Schizophrenia and Neurotransmitters
When scientists study how the brains of people with mental illness are different, they are commonly interested in two issues: brain structure and function. Researchers can study structure by comparing the brain anatomy in people with schizophrenia to brain anatomy in people without schizophrenia. Ventricle size is a good example of a structural anatomical difference seen in schizophrenia, whereas frontal lobe activity is a good example of a functional anatomical difference seen in schizophrenia.
Another area of interest to researchers is communication within the brain. Studying communication in the brain, a process carried out by substances called neurotransmitters, can help reveal even more about how the brains of people with schizophrenia differ from the brains of people without it. Studying neurotransmitters can reveal both structural and functional differences in the schizophrenic brain. Next, we will discuss how neurotransmitters work and how they appear to be implicated in schizophrenia symptoms.
Neurotransmitters. Neurotransmitters are effectively the “messengers” of the brain, carrying information from one brain cell to another.
Brain cells, called neurons, are responsive to different kinds of neurotransmitters and have receptors built specifically for them. Neurons that are sensitive to specific neurotransmitters tend to cluster together, creating circuits in the brain for processing specific kinds of information.
Neurotransmitters are released from a neuron when it signals another brain cell. The neurotransmitters are released into the small space between the two neurons, called the synapse. In the synapse, the neurotransmitters attach, or bind, to the receptors at the ends of another neuron, thus affecting the activity of the new neuron. The new neuron takes in as much of the neurotransmitter as it can and then releases the excess back into the synapse. The excess is reabsorbed by the first neuron, a process known as reuptake. Drugs that treat mood disorders like depression (e.g. Prozac, zoloft) regulate the amount of certain neurotransmitters available in the brain and the process of neurotransmitter reuptake, and affect communication between brain cells.
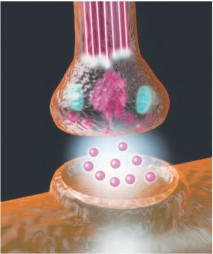 Figure 4.4 This computer graphic of a synapse shows the release of neurotransmitters (pink spheres at lower center) by vesicles inside the synaptic knob (upper center). The neurotransmitters will cross the gap and bond to the receptors of the adjacent cell, which is how information is transmitted along the nervous system. © Alfred Pasieka/Photo Researchers, Inc.
Figure 4.4 This computer graphic of a synapse shows the release of neurotransmitters (pink spheres at lower center) by vesicles inside the synaptic knob (upper center). The neurotransmitters will cross the gap and bond to the receptors of the adjacent cell, which is how information is transmitted along the nervous system. © Alfred Pasieka/Photo Researchers, Inc.
There are many different neurotransmitters in the brain. Two that have been found to be involved in schizophrenia symptoms are dopamine and glutamate. Dopamine is primarily involved in movement and thoughts. Dopamine has also been associated with novelty seeking, or interest in new experiences and reward. Some illegal drugs, such as cocaine and methamphetamine, work by affecting dopamine function in the brain. Thus, dopamine is associated with feelings of pleasure and well-being.
Dopamine pathways in the brain are highly specialized and may influence different kinds of thinking or behavior. People with high levels of dopamine in certain parts of the brain may also experience psychotic symptoms or paranoid thinking, symptoms of schizophrenia.
Due to several lines of converging evidence, many scientists believe that dopamine is the cause of many schizophrenic symptoms. The “dopamine hypothesis” dates from the 1960s and emerged from three important observations. In 1952, a drug called clorpromazine was first used to treat schizophrenia.
It worked by blocking dopamine receptors and was successful in treating many schizophrenia patients. A second observation involved the effects of amphetamines. Amphetamines work by making the brain think that there is too much dopamine in the system. People who abuse amphetamines often experience schizophrenia-like symptoms, primarily paranoia and auditory hallucinations. Parkinson’s disease is a disease in which patients experience physical movement problems.
Patients with Parkinson’s are treated with a drug that effectively increases the level of dopamine in the brain. This drug, called L-DOPA, has been associated with complications or side effects that look a lot like schizophrenic symptoms. Patients treated with L-DOPA sometimes experience psychotic symptoms, which provide researchers with more evidence that high levels of dopamine in some parts of the brain are implicated in schizophrenia.
When the brain perceives that there is an excess of dopamine, schizophrenic-like symptoms appear. We still don’t know what causes this excess of dopamine. Do some people produce too much dopamine? Is the breakdown of dopamine somehow inhibited in some people? Or do some people have dopamine receptors that are especially sensitive so their brain thinks that there is extra dopamine even when there isn’t? These are questions that have yet to be answered definitively.
One problem in studying dopamine in schizophrenia is that we can only directly study the presence of dopamine in autopsies. Presently, we can study the metabolite of dopamine, the substance that remains in the body after dopamine is used.
The metabolite of dopamine, HVA, can be found and measured in our cerebrospinal fluid, which is the fluid we have in our spinal column and in the ventricles of our brain.
In order to measure this fluid, patients must endure a spinal tap, which requires the insertion of a long needle into the spine to access the fluid. This is a painful procedure, and there are risks of infection and complications. Because of these risks, few people are willing to undergo this procedure to be part of an experimental study.
As yet, there is little evidence that people with schizophrenia are producing more dopamine than are people without schizophrenia. Instead, there is some evidence that people with schizophrenia are extremely sensitive to dopamine. Through postmortem studies, researchers have discovered that relative to people without schizophrenia, schizophrenic patients have more receptors for dopamine. Although this evidence is promising, it is unclear whether schizophrenia is caused by an excess of dopamine receptors, or whether the excess of receptors is caused by the illness or treatment.
Another neurotransmitter that may play an important role in schizophrenia is glutamate. Glutamate is believed to have an important role in learning and the formation and encoding of memory. Some hallucinogenic drugs, such as PCP, are known to block glutamate receptors. Like amphetamines, PCP can cause paranoia that mimics schizophrenic symptoms.
When people with schizophrenia take PCP, it often makes their symptoms worse. In autopsy studies, lower levels of glutamate have been found in the brains of schizophrenic patients. Dr. Daniel Weinberger, an influential researcher of schizophrenia at the National Institute of Mental Health, has suggested that an interaction between dopamine and glutamate is at the core of schizophrenia. Dopamine receptors also reduce the action of glutamate. If there are too many dopamine receptors, glutamate’s effects will be blocked.
Studying how neurotransmitters work is especially challenging. However, these investigations can provide crucial information about what causes schizophrenia and how best to treat it.
Heather Barnett Veague, Ph.D.
Heather Barnett Veague attended the University of California, Los Angeles,
and received her Ph.D. in psychology from Harvard University in 2004. She
is the author of several journal articles investigating information processing
and the self in borderline personality disorder. Currently, she is the Director
of Clinical Research for the Laboratory of Adolescent Sciences at Vassar
College. Dr. Veague lives in Stockbridge, Massachusetts, with her husband
and children.
References