Schizophrenia in African Americans
Schizophrenia is considered the most severe psychiatric disorder. It has a poor prognosis, an unknown etiology, and an age of onset in the late teens and early 20s, when many individuals finish their education and begin their careers. Current treatments are mostly palliative, with uncertain recovery and rarely substantiated cures. Individuals and their families often face a lifetime of illness that is associated with individual and societal morbidity, shortened lifespan, and high suicide rates. Recent advances have led to improved diagnostic accuracy, a better understanding of genetic risks and psychosocial stressors, and improved treatment that has made recovery an attainable goal. This chapter indicates that race and ethnicity impact the diagnosis, course, and treatment of this illness through biopsychosocial factors that are only beginning to be appreciated. The focus is on African Americans, for whom there is a more extensive literature than for other ethnic minorities.
Epidemiology
African Americans have always been viewed as being overdiagnosed with schizophrenia.
Even recent clinical reports show that African Americans are at as much as a tenfold increased risk over other ethnic minorities despite improved diagnostic accuracy and widespread use of the DSM-III and DSM-IV. Lawson, Hepler, Holladay, and Cuffel (1994) reported that African Americans in both inpatient and outpatient settings were diagnosed with schizophrenia at higher percentage rates than African Americans in the overall population.
Rates of mood disorder for African Americans, and both schizophrenia and affective disorders for European Americans were the same as rates in the general population. Strakowski and colleagues (2003) reported higher rates of schizophrenia for African Americans in inpatient and outpatient settings. The higher rates were often associated with correspondingly lower rates of affective disorders.
The findings have generally been assumed to reflect affective disorders misdiagnosed as schizophrenia. These differences often disappeared with the use of structured interviews, which presumably minimize bias. Large-scale, door-to-door epidemiological surveys have tended to support this interpretation as well. The Epidemiologic Catchment Area study, which sampled five major cities and oversampled ethnic minorities, found no difference between African Americans and other ethnic groups when socioeconomic class was controlled. The National Cormobidity Survey and the more recent National Comorbidity Survey Replication found that African Americans were less likely to have nonaffective psychosis, which is primarily schizophrenia.
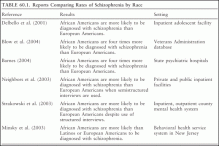 TABLE 60.1. Reports Comparing Rates of Schizophrenia by Race
TABLE 60.1. Reports Comparing Rates of Schizophrenia by Race
Nevertheless, recent clinical studies continue to report an overdiagnosis of schizophrenia in African Americans despite controls for a variety of settings. Table 60.1 summarizes reports comparing rates of schizophrenia by race. These findings show that the overdiagnosis occurs in juvenile facilities, in the Veterans Administration, and in public and private facilities. The overdiagnosis occurs despite the use of structured interview instruments. The development of DSM-III has certainly improved validity and diagnosis of psychiatric disorders. However, consistent use of DSM-III and now DSM-IV often does not prevent the misdiagnosing of African Americans. Strakowski and colleagues (2003) showed that the misdiagnosis was not the consequence of the misapplication of diagnostic criteria (i.e., variance in criteria). Rather, information variance (failure to obtain adequate information) was more of a factor. In addition, African Americans with affective disorders are more likely to have prominent first-rank psychotic symptoms than European Americans, which uninformed clinicians often interpret as evidence for schizophrenia, while overlooking affective symptoms. Other factors include clinician bias based on preconceived notions about the presence of affective disorders in African Americans, lack of familiarity with culture-based idioms of distress, and social distance.
Patient factors may also be involved. The increased likelihood of diagnosing psychotic symptoms in African Americans may be a result of misinterpretation of other intrapsychic experiences. African Americans without schizophrenia are more likely to report dissociative symptoms. Paranoia, which is often reported, is frequently seen on older versions of the Minnesota Multiphasic Personality Inventory (MMPI). A cultural reticence to disclose inner feelings to strangers of a different ethnicity is often reported and has been referred to as a “healthy paranoia.” African Americans often delay or do not seek mental health treatment until symptoms are severe, thereby making diagnosis difficult. Clearly, the diagnosis of schizophrenia in African Americans should be made only after other, alternative diagnoses are considered.
In summary, in diagnosing African Americans and other ethnic groups as well, all sources of information should be included. Family members, caretakers, and past medical records should be consulted. Premature closure should be avoided when a patient presents with psychotic symptoms. It is important to remember that hallucinations may occur in affective and anxiety disorders, especially when treatment has been delayed. Close adherence to DSM-IV criteria should be encouraged, with the recognition that DSM-IV does not exclude mood or anxiety disorders when psychotic symptoms are present. Certainly awareness of cultural issues, such as specific idioms of distress, should be recognized. It is difficult to know the nuances of every culture, which is why sources other then the patient must be consulted. Whatever the case, the diagnosis of schizophrenia should be presumptive for African Americans only when other diagnoses are excluded.
Genetic Factors
Throughout much of the 20th century, schizophrenia was thought to be the result of family pathology. A diathesis–stress model is now prevalent. Schizophrenia clearly has a genetic risk, since a heavy loading of biological relatives increases the risk.
Several studies have reported putative gene associations for African Americans when findings in other ethnic groups have been negative. Polymorphisms of the synapsin III and NOTCH 4 genes were associated with schizophrenia in African Americans but not European Americans. One possibility is that schizophrenia may have a different genetic etiology in African Americans. A more likely explanation is that individuals of African ancestry have older genetic variations, since they have ancestry genes and greater haplotype diversity. As a result, genetic differences that may exist are easily identified.
The Caspi Study reminded us that for psychiatric disorders, genes should only be considered in the context of environmental factors. In that study, major depression was associated with the number of lifetime episodes of childhood abuse, but only in the presence of a certain allele of the serotonin receptor. Family members often ask about their risk for schizophrenia. A simple statement of known risk could be misinterpreted. It is also important to inform families that ethnicity probably does not increase risk, and that family environment does not cause schizophrenia. Nevertheless, risk is not conferred by genetic factors alone. Environment, in a broad sense, is also important.
###
William B. Lawson
Clinical handbook of schizophrenia / edited by Kim T. Mueser, Dilip V. Jeste.
REFERENCES
- Barnes, A. (2004). Race, schizophrenia, and admission to state psychiatric hospitals. Administration and Policy in Mental Health, 31, 241–252.
- Blow, F. C., Zeber, J. E., McCarthy, J. F., Valenstein, M., Gillon, L., & Bingham, C. R. (2004). Ethnicity and diagnostic patterns in veterans with psychoses. Social Psychiatry and Psychiatric Epidemiology, 39, 841–851.
- Daumit, G. L., Crum, R. M., Guallar, E., Powe, N. R., Primm, A. B., Steinwachs, D. M., et al. (2003). Outpatient prescriptions for atypical antipsychotics for African Americans, Hispanics, and whites in the United States. Archives of General Psychiatry, 60, 121–128.
- DelBello, M. P., Lopez-Larson, M. P., Soutullo, C. A., & Strakowski, S. M. (2001). Effects of race on psychiatric diagnosis of hospitalized adolescents: A retrospective chart review. Journal of Child and Adolescent Psychopharmacology, 11(1), 95–103.
- Herbeck, D. M., West, J. C., Ruditis, I., Duffy, F. F., Fitek, D. J., Bell, C. C., et al. (2004). Variations in use of second-generation antipsychotic medication by race among adult psychiatric patients Psychiatric Services, 55(6), 677–684.