Substances of abuse, such as alcohol, cannabis, cocaine, and narcotics, can contribute to phenocopies of depression on the basis of acute use, chronic use, or discontinuation. Importantly, the discontinuation of two "legal" substances very commonly used by schizophrenia patients--nicotine and caffeine--can lead to withdrawal states that can mimic depression (Lavin et al. 1996). In particular, "smoke-free" and "decaf" policies on many inpatient units can lead to diagnostic confusion unless the possibility of withdrawal symptoms is considered in the differential diagnosis of "depressive" states.
Negative Symptoms of Schizophrenia
Conceptually, the presentation of negative symptoms in patients with schizophrenia overlaps with the syndrome of depression in a number of domains (Andreasen and Olsen 1982; Bermanzohn and Siris 1992; Carpenter et al. 1985; Crow 1980; Siris et al. 1988a). Overlapping symptoms include poor energy, diminished interest, lack of pleasure, lowered drive state, reduced motor activity, impaired concentration, and general sense of helplessness. Other symptoms, however, may be helpful in making the distinction (Barnes et al. 1989; Kuck et al. 1992; Lindenmayer et al. 1991; Norman and Malla 1991). ....
Incidence and Prevalence of Depression in Patients With Schizophrenia
More than two dozen studies have been published examining the rates of occurrence of depression in the course of schizophrenia (Koreen et al. 1993; Sands and Harrow 1999; Siris 1991, 1995; Tapp et al. 1994). They have varied considerably in terms of a number of methodological considerations: the definition employed for schizophrenia, the definition used for depression, the interval surveyed, the methodology of the survey, and the patients' treatment status at the time of the observation. The most notable conclusion that can be drawn from these studies is that, no matter what definitions and conditions prevail, at least some meaningful rate of phenotypic depression is observed in the course of schizophrenia.
Among these studies, the rates of depression varied from a low of 7% in a cross-sectional assessment of patients with DSM-III-defined schizophrenia who were chronically hospitalized and in whom an effort was made to distinguish depression from negative symptoms (Hirsch et al. 1989), to a high of 75% for at least one positive assessment of depression by either one of two criteria among patients with "first break" RDC-defined schizophrenia who were evaluated on a weekly to monthly basis for up to 5 years (Koreen et al. 1993). The modal rate for all these studies was 25%, a fair benchmark that has endured through the course of a number of reviews (Johnson 1981b; Mandel et al. 1982; McGlashan and Carpenter 1976b; Siris 1991, 1995; Winokur 1972).
Since depression is observed more frequently in females among people without schizophrenia (Kessler et al. 1993), and since the expression of schizophrenia in general is different in women than it is in men in a number of ways (Goldstein and Link 1988), it would be interesting to know if sex differences are observed with regard to the presentation of depression in patients with schizophrenia (Goldstein and Tsuang 1990; Seeman 1997). Indeed, such differences, if found, would have theoretical nosological implications ... 
Treatment Strategies
An appropriate treatment approach to depression begins with a consideration of the differential diagnostic possibilities outlined earlier in this chapter. Obviously, since there are no available biological tests (except for the medical/organic conditions), or even psychological tests, that are known to be informative in drawing these diagnostic distinctions, these diagnoses must be made on a purely clinical basis. 
Vulnerability, Stress, and Psychiatric Diatheses: A Hypothetical Model
Figure 2�1 depicts an integrative schema that conceptualizes the interplay of extrinsic and intrinsic factors with the schizophrenia diathesis. The basis for this formulation is the familiar stress-diathesis model of schizophrenia (Nuechterlein and Dawson 1984; Zubin and Spring 1977), supported by more recent understanding of the neuropsychological underpinnings of the pathophysiology of schizophrenia (Weinberger 1987).
In Figure 2�1, the vertical axis represents vulnerability to psychotic symptoms of the schizophrenic type and the horizontal axis depicts the proportion of the general population. At the far left, a tiny fraction of the population manifests a very high vulnerability to psychosis, with an everdecreasing loading for such risk moving to the right along the curve.
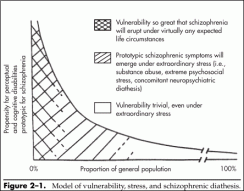 Figure 2�1. Model of vulnerability, stress, and schizophrenic diathesis.
Figure 2�1. Model of vulnerability, stress, and schizophrenic diathesis.
Only a fraction of 1% of the population express a vulnerability so great that a schizophrenic psychosis will emerge under virtually any level of life stress, no matter how minor ... 
References
- Addington D, Addington J, Patten S: Gender and affect in schizophrenia. Can J Psychiatry 41:265-268, 1996
- American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders. Washington, DC, American Psychiatric Association, 1994
- Andreasen NC, Olsen S: Negative vs positive schizophrenia: definition and validation. Arch Gen Psychiatry 39:789-794, 1982
- Atre-Vaidya N, Taylor MA: Effectiveness of lithium in schizophrenia: do we really have an answer? J Clin Psychiatry 50:170-173, 1989
- Bandelow B, Muller P, Gaebel WE: Depressive syndromes in schizophrenic patients after discharge from hospital. Eur Arch Psychiatry Clin Neurosci 240:113-120, 1991
- Barnes TR, Curson DA, Liddle PF, et al: The nature and prevalence of depression in chronic schizophrenic in-patients. Br J Psychiatry 154:486-491, 1989
- Bartels SJ, Drake RE: Depressive symptoms in schizophrenia: comprehensive differential diagnosis. Compr Psychiatry 29:467-483, 1988
- Bartels SJ, Drake RE, McHugo GJ: Alcohol abuse, depression and suicidal behavior in schizophrenia. Am J Psychiatry 149:394-395, 1992
- Becker RE: Implications of the efficacy of thiothixene and a chlorpromazineimipramine combination for depression in schizophrenia. Am J Psychiatry 140:208-211, 1983
- Bermanzohn PC, Siris SG: Akinesia: A syndrome common to parkinsonism, retarded depression, and negative symptoms. Compr Psychiatry 33:221-232, 1992
- Berrios GE, Bulbena A: Post psychotic depression: the Fulbourn cohort. Acta Psychiatr Scand 76:89-93, 1987
- Birchwood M, Mason R, Macmillan F, et al: Depression, demoralization and control over psychotic illness: a comparison of depressed and non-depressed patients with a chronic psychosis. Psychol Med 23:387-395, 1993
- Bland RC, Newman SC, Orn H: Schizophrenia: lifetime co-morbidity in a community sample. Acta Psychiatr Scand 75:383-391, 1987
- Bleuler E: Dementia Praecox, or the Group of Schizophrenias (1911). New York, International Universities Press, 1950
- Bodkin AJ, Cohen BM, Salomon MS, et al: Treatment of negative symptoms in schizophrenia and schizoaffective disorder by selegiline augmentation of antipsychotic medication. J Nerv Ment Dis 184:295-301, 1996
- Bowers MD, Astrachan BM: Depression in acute schizophrenia. Am J Psychiatry 123:976-979, 1967
- Bucci L: The negative symptoms of schizophrenia and the monoamine oxidase inhibitors. Psychopharmacology (Berl) 91:104-108, 1987
- Caldwell CB, Gottesman II: Schizophrenics kill themselves too: a review of risk factors for suicide. Schizophr Bull 16:571-589, 1990
- Carpenter WT Jr, Heinrichs DW, Alphs LD: Treatment of negative symptoms. Schizophr Bull 11:440-452, 1985
- Chien CP, DiMascio A, Cole JD: Antiparkinson agents and depot phenothiazines. Am J Psychiatry 131:86-90, 1984
- Christison GW, Kirch DG, Wyatt RJ: When symptoms persist: choosing among alternative somatic treatments for schizophrenia. Schizophr Bull 17:217-240, 1991
- Coryell W, Keller M, Lavori P, et al: Affective syndromes, psychotic features, and prognosis, I: depression. Arch Gen Psychiatry 47:651-657, 1990
- Crow TJ: Molecular pathology of schizophrenia: more than one disease process? BMJ 280:66-68, 1980
- Davis KL, Kahn RS, Ko G, et al: Dopamine in schizophrenia: a review and reconceptualization. Am J Psychiatry 148:1474-1486, 1991
- DeAlarcon R, Carney MWP: Severe depressive mood changes following slowrelease intramuscular fluphenazine injection. BMJ 3:564-567, 1969
- de Figueiredo JM: Depression and demoralization: phenomenologic differences and research perspectives. Compr Psychiatry 34:308-311, 1993
- Docherty JP, van Kammen DP, Siris SG, et al: Stages of onset of acute schizophrenic psychosis. Am J Psychiatry 135:720-726, 1978
- Drake RE, Cotton PG: Depression, hopelessness and suicide in chronic schizophrenia. Br J Psychiatry 148:554-559, 1986
- Drake RE, Ehrlich J: Suicide attempts associated with akathisia. Am J Psychiatry 142:499-501, 1985
- Dufresne RL, Kass DJ, Becker RE: Buproprion and thiothixene versus placebo and thiothixene in the treatment of depression in schizophrenia. Drug Development Research 12:259-266, 1988
- Eissler KR: Remarks on the psycho-analysis of schizophrenia. Int J Psychoanal 32:139-156, 1951
- Falloon I, Watt DC, Shepherd M: A comparative controlled trial of pimozide and fluphenazine decanoate in the continuation therapy of schizophrenia. Psychol Med 8:59-70, 1978
- Fleischhaker WW, Roth SD, Kane JM: The pharmacologic treatment of neuroleptic-induced akathisia. J Clin Psychopharmacol 10:12-21, 1990
- Floru L, Heinrich K, Wittek F: The problem of post-psychotic schizophrenic depressions and their pharmacological induction. International Pharmacopsychiatry 10:230-239, 1975
- Frank JD: Persuasion and Healing. Baltimore, MD, Johns Hopkins University Press, 1973
- Galdi J: The causality of depression in schizophrenia. Br J Psychiatry 142:621-625, 1983
- Galdi J, Rieder RO, Silber D, et al: Genetic factors in the response to neuroleptics in schizophrenia: a pharmacogenetic study. Psychol Med 11:713-728, 1981
- Goff DC, Midha KK, Sarid-Segal O, et al: A placebo-controlled trial of fluoxetine added to neuroleptic in patients with schizophrenia. Psychopharmacology (Berl) 117:417-423, 1995
- Goldstein JM, Link BG: Gender and the expression of schizophrenia. J Psychiatr Res 22:141-155, 1988
- Goldstein JM, Tsuang MT: Gender and schizophrenia: an introduction and synthesis of findings. Schizophr Bull 16:179-183, 1990
- Goldstein JM, Santangelo SL, Simpson JC, et al: The role of gender in identifying subtypes of schizophrenia: a latent class analytic approach. Schizophr Bull 16:263-275, 1990
- Green MF, Nuechterlein KH, Ventura J, et al: The temporal relationship between depressive and psychotic symptoms in recent-onset schizophrenia. Am J Psychiatry 147:179-182, 1990
- Haas GL, Glick ID, Clarkin JF, et al: Gender and schizophrenia outcome: a clinical trial of an inpatient family intervention. Schizophr Bull 16:277-292, 1990
- Hafner H, Maurer K, Loffler W, et al: The epidemiology of early schizophrenia: influence of age and gender on onset and early course. Br J Psychiatry 164 (suppl 23):29-38, 1994
- Hallonquist JD, Seeman MV, Lang M, et al: Variation in symptom severity over the menstrual cycle of schizophrenics. Biol Psychiatry 33:207-209, 1993
- Halstead SM, Barnes TRE, Speller JC: Akathisia: prevalence and associated dysphoria in an in-patient population with chronic schizophrenia. Br J Psychiatry 164:177-183, 1994
- Harrow M, Yonan CA, Sands JR, et al: Depression in schizophrenia: are neuroleptics, akinesia, or anhedonia involved? Schizophr Bull 20:327-338, 1994
- Heilä H, Isometsä ET, Henriksson MM, et al: A nationwide psychological autopsy study on age- and sex-specific clinical characteristics of 92 suicide victims with schizophrenia. Am J Psychiatry 154:1235-1242, 1997
- Herz M: Prodromal symptoms and prevention of relapse in schizophrenia. J Clin Psychiatry 46 (no 11, sec 2):22-25, 1985
- Herz M, Melville C: Relapse in schizophrenia. Am J Psychiatry 137:801-805, 1980
- Hirsch SR, Gaind R, Rohde PD, et al: Outpatient maintenance of chronic schizophrenic patients with long-acting fluphenazine: double-blind placebo trial. BMJ 1(854):633-637, 1973
- Hirsch SR, Jolley AG, Barnes TRE, et al: Dysphoric and depressive symptoms in chronic schizophrenia. Schizophr Res 2:259-264, 1989
- Hogarty GE, Munetz MR: Pharmacogenic depression among outpatient schizophrenic patients: a failure to substantiate. J Clin Psychopharmacol 4:17-24, 1984
- Hogarty GE, Anderson CM, Reiss DJ, et al: Family psychoeducational, social skills training, and maintenance chemotherapy in the aftercare treatment of schizophrenia, 1: one-year effects of a controlled study on relapse and expressed emotion. Arch Gen Psychiatry 43:633-642, 1986
- Johnson DAW: Depressions in schizophrenia: some observations on prevalence, etiology, and treatment. Acta Psychiatr Scand 63 (suppl 291):137-144, 1981a
- Johnson DAW: Studies of depressive symptoms in schizophrenia. Br J Psychiatry 139:89-101, 1981b
- Johnson DAW: The significance of depression in the prediction of relapse in chronic schizophrenia. Br J Psychiatry 152:320-323, 1988
- Kessler RC, McGonagle KA, Swartz M, et al: Sex and depression in the National
- Comorbidity Survey, I: lifetime prevalence, chronicity, and recurrence. J Affect Disord 29:85-96, 1993
- Klein DF: Endogenomorphic depression: a conceptual and terminological revision. Arch Gen Psychiatry 31:447-454, 1974
- Knights A, Hirsch SR: "Revealed" depression and drug treatment for schizophrenia. Arch Gen Psychiatry 38:806-811, 1981
- Koreen AR, Siris SG, Chakos M, et al: Depression in first episode schizophrenia. Am J Psychiatry 150:1643-1648, 1993
- Kramer MS, Vogel WH, DiJohnson C, et al: Antidepressants in 'depressed' schizophrenic inpatients: a controlled trial. Arch Gen Psychiatry 46:922-928, 1989
- Kuck J, Zisook S, Moranville JT, et al: Negative symptomatology in schizophrenic outpatients. J Nerv Ment Dis 180:510-515, 1992
- Kurland AA, Nagaraju A: Viloxazine and the depressed schizophrenic: methodological issues. J Clin Pharmacol 21:37-41, 1981
- Lavin MR, Siris SG, Mason SE: What is the clinical importance of cigarette smoking in schizophrenia? Am J Addict 5:189-208, 1996
- Leff J, Tress K, Edwards B: The clinical course of depressive symptoms in schizophrenia. Schizophr Res 1:25-30, 1988
- Lerner Y, Mintzer Y, Schestatzky M: Lithium combined with haloperidol in schizophrenic patients. Br J Psychiatry 153:359-362, 1988
- Levitt JJ, Tsuang MT: The heterogeneity of schizoaffective disorder: implications for treatment. Am J Psychiatry 145:926-936, 1988
- Lewine R: Schizophrenia: An amotivational syndrome in men. Can J Psychiatry 30:316-318, 1985
- Lindenmayer J-P, Grochowski S, Kay SR: Schizophrenic patients with depression: psychopathological profiles and relationship with negative symptoms. Compr Psychiatry 32:528-533, 1991
- Mandel MR, Severe JB, Schooler NR, et al: Development and prediction of postpsychotic depression in neuroleptic-treated schizophrenics. Arch Gen Psychiatry 39:197-203, 1982
- Martin RL, Cloninger RC, Guze SB, et al: Frequency and differential diagnosis of depressive syndromes in schizophrenia. J Clin Psychiatry 46 (no 11, sec 2):9- 13, 1985
- McGlashan TH, Bardenstein KK: Gender differences in affective, schizoaffective, and schizophrenic disorders. Schizophr Bull 16:319-329, 1990
- McGlashan TH, Carpenter WT Jr: An investigation of the postpsychotic depressive syndrome. Am J Psychiatry 133:14-19, 1976a
- McGlashan TH, Carpenter WJ Jr: Postpsychotic depression in schizophrenia. Arch Gen Psychiatry 33:231-239, 1976b
- Miles C: Conditions predisposing to suicide. A review. J Nerv Ment Dis 164:221- 246, 1977
- Miller JB, Sonnenberg SM: Depression following psychotic episodes: a response to the challenge of change? J Am Acad Psychoanal 1:253-270, 1973
- Moller HJ, von Zerssen D: Depressive states occurring during the neuroleptic treatment of schizophrenia. Schizophr Bull 8:109-117, 1982
- Moller HJ, von Zerssen D: Handbook of Studies on Schizophrenia. New York, Elsevier, 1986
- Norman RMG, Malla AK: Dysphoric mood and symptomatology in schizophrenia. Psychol Med 21:897-903, 1991
- Norman RMG, Malla AK: Correlation over time between dysphoric mood and symptomatology in schizophrenia. Compr Psychiatry 35:34-38, 1994
- Nuechterlein KH, Dawson MD: A heuristic vulnerability/stress model of schizophrenic episodes. Schizophr Bull 10:300-312, 1984
- Perenyi A, Goswami U, Frecska E, et al: L-Deprenyl in treating negative symptoms of schizophrenia. Psychiatry Res 42:189-191, 1992
- Plasky P: Antidepressant usage in schizophrenia. Schizophr Bull 17:75-98, 1991
- Prasad AJ, Kumar N: Suicidal behavior in hospitalized schizophrenics. Suicide Life Threat Behav 18:265-269, 1988
- Prusoff BA, Williams DH, Weissman MM, et al: Treatment of secondary depression in schizophrenia. Arch Gen Psychiatry 36:569-575, 1979
- Riecher-Rossler A, Hafner H, Stumbaum M, et al: Can estradiol modulate schizophrenic symptomatology? Schizophr Bull 20:203-214, 1994
- Rifkin A, Quitkin F, Klein DF: Akinesia: a poorly recognized drug-induced extrapyramidal behavioral disorder. Arch Gen Psychiatry 32:672-674, 1975
- Rifkin A, Quitkin F, Kane JM, et al: Are prophylactic antiparkinson drugs necessary? Arch Gen Psychiatry 35:483-489, 1978
- Roth S: The seemingly ubiquitous depression following acute schizophrenic episodes, a neglected area of clinical discussion. Am J Psychiatry 127:51-58, 1970
- Roy A: Suicide in chronic schizophrenia. Br J Psychiatry 141:171-177, 1982
- Roy A: Do neuroleptics cause depression? Biol Psychiatry 19:777-781, 1984
- Roy A: Depression, attempted suicide and suicide in patients with chronic schizophrenia. Psychiatr Clin North Am 9:193-206, 1986
- Roy A, Thompson R, Kennedy S: Depression in chronic schizophrenia. Br J Psychiatry 142:465-470, 1983
- Sands JR, Harrow M: Depression during the longitudinal course of schizophrenia. Schizophr Bull 25:157-171, 1999
- Seeman MV: The role of estrogen in schizophrenia. J Psychiatry Neuroscience 21:123-127, 1996a
- Seeman MV: Schizophrenia, gender, and affect. Can J Psychiatry 41:263-264, 1996b
- Seeman MV: Psychopathology in women and men: focus on female hormones. Am J Psychiatry 154:1641-1647, 1997
- Semrad EV: Long-term therapy of schizophrenia: formulation of the clinical approach, in Psychoneuroses and Schizophrenia. Edited by Usdin GP. Philadelphia, PA, JB Lippincott, 1966, pp 155-173
- Shear K, Frances A, Weiden P: Suicide associated with akathisia and depot fluphenazine treatment. J Clin Psychopharmacol 3:235-236, 1983
- Shtasel DL, Gur RE, Gallacher F, et al: Gender differences in the clinical expression of schizophrenia. Schizophr Res 7:225-231, 1992
- Silver H, Nassar A: Fluvoxamine improves negative symptoms in treated chronic schizophrenia: an add-on double-blind, placebo-controlled study. Biol Psychiatry 31:698-704, 1992
- Singh AN, Saxena B, Nelson HL: A controlled clinical study of trazodone in chronic schizophrenic patients with pronounced depressive symptomatology. Current Therapeutics Research 23:485-501, 1978
- Siris SG: Akathisia and "acting-out." J Clin Psychiatry 46:395-397, 1985
- Siris SG: Implications of normal brain development for the pathogenesis of schizophrenia (letter). Arch Gen Psychiatry 45:1055, 1988
- Siris SG: Diagnosis of secondary depression in schizophrenia: implications for DSM-IV. Schizophr Bull 17:75-98, 1991
- Siris SG: Depression and schizophrenia, in Schizophrenia. Edited by Hirsch SR, Weinberger DR. Cambridge, MA, Blackwell Science, 1995, pp 128-145
- Siris SG: The treatment of schizoaffective disorder, in Current Psychiatric Therapy II. Edited by Dunner DL. Philadelphia, PA, WB Saunders, 1996, pp 196-201
- Siris SG: Depression in schizophrenia: perspective in the era of "atypical" antipsychotic agents. Am J Psychiatry 157:1379-1389, 2000
- Siris SG, Lavin MR: Schizoaffective disorder, schizophreniform disorder and acute psychotic disorder (including brief reactive psychosis), in Comprehensive Textbook of Psychiatry/VI, 6th Edition. Edited by Kaplan HI, Sadock BJ. Philadelphia, PA, Williams & Wilkins, 1995, pp 1019-1031
- Siris SG, Morgan V, Fagerstrom R, et al: Adjunctive imipramine in the treatment of post-psychotic depression: a controlled trial. Arch Gen Psychiatry 44:533-539, 1987
- Siris SG, Adan F, Cohen M, et al: Post-psychotic depression and negative symptoms: an investigation of syndromal overlap. Am J Psychiatry 145:1532-1537, 1988a
- Siris SG, Strahan A, Mandeli J, et al: Fluphenazine decanoate dose and severity of depression in patients with post-psychotic depression. Schizophr Res 1:31-35, 1988b
- Siris SG, Bermanzohn PC, Mason SE, et al: Maintenance imipramine therapy for secondary depression in schizophrenia: a controlled trial. Arch Gen Psychiatry 51:109-115, 1994
- Spina E, DeDomenico P, Ruello C, et al: Adjunctive fluoxetine in the treatment of negative symptoms in chronic schizophrenic patients. Int Clin Psychopharmacol 9:281-285, 1994
- Spitzer RL, Endicott J, Robins E: Research Diagnostic Criteria: rationale and reliability. Arch Gen Psychiatry 35:773-782, 1978
- Stephens JH, Richard P, McHugh PR: Suicide in patients hospitalized for schizophrenia: 1913-1940. J Nerv Ment Dis 187:10-14, 1999
- Strian F, Heger R, Klicpera C: The time structure of depressive mood in schizophrenic patients. Acta Psychiatr Scand 65:66-73, 1982
- Szymanski HV, Simon J, Gutterman N: Recovery from schizophrenic psychosis. Am J Psychiatry 140:335-338, 1983
- Tapp A, Tandon R, Douglass A, et al: Depression in severe chronic schizophrenia. Biol Psychiatry 35:667, 1994
- Taylor MA: Are schizophrenia and affective disorder related? A selective literature review. Am J Psychiatry 149:22-32, 1992
- Tollefson GD, Andersen SW, Tran PV: The course of depressive symptoms in predicting relapse in schizophrenia: a double-blind, randomized comparison of olanzapine and risperidone. Biol Psychiatry 46:365-373, 1999
- Van Putten T: The many faces of akathisia. Compr Psychiatry 16:43-47, 1975
- Van Putten T, May PRA: 'Akinetic depression' in schizophrenia. Arch Gen Psychiatry 35:1101-1107, 1978
- Waehrens J, Gerlach J: Antidepressant drugs in anergic schizophrenia: a doubleblind cross-over study with maprotiline and placebo. Acta Psychiatr Scand 61:438-444, 1980
- Weinberger DR: Implications of normal brain development for the pathogenesis of schizophrenia. Arch Gen Psychiatry 44:660-669, 1987
- Winokur G: Family history studies, VIII: secondary depression is alive and well, and . . . Diseases of the Nervous System 33:94-99, 1972
- Wise RA: Neuroleptics and operant behaviour: the anhedonia hypothesis. Behav Brain Sci 5:39-87, 1982
- Wistedt B, Palmstierna T: Depressive symptoms in chronic schizophrenic patients after withdrawal of long-acting neuroleptics. J Clin Psychiatry 44:369-371, 1983
- World Health Organization: International Classification of Diseases (ICD-10): Clinical Descriptions and Diagnostic Guidelines (draft of field trials). Geneva, World Health Organization, 1988
- Zubin J, Spring B: Vulnerability: a new view of schizophrenia. J Abnorm Psychol 86: 103-126, 1977
![]()
![]()
![]()
![]()
 Figure 2�1. Model of vulnerability, stress, and schizophrenic diathesis.
Figure 2�1. Model of vulnerability, stress, and schizophrenic diathesis.
![]()


