Differential diagnosis and complications of Childhood obesity
Endocrine diseases, congenital and acquired hypothalamic defects, genetic syndromes, and use of drugs affecting appetite should be considered during assessment of paediatric patients with obesity (figure 2).
Clinical history and examination should guide differential diagnosis. Onset of obesity during early infancy raises suspicion of function-changing genetic mutations affecting the leptin signalling pathway, but these disorders are very rare, with the most common, melanocortin-4-receptor defects, affecting less than 5% of children with early-onset obesity.56
During assessment of new-onset excessive weight gain, potential side-effects from a recently initiated drug should be taken into consideration, because weight gain can be associated with administration of insulin or insulin secretagogues, glucocorticoids, hormonal contraceptives (eg, depot medroxyprogesterone acetate), psychotropic drugs (including atypical antipsychotics [eg, clozapine, olanzapine, risperidone], mood stabilisers [eg, lithium], tricyclic antidepressants [eg, amitriptyline, imipramine, and nortriptyline], and anticonvulsants [eg, valproic acid, gabapentin, and carbamazepine]), antihypertensive drugs (eg, propranolol and clonidine), and antihistamines.65 In patients with decreased growth velocity despite continued weight gain, an endocrinopathy should be considered; measurement of thyroidstimulating hormone and free thyroxine and referral to a paediatric endocrinologist are recommended.
Almost all patients, however, do not have any of these identifiable disorders. All patients, irrespective of cause of obesity, should be assessed for modifiable lifestyle factors, including physical activity and diet, and screened for complications of obesity, including measurement of lipid and glucose concentrations after overnight fasting, and alanine aminotransferase. If fasting glucose concentration is 5.6 - 6.9 mmol/L, an oral glucose tolerance test is recommended. Screening for vitamin D and iron deficiency should also be considered.
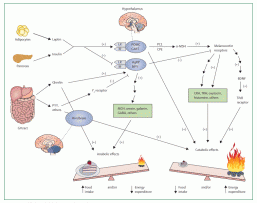 Figure 1A simplified model of the leptin signalling pathway
Figure 1A simplified model of the leptin signalling pathway
Lines with arrowheads show stimulatory action. Lines with perpendicular endblocks show inhibitory action. AgRP=agouti-related protein. BDNF=brain-derived neurotrophic factor. CART=cocaine-amphetamine related transcript. CPE=carboxypeptidase E. CRH=corticotropin-releasing hormone. GABA=gamma amino butyric acid.
GI=gastrointestinal. IR=insulin receptor. LR=leptin receptor. MCH=melanin-concentrating hormone. MSH=melanocyte-stimulating hormone. NPY=neuropeptide Y.
PC1=prohormone convertase 1. POMC=pro-opiomelanocortin. PYY=peptide YY. TRH=thyrotropin-releasing hormone. TrkB=tropomyosin receptor kinase B.
Childhood obesity can adversely affect almost every organ system (figure 3) and often has serious consequences, including hypertension, dyslipidaemia, insulin resistance or diabetes, fatty liver disease, and psychosocial complications.66 Results of one study showed that being overweight or obese between ages 14 and 19 years was associated with increased adult mortality (from age 30 years) from various systemic diseases.67 The atherosclerotic process68 seems to be accelerated in obese children and almost half of children with BMI higher than the 97th percentile have one or more of the disorders that make up the metabolic syndrome.69 High childhood and adolescent BMI is associated with increased risk of cardiovascular disease in adulthood.70 Pulmonary disorders, including obstructive sleep apnoea and reactive airway disease,71 are reported more frequently in obese children than in their normal-weight counterparts. Asthma severity, however, does not seem to be affected by obesity;72 weight-related but non-asthmatic airflow limitations are perhaps being misdiagnosed as asthma in some obese children.73 Specific nutritional deficiencies often accompany childhood obesity. High BMI and adiposity have been associated with low vitamin D concentrations in children.74
The mechanism underlying low vitamin D concentrations in obesity is unclear, but increased storage of vitamin D in adipose tissue has been proposed.75 Overweight or obese children are also at least twice as likely to be iron-deficient than children of normal weight.76 Obesity leads to increased production of proinflammatory cytokines that in turn promote release of hepcidin, which is a peptide hormone produced by the liver and adipocytes that decreases iron absorption from the gut.77
Complications of childhood obesity include acceleration in timing of thelarche and menarche in girls,78,79 pubertal advancement in boys80 and adverse effects on maturation81 and alignment82 of developing bones in both sexes.
Advanced skeletal maturation has been attributed to increased adipose tissue aromatisation of weak androgens into more potent oestrogens. Obesity might also affect pubertal timing through nutrition-related signals (eg, insulin and leptin) on the reproductive axis.83
Orthopaedic complaints, including fractures, musculoskeletal discomfort, impaired mobility, and lower-limb mal alignment seem to be more common in obese children than in those who are not overweight.82 Serious orthopaedic complications of childhood obesity are tibia vara (Blount’s disease or adolescent bowing of the legs)84 and slipped capital femoral epiphyses.85 By contrast, however, obesity might have some beneficial effect on bone mineral density.
Results of a recent study, using variation in the FTO gene as an instrumental variable, suggested that high fat mass in children was causally associated with increased total, spinal, and limb bone mineral content.86
###
Joan C Han, Debbie A Lawlor, Sue Y S Kimm
Lancet 2010; 375 - 1737-48
Published Online May 6, 2010 DOI - 10.1016/ S0140- 6736(10)60171-7
Unit on Growth and Obesity, Program on Developmental Endocrinology and Genetics, Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institutes of Health, DHHS, Bethesda, MD, USA (J C Han MD); MRC Centre for Causal Analyses in Translational Epidemiology, Department of Social Medicine, University of Bristol, Bristol, UK (Prof D A Lawlor PhD); and Department of Internal Medicine/Epidemiology, University of New Mexico School of Medicine, Albuquerque, NM, USA (S Y S Kimm MD)
Correspondence to - Dr Sue Y S Kimm, University of New Mexico Health Sciences Center, Department of Internal Medicine/Epidemiology, University of New Mexico, MSC 10 5550 Albuquerque, NM 87131-0001, USA .(JavaScript must be enabled to view this email address)
###
REFERENCES
- Ebbeling CB, Pawlak DB, Ludwig DS. Childhood obesity: public-health crisis, common sense cure. Lancet 2002; 360: 473-82.
- Wang Y, Lobstein T. Worldwide trends in childhood overweight and obesity. Int J Pediatr Obes 2006; 1: 11-25.
- Ogden CL, Carroll MD, Flegal KM. High body mass index for age among US children and adolescents, 2003-2006. JAMA 2008; 299: 2401-05.
- Kipping RR, Jago R, Lawlor DA. Obesity in children. Part 1: epidemiology, measurement, risk factors, and screening. BMJ 2008; 337: a1824.
- Sundblom E, Petzold M, Rasmussen F, Callmer E, Lissner L. Childhood overweight and obesity prevalences levelling off in Stockholm but socioeconomic differences persist. Int J Obes (Lond) 2008; 32: 1525-30.
- Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240-43.