Peripheral Arterial Disease Clinical Presentation and Diagnosis
Clinical Assessment
PAD is associated with two very characteristic types of limb symptoms, intermittent claudication and ischemic rest pain. Claudication is derived from the Latin word meaning to limp, which is the type of gait observed when a patient with PAD develops symptoms of claudication. The discomfort most commonly involves the calf or buttocks during walking exercise and is resolved within 10 min of rest. These patients commonly can walk no more than two to three blocks (200-300 m) before they must stop to relieve the claudication pain. Peak exercise capacity is reduced 50% compared to healthy elderly subjects, and there is a profound limitation in daily activities.
Patients with chronic critical limb ischemia often present with rest pain in the distal foot that occurs at night and is relieved with dependency. Patients with more severe disease develop ischemic ulcers that are usually found at the distal points of the foot (toes, etc.) and are painful. In general, any patient with an open foot wound needs to have adequate arterial circulation confirmed by vascular studies.
The differential diagnosis in patients with leg symptoms includes PAD, diabetic sensory neuropathy, reflex sympathetic dystrophy, vasculitis, spinal stenosis, and arthritis. Patients with diabetic neuropathy may present with normal pedal pulses, but symptoms consistent with ischemic pain, and nonhealing neuropathic ulcers (these ulcers are usually on the plantar surface of the foot at pressure points—metatarsal heads). Reflex sympathetic dystrophy may present after surgical or other forms of trauma and leads to a painful, discolored, swollen extremity. Although this disorder is most likely caused by an autonomic neuropathy, arterial perfusion is typically normal. Patients with vasculitis may present with Buerger’s disease (thromboangitis obliterans) and a strong smoking history. Claudication-like symptoms may also arise from spinal stenosis, which is due to osteophytic narrowing of the lumbar neurospinal canal. These symptoms include numbness and weakness in the lower extremity that is produced by standing or increasing lumbar lordosis rather than just ambulation. The symptoms are relieved not simply by rest, but also by sitting down or leaning forward to straighten out the lumbar spine. Patients with arthritis of the knee or hip may also have not only pain in the joint with ambulation, but also pain at rest or with weightbearing.
Hemodynamic Assessment
An ankle-brachial index (ABI) should be performed in patients suspected of having PAD, which would include persons at risk who are over the age of 70 years or younger patients between the age of 50 to 69 years who smoke or have diabetes. The estimated prevalence of PAD in this population at risk is more than 25%. In addition, patients with exertional leg symptoms should also be evaluated with an ABI. The ABI test can be performed in the office setting using a routine sphygmomanometer and a handheld, continuous-wave Doppler to determine the systolic blood pressure in the arms and posterior tibial and dorsalis pedis arteries of each ankle. The ABI calculation is based on the higher of the two arm pressures and the higher pressure of the two vessels in each ankle. There is not a single cutoff value to define an abnormal ABI, but a ratio of 0.90 or less should be considered diagnostic for PAD. ABI values of 0.40 or less are consistent with critical leg ischemia. In addition to obtaining the ABI, occlusive lesions can be further localized by taking pressure measurements in the upper and lower thigh and calf (segmental limb pressures). In patients with iliac occlusive disease, the thigh pressures are reduced, whereas patients with disease more distal in the leg may have a normal thigh pressure but reduced calf and ankle pressures.
Functional Assessment
Patients with claudication have a severe limitation in exercise performance and walking ability. Thus, determining functional status is an important aspect of the overall evaluation of the patient with PAD. In patients with claudication, treadmill testing can be used to define the distance at which claudication pain begins (initial claudication distance) and the maximal walking distance. Claudication therapies typically increase both the initial and maximal walking distances.
In addition to treadmill testing, several questionnaire measures of functional status have been developed and validated in this patient population. The walking impairment questionnaire (WIQ) is a disease-specific instrument that asks a series of questions regarding the patient’s claudication severity and ability to walk defined distances, speeds, and stairs. This questionnaire is simple to administer and has been shown to predict the response to claudication therapies. The Medical Outcomes Short Form-36 instrument is a nondisease-specific questionnaire that assesses a variety of functional status domains. This questionnaire has also been sensitive in detecting treatment effect, particularly in the physical functioning realm.
Figure 41.1 provides an approach to the diagnosis of PAD in elderly populations.
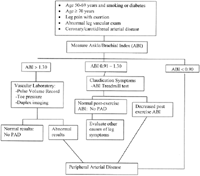
Figure 41.1. Evaluation of patients suspected to have periph-eral arterial disease (PAD). Patients should be evaluated for Peripheral arterial disease if they if they are at increased risk because of their age or presence of atherosclerotic risk factors, have leg symptoms on exertion, or have distal limb ulceration for which history and examination do not provide an obvious explanation. Additional vascular studies can be obtained in patients with an ankle-brachial index (ABI) above 1.30, including pulse volume recordings (PVR), and pressure in the first toe, or by duplex imaging of the peripheral vessels to determine if Peripheral arterial disease is present. Patients with leg symptoms on exertion who have an ankle-brachial index of 0.91 to 1.30 should be considered for an exercise test. An ankle-brachial index that is above 0.90 at rest but decreases by 20% after exercise is diagnostic of Peripheral arterial disease.96 If the initial ankle-brachial index is 0.90 or less at rest, then the patient likely has Peripheral arterial disease and no additional tests are necessary.