Varicocele
Varicocele Overview
Non-surgical Treatment for Male Infertility
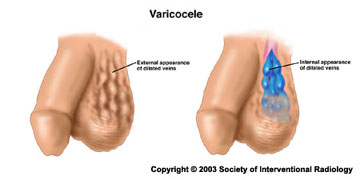
A varicocele is a varicose vein of the testicle and scrotum that may cause pain, testicular atrophy (shrinkage) or fertility problems. Veins contain one-way valves that work to allow blood to flow from the testicles and scrotum back to the heart. When these valves fail, the blood pools and enlarges the veins around the testicle in the scrotum to cause a varicocele. Open surgical ligation, performed by a urologist, is the most common treatment for symptomatic varicoceles. Varicocele embolization, a non-surgical treatment performed by an interventional radiologist, is a highly effective, widely available technique to treat symptomatic varicoceles that is greatly underutilized in this country.
Prevalence
- Approximately 10 percent of all men have varicoceles - among infertile couples, the incidence of varicoceles increases to 30 percent
- Highest occurrence in men aged 15-35
- As many as 70-80,000 men in America may undergo surgical correction of varicocele annually
Symptoms
Pain - aching pain when an individual has been standing or sitting for long periods of time and pressure builds up on the affected veins. Typically, painful varicoceles are prominent in size.
Fertility Problems - There is an association between varicoceles and infertility. The incidence of varicocele increases to 30 percent in infertile couples. Decreased sperm count, decreased motility of sperm, and an increase in the number of deformed sperm are related to varicoceles. Some experts believe that blocked and enlarged veins around the testes, called varicoceles, cause infertility by raising the temperature in the scrotum and decreasing sperm production.
Testicular Atrophy - Shrinking of the testicles is another sign of varicoceles. Often, once the testicle is repaired it will return to normal size.
Varicocele Diagnosis
Diagnosis is fairly simple through either physical or diagnostic examination.
- Typical on left side of scrotum
- Physical exam - visible - scrotum looks like a “bag of worms”
- Testicle can shrink in size / atrophy
- When varicoceles are not clearly present, the abnormal blood flow can often be detected with a noninvasive imaging exam called color flow ultrasound or through a venogram-an X-ray in which a special dye is injected into the veins to “highlight” blood vessel abnormalities
Varicocele Treatments
Currently there are two treatment options for men with varicoceles: Catheter-directed embolization or surgical ligation
Catheter-directed Embolization
Catheter directed embolization is a non-surgical, outpatient treatment performed by an interventional radiologist using imaging to guide catheters or other instruments inside the body. Through mild IV sedation and local anesthesia, patients are relaxed and pain-free during the approximately two-hour procedure.
For the procedure, an interventional radiologist makes a tiny nick in the skin at the groin using local anesthesia, through which a thin catheter (much like a piece of spaghetti) is passed into the femoral vein, directly to the testicular vein. The physician then injects contrast dye to provide direct visualization of the veins so s/he can map out exactly where the problem is and where to embolize, or block, the vein. By using coils, balloons, or particles, the interventional radiologist blocks the blood flow in the vein which reduces pressure on the varicocele. By embolizing the vein, blood flow is re-directed to other healthy pathways. Essentially, the incompetent vein is “shut off” internally by preventing blood flow, accomplishing what the urologist does, but without surgery.
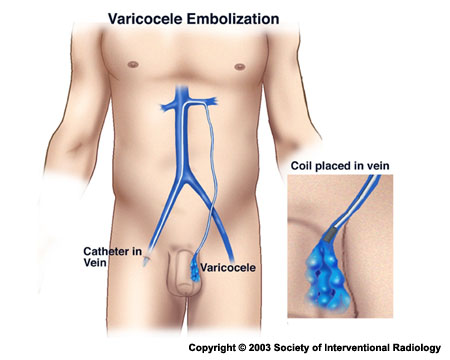
Surgical Ligation
Usually, outpatient surgery is performed under general anesthesia. During this treatment, the surgeon makes an incision above the scrotum and cuts through the layers of tissue to expose the faulty veins. The affected veins are tied off, ligated, to redirect the blood flow into normal veins. A laparoscope is sometimes used to perform the procedure. Recovery usually takes up to six weeks before heavy lifting and other strenuous activities can be performed.
Efficacy
Clinical resolution of pain and swelling and restoration of blood flow in the vein is greater than 85 percent with the catheter-directed technique.
Revision date: July 4, 2011
Last revised: by David A. Scott, M.D.