Prevention of Childhood obesity
Prevention, especially in young people, is universally viewed as the best approach to reverse the rising global prevalence of obesity. However, evidence about the most effective means of prevention of obesity development in children is scarce. Many prevention trials have had sample sizes too small for expected effect size or insuficient length of follow-up. Some trials have also been criticised for not being based on sound theories of behavioural change and for having inadequate feasibility and pilot work.87
Trials of prevention interventions might also have failed to show notable effects because they did not adequately address the energy gap88 separating children who remain lean from those who gain weight throughout childhood.89 Butte and Ellis90 calculated that an energy deficit of more than 250 kcal per day is needed to prevent further weight gain in 90% of overweight children; this deficit is equivalent to a child walking an additional 1-2 h per day at 1·9 km/h, or consuming roughly a fifth fewer calories than usual per day.
Prevention measures can be instituted at individual, household, institutional, community, and health-care levels. At the individual level, carers should be targeted rather than young children themselves, and focus on mothers seems reasonable. First, developmental or fetal overnutrition as a result of gestational diabetes or maternal obesity might have contributed to the obesity epidemic.
So far, no intervention studies have examined the long-term effect of reduction of gestational diabetes or maternal adiposity on future obesity risk in offspring. Second, breastfeeding might prevent childhood obesity. However, results of systematic reviews suggest that observational associations could be accounted for largely by residual confounding or publication bias, and in a large randomised trial of a breastfeeding promotion intervention, no causal effect of breastfeeding on obesity risk was reported.91
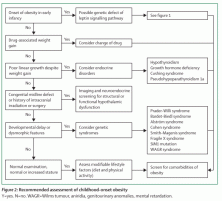 Figure 2: Recommended assessment of childhood-onset obesity
Figure 2: Recommended assessment of childhood-onset obesity
Y=yes. N=no. WAGR=Wilms tumour, aniridia, genitourinary anomalies, mental retardation.
Third, mothers might influence diets of offspring more than do fathers;92 however, no intervention trials of maternal-only interventions to prevent childhood obesity have been done.
At a household or family level, encouragement of parents to offer appropriate food portions, foster physical activity, increase activities of daily living, and keep sedentary behaviours to a minimum are viewed as basic measures of prevention.93 Most government guidelines have traditionally focused on ensuring that nutritional intake is adequate.94
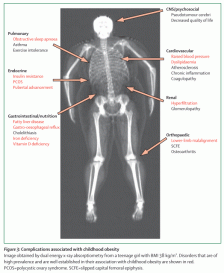 Figure 3: Complications associated with childhood obesity
Figure 3: Complications associated with childhood obesity
Image obtained by dual energy x-ray absorptiometry from a teenage girl with BMI 38 kg/m². Disorders that are of high prevalence and are well established in their association with childhood obesity are shown in red. PCOS=polycystic ovary syndrome. SCFE=slipped capital femoral epiphysis.
However, these guidelines might not be useful to ensure energy intakes that are appropriate for contemporary sedentary lifestyles. We are unaware of any randomised controlled trials focusing solely on household or family-based interventions to prevent childhood obesity.
Most randomised prevention trials have taken place in schools since they are viewed as a universal catchment setting for children. The core features of most prevention programmes are to change the caloric content of school meals and encourage physical activity. One policy that is debated in the USA is removal of vending machines from schools to curb availability of energy-dense snack foods.
However, a US national survey showed that snack foods from vending machines contributed only 1·3% of total daily calories from snacks, whereas snacks at or from home contributed 69·1%.95 At least nine systematic reviews have examined randomised controlled trials of school-based childhood obesity prevention programmes87,96 (see also citations of other systematic reviews within these reports).
Early reviews noted scarce evidence of effectiveness and poor quality of studies, whereas more recent reviews suggested that school-based interventions might be effective. Gonzalez-Suarez and colleagues96 identified 19 high-quality trials of school-based interventions and reported reduced odds of overweight or obesity in intervention compared with control groups (pooled odds ratio 0·74 [95% CI 0·60-0·92]). The key effective characteristics of such programmes remain to be established, and, since most studies were done in the USA, whether they are effective elsewhere. Although initiatives have also been aimed at children in kindergarten or nurseries,97 the few controlled trials in this setting have not yet been systematically reviewed. One area to be addressed is the built environment of schools or nurseries.