of the neuropsychological underpinnings of the pathophysiology of schizophrenia (Weinberger 1987).
In Figure 21, the vertical axis represents vulnerability to psychotic symptoms of the schizophrenic type and the horizontal axis depicts the proportion of the general population. At the far left, a tiny fraction of the population manifests a very high vulnerability to psychosis, with an everdecreasing loading for such risk moving to the right along the curve.
Only a fraction of 1% of the population express a vulnerability so great that a schizophrenic psychosis will emerge under virtually any level of life stress, no matter how minor.
However, several percent of the population have a meaningful but lesser degree of vulnerability, such that the schizophrenic psychosis will become manifest if a great enough stress is encountered to “push the patient over the brink.” This stress can come from any of a variety of sources and can be biological, psychological, or social.
Depression in Schizophrenia
- Depression in the Course of Schizophrenia
- Differential Diagnosis of Depression in the Course of Schizophrenia
- - Medical/Organic Factors
- - Negative Symptoms of Schizophrenia
- - Neuroleptic-Induced Dysphoria
- - Neuroleptic-Induced Akinesia
- - Neuroleptic-Induced Akathisia
- - Disappointment Reactions
- - Prodrome of Psychotic Relapse
- - Schizoaffective Depression
- - Depression as the Expression of a Biological Diathesis
- Incidence and Prevalence of Depression
- Treatment Strategies
- Vulnerability, Stress, and Psychiatric Diatheses
The model depicted fits much of what we know about schizophrenia and what can influence its expression. If the fundamental vulnerability is genetic, additional biopsychosocial stressors might be poor maternal nutrition (associated with poverty), intrauterine viral infection, injuries during a difficult delivery, inadequate childhood nutrition, lack of normal childhood stimulation, lack of opportunity to learn protective interpersonal and coping skills, developmental experiences promoting intrapsychic conflicts, extreme psychic stress in adolescence/early adulthood (e.g., high “expressed emotion,” poverty, trauma, chaotic environments), and the biological, psychological, and social insults that may be associated with substance use and abuse.
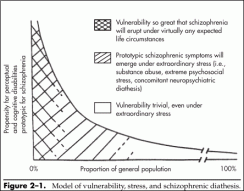 Figure 21. Model of vulnerability, stress, and schizophrenic diathesis.
Figure 21. Model of vulnerability, stress, and schizophrenic diathesis.
Integrative schema conceptualizing the interplay of extrinsic and intrinsic factors with the schizophrenic diathesis. Source. Reprinted with permission from Siris SG, Lavin MR: “Schizoaffective Disorder, Schizophreniform Disorder and Acute Psychotic Disorder (Including Brief Reactive Psychosis),” in Comprehensive Textbook of Psychiatry/VI, 6th Edition. Edited by Kaplan HI, Sadock BJ. Philadelphia, PA, Williams & Wilkins, 1995, pp. 1019 1031 (p.
1021). Copyright 1995, Williams & Wilkins.
Once the patient is “pushed over the brink” into psychosis, of course, the full physiological and biopsychosocial cascade of events is unleashed, representing the multivariate clinical course of schizophrenia.
A novel integrative model posits that the diathesis for an independent psychiatric disorder may represent the stressor that can tip a person with an intermediate vulnerability over into the path of psychotic deterioration (Siris 1988; Siris and Lavin 1995). Thus, a person who has a diathesis for a major depressive disorder accompanying his or her intermediate diathesis for schizophrenia could be tipped over by the stress of the affective disorder into a schizophrenic psychosis.
Certainly, a person with depression is sorely stressed psychologically. It is not unreasonable to speculate that such a person is stressed biologically and socially as well.