Non-pharmacological treatment of Childhood obesity
We recommend that children with BMI higher than the 95th percentile, or higher than the 85th percentile when accompanied by comorbidities, such as hypertension, hyperlipidaemia, or impaired glucose tolerance, be considered for treatment. Non-pharmacological approaches should be the foundation of all obesity treatments, especially in children, and should always be considered as first-line therapy. In a systematic review109 of randomised controlled trials of treatments for childhood obesity, investigators identified 64 trials, 54 of which assessed non-pharmacological lifestyle interventions.
These trials were generally of small sample size (16 to 218 participants), with 70% including fewer than 30 participants. Most trials had substantial methodological limitations and short-term follow-up. Despite these limitations, the investigators concluded that “...this review shows that family-based, lifestyle interventions with a behavioural program aimed at changing diet and physical activity and thinking patterns provide significant and clinically meaningful decreases in overweight in both children and adolescents…in the short- and the long-term”. These findings are encouraging and provide useful guidance for treatment of obese children, but they also emphasise the need for additional large randomised controlled trials with long-term follow-up.
A catabolic state of stored energy is needed to induce weight loss. Guidelines from the American Academy of Pediatrics recommend that weight-reducing diets contain “less energy than that required to maintain weight but not less than 1200 kilocalories a day.”110 Equivalent UK guidance emphasises energy balance between intake and expenditure, but does not specify amounts of intake.111
Another recommended approach is to construct a diet that is 300-400 kcal per day lower than weight-maintenance requirements as assessed by dietary history or as calculated on the basis of a formula relating anthropometry to energy expenditure, such as the Harris-Benedict equation. In view of the magnitude of the energy gap, a sizeable energy deficit would be needed to induce appreciable weight reduction in an obese child, and many weight-loss diets might be energy neutral in young children or even lead to weight gain in sedentary female adolescents.88,90
Some guidelines (eg, in the UK) and commentators emphasise behavioural strategies that do not specify actual caloric intake. Results of a randomised trial of behavioural treatment without specified calorie limits showed no effect on BMI.112,113 A protein-sparing modified fast has a very low calorie regimen (600-800 kcal per day) and seems to be promising, but this notion has not progressed since it was first reported.114 Transient growth deceleration was recorded, but growth returned to normal by 14 months.115 However, this trial was not randomised and had few follow-up data.
Promotion of increased energy expenditure for weight reduction has not received the same attention as have dietary prescriptions. We found only one randomised controlled trial of 6-11-year-old obese children that compared hypocaloric diet, 90 min of moderate exercise 3 days per week, or both. Weight loss was greater in the diet or diet-plus-exercise group (being similar in these two) than in the exercise-only group, but there was no control group and follow-up lasted only 9 months.116
Interventions to decrease sedentary activity, such as restriction of television viewing, have been examined and are promising.117
The macronutrient composition of diets has been examined for differential weight-loss benefits. Several popular diets, including Atkin’s, have emphasised increasing protein intake, but not changing energy content. Although some results show increased weight loss with this diet in adults,118-120 data from long-term studies generally show no difference in weight loss between diets of varying macronutrient contents that do not change total energy intake.121,122
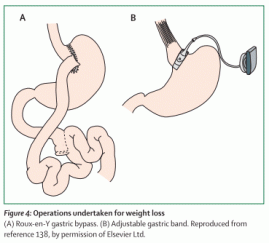 Figure 4: Operations undertaken for weight loss
Figure 4: Operations undertaken for weight loss
(A) Roux-en-Y gastric bypass. (B) Adjustable gastric band. Reproduced from reference 138, by permission of Elsevier Ltd.
Demol and colleagues121 reported no differences in BMI decrease in obese adolescents on different macronutrient diets.