Pharmacotherapy - Schizophrenia in African Americans
Although psychosocial support is important in managing schizophrenia, pharmacotherapy remains essential for maintenance and recovery. Unfortunately, the treatment of ethnic minorities is often inappropriate. African Americans often receive excessive doses of medication, whereas Hispanics and Asians receive lower medication doses, when treated by ethnic providers. Moreover African Americans are more likely to receive first-generation rather than second-generation or atypical medications, higher doses of medication, and more depot medication. Table 60.2 summarizes findings about the medicating of African Americans. Please note that some of the studies involved Medicaid or Veterans Administration hospital patients, and income presumably should not have affected the difference.
Also note that some of the typical agents and high doses may have been a consequence of the use of depot medication, for which only one atypical agent is now available, and no atypical form was available at the time of many of the studies. Yet when the use of depot medication was controlled, the high dosing of typical medication persisted.
The biological evidence, if anything, supports lower dosing for ethnic minorities.
Ethnic differences have been found in the way many psychotropic agents are metabolized through the cytochrome P450 family of liver isoenzymes. The CYP450 2D6 isoenzyme in particular shows ethnic variation. Relative to the majority of European Americans, Asians, Hispanics, and African Americans show reduced activity in this enzyme, whereas many Ethiopians show increased activity. Reduced activity means that a drug is metabolized more slowly, therefore having higher plasma levels. Individuals with CYP450 2D6 alleles associated with reduced or no activity who are given standard medication doses are more likely to have extrapyramidal side effects on antipsychotics and to discontinue treatment, whereas those with increased activity may not show any response at all. Thus, there is no biological reason for the excessive dosing of African Americans.
Pharmacological studies provide some support for prescribing atypical antipsychotics to African Amerians. Second-generation, or atypical antipsychotics, are less likely to cause extrapyramidal side effects and are believed to cause less tardive dyskinesia.
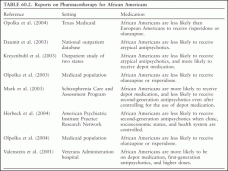 TABLE 60.2. Reports on Pharmacotherapy for African Americans
TABLE 60.2. Reports on Pharmacotherapy for African Americans
Moreover, some of the newer antipsychotic agents are not predominately metabolized through the CYP450 2D6 system and are instead metabolized through CYP450 1A2, with CYP450 2D6 as a minor pathway. Asians and Hispanics are more likely than European Americans to experience movement disorder side effects, such as acute dystonic reactions, when given typical or first-generation antipsychotics. African Americans are twice as likely as European Americans to develop tardive dyskinesia on typical antipsychotics. African Americans are also more likely than European Americans to experience acute extrapyramidal symptoms with typical antipsychotics, but these differences disappear with atypical agents.
For ethnic minorities, especially African Americans, the atypical antipsychotics appear to offer a decided advantage when movement disorder side effects are considered.
However some of the atypical agents have been associated with unacceptable metabolic consequences, such as diabetes and metabolic syndrome. These disorders are more common in African Americans and Latinos. The Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE), a naturalistic federally funded study that compared the atypical agents to each other and to a typical agent, showed that the atypical agents did not provide a great advantage. The CATIE study had 40% African American participation, so insufficient numbers of minorities cannot be used as an argument against it. Nevertheless, the study excluded those with tardive dyskinesia, limited the dosing range, and involved a limited time period. Regarding ethnic minorities, although better than most studies, CATIE must be considered in the context of differing ethnic needs.
The atypical agent clozapine has consistently shown superior efficacy and fewer movement disorder side effects compared to other antipsychotics. Like other atypical antipsychotics, it is also less available to African Americans, but for different reasons. Its side effects include the metabolic side effects seen in atypical agents, but this is not the limiting factor. The difficulty is its greater risk for agranulocytosis, which requires regular blood monitoring. Before taking clozapine, minimal leukocyte counts are recommended despite the lack of evidence that preexisting white counts predict agranulocytosis. However, African Americans are known to have normal leukocyte counts whose range may extend well below listed normal values (i.e., a “benign leukopenia”). As a result, the overly cautious clinician may choose not to start otherwise healthy African American patients on clozapine.
Since pharmacological factors do not explain the differing prescribing patterns seen with African Americans, what does? As noted earlier, provider attitudes and eithic minorities’ perceptions of the mental health system are extremely important. The view that African Americans are more hostile than they actually are may be confounded by poor communications and social, economic, and ethnic distance. Patients who become suspicious and hostile to the system either choose other alternatives or are less compliant, as shown by the high rate of noncompliance. The solution appears to be straightforward. African Americans must be made to feel welcome in the mental health system. When physicians are more willing to consider patients’ ethnic differences, excessive dosing disappears.
To summarize, ethnic minorities receive older antipsychotics. African Americans receive higher doses and more depot medication, probably due more to attitudinal factors than to socioeconomic or biological factors. These treatment differences ignore biological differences that may require lower doses and a greater concern for movement disorder side effects. The prudent clinician should individualize treatment. The patient should be considered a partner in developing a reasonable dosing plan. Culture, ethnicity, and the patient’s individual risk profile must be considered. Family history and family members must be consulted. As much as possible, rapport should be established regardless of ethnicity.
CONCLUSION
Schizophrenia is a devastating disorder for anyone, but especially for ethnic minorities. Limited access to treatment increases illness burden for economically depressed families.
When treatment is available, misdiagnosis is common; other disorders, mislabeled as schizophrenia, are treated inappropriately. Genetic factors are important in schizophrenia, as is the family environment. Consideration of cultural factors means that findings about family environment in European American families do not apply to ethnic minorities. Suboptimal treatment of African Americans with schizophrenia is not simply a consequence of socioeconomic factors. Excessive dosing with older medications is common and cannot be accounted for by biological factors. The physician–patient relationship, willingness of the physician to engage the patient, and individualized treatment are crucial to optimal pharmacotherapy. Race and ethnicity, their cultural determinants, and their interaction with socioeconomic and biological factors must be considered in the diagnosis and treatment of schizophrenia.
- Overdiagnosis of schizophrenia is common among African Americans, with affective disorders often misdiagnosed as schizophrenia, mainly due to a failure to get adequate information, clinician bias, and cultural factors.
- For a proper diagnosis of schizophrenia in African Americans and other ethnic groups, all sources of information should be considered, including adherence to DSM-IV criteria, and taking cultural issues into account.
- Several studies have shown putative gene associations for schizophrenia in African Americans (e.g., polymorphisms of the synapsin III and NOTCH 4 genes); however, genes should only be considered in the context of environmental factors.
- Despite limited resources, African American families are more likely than European American families to become caregivers for family members with schizophrenia.
- High emotionality and family intrusiveness have been shown to predict poor outcome in European Americans with schizophrenia, but not in their African American counterparts.
- African Americans have less access to health care (even after income is controlled), a greater rate of involuntary hospitalizations, and lower use of preferential treatments, such as day treatment or case management, than European Americans.
- African American patients are more likely to receive first-generation antipsychotics, higher doses of medications, and more depot medication than European Americans, whereas Hispanics and Asians receive lower dosages.
- African Americans, Asians, and Hispanics show reduced activity of the cytochrome P450 isoenzyme CYP450 2D6 compared to a majority of European Americans; this suggests higher plasma levels of the antipsychotic drugs, and thereby a need for lower dosages in the ethnic minority groups.
- Asians and Hispanics are more likely to develop antipsychotic-induced movement disorders such as acute dystonia, whereas African Americans have a greater risk of developing tardive dyskinesia with first-generation antipsychotics than do European Americans.
- To reduce mental health care disparity, African Americans (as well as other ethnic minority groups) should be made to feel welcome in the mental health system; treatment should be individualized, and cultural factors should be considered.
###
William B. Lawson
Clinical handbook of schizophrenia / edited by Kim T. Mueser, Dilip V. Jeste.
REFERENCES
- Barnes, A. (2004). Race, schizophrenia, and admission to state psychiatric hospitals. Administration and Policy in Mental Health, 31, 241–252.
- Blow, F. C., Zeber, J. E., McCarthy, J. F., Valenstein, M., Gillon, L., & Bingham, C. R. (2004). Ethnicity and diagnostic patterns in veterans with psychoses. Social Psychiatry and Psychiatric Epidemiology, 39, 841–851.
- Daumit, G. L., Crum, R. M., Guallar, E., Powe, N. R., Primm, A. B., Steinwachs, D. M., et al. (2003). Outpatient prescriptions for atypical antipsychotics for African Americans, Hispanics, and whites in the United States. Archives of General Psychiatry, 60, 121–128.
- DelBello, M. P., Lopez-Larson, M. P., Soutullo, C. A., & Strakowski, S. M. (2001). Effects of race on psychiatric diagnosis of hospitalized adolescents: A retrospective chart review. Journal of Child and Adolescent Psychopharmacology, 11(1), 95–103.
- Herbeck, D. M., West, J. C., Ruditis, I., Duffy, F. F., Fitek, D. J., Bell, C. C., et al. (2004). Variations in use of second-generation antipsychotic medication by race among adult psychiatric patients Psychiatric Services, 55(6), 677–684.