Vulnerability, Stress, and Psychiatric Diatheses: A Hypothetical Model
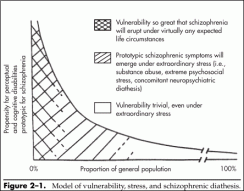
Since, as depicted in Figure 21, there are many more people with intermediate vulnerabilities to the schizophrenic psychosis than with extreme vulnerability, the chances of a psychosis being triggered by another concurrent psychiatric diathesis can be considerable. For example, if this proposed model were the basis for so-called schizoaffective disorder, it could account for schizoaffective disorder being roughly as prevalent as schizophrenia in the general population (Siris and Lavin 1995).
This model, of course, also opens the possibility that other concurrent psychiatric diatheses, such as those for panic disorder or obsessive-compulsive disorder, could interact with an intermediate vulnerability for psychosis in a similar manner. Several of the issues discussed earlier are consistent with this model involving depression in schizophrenia. One is the observation that depressive-like symptoms are a common component of the psychotic prodrome (Docherty et al. 1978; Green et al. 1990; Herz 1985; Herz and Melville 1980; Hirsch et al. 1989; Johnson 1988; Tollefson et al. 1999).
Dysphoria also has been found to be more strongly associated with positive symptoms in schizophrenia than with negative symptoms (Norman and Malla 1994). However, since simple dysthymia is not overrepresented in patients with schizophrenia the way depression is (Bland et al. 1987), the role of depression in schizophrenia cannot readily be accounted for as a mere psychological reaction to the unfolding of unpleasant events.
Depression in Schizophrenia
- Depression in the Course of Schizophrenia
- Differential Diagnosis of Depression in the Course of Schizophrenia
- - Medical/Organic Factors
- - Negative Symptoms of Schizophrenia
- - Neuroleptic-Induced Dysphoria
- - Neuroleptic-Induced Akinesia
- - Neuroleptic-Induced Akathisia
- - Disappointment Reactions
- - Prodrome of Psychotic Relapse
- - Schizoaffective Depression
- - Depression as the Expression of a Biological Diathesis
- Incidence and Prevalence of Depression
- Treatment Strategies
- Vulnerability, Stress, and Psychiatric Diatheses
Also relevant is the finding that maintenance adjunctive antidepressant treatment in responding postpsychotic depressed patients protected them not only from relapses into depression but from psychotic exacerbations as well (Siris et al. 1994). Although the model proposed here is by no means proven, it is rich in testable hypotheses and possibly could account for a portion of the heterogeneity well known to be a component of the disorder we refer to as schizophrenia.
 Additionally, and importantly, it is a model with implications for treatment, to relieve suffering and promote functioning among a substantial number of patients afflicted with symptoms of both schizophrenia and depression. In summary, it is well described that a depressive syndrome often occurs in the course of schizophrenia.
Additionally, and importantly, it is a model with implications for treatment, to relieve suffering and promote functioning among a substantial number of patients afflicted with symptoms of both schizophrenia and depression. In summary, it is well described that a depressive syndrome often occurs in the course of schizophrenia.
However, this syndrome is not homogeneous. Rather, there is a broad differential diagnosis that is crucial both for our understanding of its etiology in any specific case and for our arriving at a rational approach to its treatment.
Moreover, the occurrence of a depressive syndrome in the course of schizophrenia raises theoretical issues relevant to the interplay of psychosis with both situational events and affective diatheses in psychiatry.
These are issues that cut to the very core of our understanding of the disorder we know as schizophrenia, suggesting novel approaches to the organization of its heterogeneity as well as testable hypotheses concerning a variety of therapeutic interventions.
Samuel G. Siris, M.D.
References
- Addington D, Addington J, Patten S: Gender and affect in schizophrenia. Can J Psychiatry 41:265-268, 1996
- American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders. Washington, DC, American Psychiatric Association, 1994
- Andreasen NC, Olsen S: Negative vs positive schizophrenia: definition and validation. Arch Gen Psychiatry 39:789-794, 1982
- Atre-Vaidya N, Taylor MA: Effectiveness of lithium in schizophrenia: do we really have an answer? J Clin Psychiatry 50:170-173, 1989
- Bandelow B, Muller P, Gaebel WE: Depressive syndromes in schizophrenic patients after discharge from hospital. Eur Arch Psychiatry Clin Neurosci 240:113-120, 1991
- Barnes TR, Curson DA, Liddle PF, et al: The nature and prevalence of depression in chronic schizophrenic in-patients. Br J Psychiatry 154:486-491, 1989
- Bartels SJ, Drake RE: Depressive symptoms in schizophrenia: comprehensive differential diagnosis. Compr Psychiatry 29:467-483, 1988
- Bartels ..... full References ... »