Obesity and Mental Illness
Epidemiology
Obesity has reached epidemic proportions in the general population. Current International Obesity Task Force estimates suggest that at least 1.1 billion adults are overweight including 312 million who are obese; this represents a doubling and trebling in less than two decades. Among randomly selected middle-aged participants from 34 populations in 21 countries from the early 1980s to the mid-1990s, mean BMI as well as the prevalence of overweight increased in virtually all Western European countries, Australia, the USA, and China, and was related to increasing trends in total energy supply per capita. Since 1980, the prevalence of obesity in Great Britain in adults has almost trebled with obesity prevalence in 2002 of 23% for men and 25% for women. In the US, obesity prevalence among adults in 2003–2004 was 32%, and the prevalence of extreme obesity (BMI of at least 40) was 2.8% in men and 6.9% in women.
Patients with schizophrenia have higher rates of obesity. Among the patients participating in phase 1 of the randomized and double-blinded 18-month Clinical Antipsychotic Trials of Intervention Effectiveness schizophrenia study (CATIE), the mean BMI was 30. Moreover, waist circumference exceeded norms for 46% of all subjects (n = 1435), 37% of all men (n = 1059), 73% of all women (n = 376), 48% of all Caucasians (n = 858), 43% of all Blacks (n = 504), and 47% of all Hispanics (n = 167).
Contributory Factors
Obesity in Schizophrenia
Overweight and obesity is related to a mismatch between energy intake, expenditure, and storage. A sedentary lifestyle associated with increased intake of high caloric food will lead to increased weight. For example, about 7,800 kcal of chemical energy is contained in 1 kg of adipose tissue so that even a small increase in intake (such as 0.5 liters a day of a sugared carbonated beverage or 200 kcal) can lead to a significant amount of weight gain of 9 kg in one year if these additional calories are not expended but instead stored as fat. The availability of different foods and the amount consumed varies from country to country.
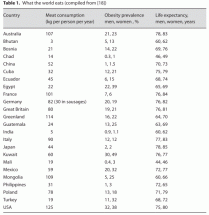 Table 1. What the world eats (compiled from)
Table 1. What the world eats (compiled from)
Table 1 outlines meat consumption, prevalence of obesity, and life expectancy for 24 different countries.
Patients with mental disorders such as schizophrenia may make poor dietary choices. In patients with an increased risk for central adiposity to begin with, this combination of poor diet and lack of physical activity is particularly problematic.
Psychotropic medications such as antipsychotics, antidepressants, and anticonvulsants, have been associated with weight gain. It is not uncommon for these medications to be used in combination.
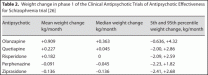 Table 2. Weight change in phase 1 of the Clinical Antipsychotic Trials of Antipsychotic Effectiveness for Schizophrenia trial
Table 2. Weight change in phase 1 of the Clinical Antipsychotic Trials of Antipsychotic Effectiveness for Schizophrenia trial
Possible mechanisms for medication-associated weight gain include weight loss before drug treatment, food craving, alteration in resting metabolic rate, sedation/decreased physical activity, change in neurotransmitters (in general, alpha-adrenergic neurotransmission is thought to stimulate appetite, whereas beta-adrenergic, histaminergic, dopaminergic, and serotoninergic signal transduction confers satiety) and alteration of neuropeptides such as leptin and cytokines such as tumor necrosis factor.